An algorithm to improve the accuracy of emergency weight estimation in obese children
Mike Wells, Lara Nicole Goldstein
Corresponding author: Lara Nicole Goldstein, Division of Emergency Medicine, Faculty of Health Sciences, University of the Witwatersrand, Johannesburg, South Africa 
Received: 06 Sep 2017 - Accepted: 25 Sep 2018 - Published: 05 Oct 2018
Domain: Emergency medicine,Urgent Care Medicine,Pediatrics (general)
Keywords: Body weight, resuscitation, pediatric obesity
©Mike Wells et al. Pan African Medical Journal (ISSN: 1937-8688). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Mike Wells et al. An algorithm to improve the accuracy of emergency weight estimation in obese children. Pan African Medical Journal. 2018;31:90. [doi: 10.11604/pamj.2018.31.90.13821]
Available online at: https://www.panafrican-med-journal.com//content/article/31/90/full
Original article 
An algorithm to improve the accuracy of emergency weight estimation in obese children
An algorithm to improve the accuracy of emergency weight estimation in obese children
Mike Wells1, Lara Nicole Goldstein1,&
1Division of Emergency Medicine, Faculty of Health Sciences, University of the Witwatersrand, Johannesburg, South Africa
&Corresponding author
Lara Nicole Goldstein, Division of Emergency Medicine, Faculty of Health Sciences, University of the Witwatersrand, Johannesburg, South Africa
Introduction: during medical emergencies in children, accurate and appropriate weight estimations may ultimately influence the outcome by facilitating the delivery of safe and effective doses of medications. Children at the extremes of habitus, especially obese children, are more at risk of an inaccurate weight estimation and therefore may be more at risk of medication errors. The objective was therefore to develop an algorithm to guide accurate emergency weight estimation in obese children.
Methods: relevant medical evidence was reviewed regarding weight estimation and its role and timing in the resuscitation of obese children. This was used as the basis for a weight-estimation algorithm.
Results: there was limited evidence regarding the way the weight-estimation systems should be used in obese children other than that the dual length- and habitus-based systems were the most accurate. The methods included in the algorithm were the Broselow tape, the Mercy method, parental estimates, the paediatric advanced weight prediction in the emergency room/ eXtra Length-eXtra Large (PAWPER XL) tape and the Traub-Johnson formula. The algorithm recognised several ways in which weight estimation could be tailored to the clinical scenario to estimate both ideal and total body weight.
Conclusion: weight-estimation in obese children must be conducted appropriately to avoid medication errors. This algorithm provides a framework to achieve this.
The process of weight estimation during the management of paediatric emergencies is very important. Failure to obtain an early and accurate weight estimate may be a major impediment to resuscitative care for two reasons: firstly, the process of obtaining a weight estimation may cause uncertainty and delay which will prevent the timely administration of necessary medications as well as other weight-dependent interventions (e.g. defibrillation); secondly, inaccurate weight estimation may result in dosage errors, with the resultant potential for patient harm [1]. Failure to obtain a timeous, accurate and appropriate weight estimation must be considered a medical error [2]. Ultimately, the accuracy of the weight estimation may determine the efficacy and safety of resuscitative drug treatment and failure to achieve accurate dosing may lead to increased mortality, especially in obese or underweight children who are at highest risk of inaccurate weight estimations [3]. There is a wealth of evidence to support the use of the newer dual length- and habitus-based weight-estimation systems when weight cannot be measured in an emergency. The most-studied examples of these systems are the Mercy method and the PAWPER (or PAWPER XL) tape. The older, one dimensional age- or length-based methodologies have been superseded, primarily because of their inaccuracy but also because of the cognitive burden they can impose on the treating healthcare professional [4]. Not only is the accuracy of weight estimation important, but the method as well as the ease with which it is obtained is crucial.
�
With the increasing prevalence of obesity in low-, middle- and high-income countries, healthcare providers may well be faced with children of vastly different body habitus and body composition in the resuscitation room. The use of weight estimation methods that estimate only total body weight (TBW) may not be sufficient for all children, since obese children require an estimation of ideal body weight (IBW) in addition, for certain drug dose calculations [5]. The use of IBW alone would also not be appropriate as TBW is still required for many dose calculations in obese children. For normal weight and underweight children TBW is used for all drug dose calculations. In underweight children IBW might far exceed TBW, which could result in a dangerous overdose of potentially harmful medications [6].�
How the estimation of TBW and IBW should be accomplished during emergency care in obese children, in a manner that is accurate, safe and easy-to-perform, has not previously been considered. There is limited evidence on the harmful effects of dosage errors resulting from poor weight estimation during resuscitative care, but it cannot be considered to be good medical practice to tolerate significant medication errors resulting from inaccurate or inappropriate weight estimations [7]. It would be useful, therefore, to establish guidelines on how to approach weight estimation at the time of initiation of emergency medical care in obese children. The aim of this study was to create an evidence-based algorithm for weight estimation, to be employed during the management of medical emergencies in children, with a focus on how weight estimation should be achieved in obese children. The constraints were that the accuracy, ease-of-use and time-to-completion of weight estimation had to be balanced against the potential for aggravating the cognitive load, which could impact negatively on resuscitative care.
Search strategy
�
An online search using Scopus, MEDLINE, Google Scholar and Google was conducted using the following search terms: �paediatric weight estimation�, �weight estimation children�, �Broselow tape�, �Mercy method� and �resuscitation aid�. The articles were screened to retrieve relevant information on the accuracy of weight estimation systems, the performance of weight estimation systems in obese and underweight children specifically, the requirements for training with existing weight-estimation systems and the performance of weight estimation systems under stressful conditions.�
Creation of the algorithm�
The algorithm was created with the emergency interventions that might be required for three common emergency scenarios in mind: a child in cardiac arrest, a child that required urgent airway management and a child with convulsive status epilepticus. The algorithm was also developed with the objective of optimising weight estimation for all children, including obese and underweight children, to facilitate safe and accurate drug dose determination.
There was very little evidence on any aspect of weight estimation other than accuracy. A summary of the evidence is shown in Table 1.
�
Summary of findings used to create the algorithm�
Information on weight estimation in obese children was very sparse with only low-grade evidence available. The relevant evidence could be divided into two main groups of findings, as summarised below.�
What are the most appropriate dose scalars for obese children?�
Several recent reviews have provided some guidance about appropriate dosing of emergency medications in obese children. Although there is some difference between anaesthetic and emergency medicine dosing, the principles of which weight descriptors should be used have been well elucidated [5, 8, 9]. In obese children, lipophilic drugs�which account for about half of the drugs that are commonly-used during paediatric emergencies�should generally be dosed using TBW as a scalar or weight descriptor. Hydrophilic drugs should be dosed to IBW in obese children to avoid overdosing if dosed to TBW [5]. Some drugs, such as phenytoin, require an intermediate dosing scalar to achieve optimum dosing. This adjusted body weight (ABW) is generally calculated from TBW, IBW and a defined constant.�
Which weight estimation systems are the most accurate in obese children?�
Age-based formulas: the evidence was very clear that age-based formula estimations of TBW are very inaccurate in all children�even more so in obese children�and should not be used. Formulas are also hard to remember and even the simplest calculations are vulnerable to errors during emergencies [10]. There is some preliminary evidence that some age-based formulas, especially the European Paediatric Life Support formula may be useful to estimate IBW [11].�
Length-based formulas: the Traub-Johnson and Traub-Kichen formulas have not been shown to estimate TBW with acceptable accurately, but can predict IBW with a high degree of accuracy [12].�
Broselow tape: the tape has been shown to be inaccurate in both underweight and obese populations, with potentially deleterious effects on patient safety [13, 14]. The tape does predict IBW with a great deal of accuracy, however [15].�
Guesses and estimations: the use of healthcare providers� guesses of TBW to calculate drug doses have been shown to be grossly inaccurate and potentially harmful to children [7, 16]. There is no evidence on the ability of healthcare providers to estimate IBW. Parental estimates of TBW can be very accurate [13]. Parental estimates may not be as accurate in overweight and obese children as in normal weight children, however, unless the parent can recall the result of a recently scale-measured weight [17].�
Dual length- and habitus-based systems: from the evidence, it appears that accurate TBW estimation can be best achieved using two-dimensional, dual length- and habitus-based systems such as the Mercy method and the PAWPER or PAWPER XL tape, especially in obese and underweight children. These systems are far more accurate than other, older systems [18]. Accurate IBW estimation can be achieved using the Broselow tape, the PAWPER or PAWPER XL tape and the length-based formulas (such as the Traub-Johnson formula) [19].�
Algorithm�
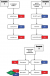
The hierarchy of the preferred weight estimation methodologies is shown in the Figure 1. The devised algorithm is shown in Figure 2, with accompanying notes in Table 2. A description of the weight estimation systems included in the algorithm is contained in Figure 3.
This is the first article to suggest a methodology to guide the practice of weight estimation in obese children, which is more complex than in non-obese children. Even though medication errors in children have been shown to be common and serious, little work has been done to evaluate how inaccuracies in weight estimation contribute to these errors and how this could be improved, especially in obese children [2, 20].
�
Appropriate dose scalars for obese children�
Estimates of both TBW and IBW are required to permit safe and effective drug dosing in obese children. This has received little attention in emergency weight-estimation studies, but it is important as, notwithstanding the emergency nature of any presentation, it is imperative that medication errors be minimised. With the high prevalence of childhood obesity in high-, middle- and low-income countries, it is not uncommon that obese children will present with conditions that require urgent treatment. Errors in the selection of the dosing scalar for drug dose calculations could result in a significant dose error. The inappropriate use of TBW for hydrophilic drugs could cause significant overdosing and potential resultant harm. The inappropriate use of IBW for lipophilic medications would result in a significant underdosing, with potential diminished effectiveness of drug treatment and potential harm � e.g. the failure to rapidly abort seizures in status epilepticus with inadequate doses of valproate. It is important to recognise that IBW should not be used for non-obese children. Although IBW and TBW are similar for children around the 50th centile of weight-for-length, IBW should definitely not be used for thin or underweight children as IBW will exceed TBW and may result in a dangerous overdosing of medications [21].�
Figure 4 demonstrates the different weight scalars required during emergency medical management of an obese child in three common emergency scenarios. These scenarios illustrate not only the importance of estimating both TBW and IBW, but also how early these estimates are required after the initiation of emergency care. The first scenario a child in cardiac arrest illustrates the need for TBW for determination of defibrillation doses and for doses of lipophilic medications (e.g. amiodarone). The correct management for a child presenting with ventricular fibrillation (VF) would be immediate defibrillation. A measure of TBW would therefore be required immediately to enable the calculation of the correct defibrillation energy dose. The initial dose of amiodarone would be required four to five minutes into the resuscitation. IBW is required to scale doses of hydrophilic medications (e.g. epinephrine) � dosing these medications to TBW carries a high risk of morbidity in obese children. Since the correct management of a child with a cardiac arrest would require the administration of epinephrine within two to four minutes of the initiation of the resuscitation, an accurate estimation of IBW would be required very early in the process to facilitate correct dose calculation.�
The second scenario illustrates a similar requirement to have estimations of both TBW and IBW to allow for optimum drug dosing. While IBW is not directly useful for determining equipment size, length is. Therefore, the non-habitus-modified weight (IBW) is more useful to determine equipment size than a habitus-modified TBW estimation. In this scenario, where rapid airway management is required, drug doses would need to be determined immediately to allow for their preparation during the period of pre-oxygenation. There would be very little leeway for delay in obtaining estimates of both TBW and IBW to allow for optimum management.�
The third scenario, an obese child with status epilepticus, illustrates further complexities in drug dose calculation. As in the other scenarios, both TBW and IBW estimations are required within the first few minutes of initiating emergency care � there is no time for delay. Anticonvulsant medications must be dosed according to TBW or IBW depending on their individual pharmacokinetic properties. When anti-epileptic medications are administered, doses also need to be individualised: some drugs, such as phenytoin, are best dosed to an adjusted body weight (ABW) for which estimations of both TBW and IBW are required. Other drugs, such as valproate, must be dosed to TBW.�
Weight estimation in obese children�
The decision on which weight estimation methods to include in the algorithm depended primarily on their established accuracy. Their role within the framework of the algorithm was determined primarily by how they function and how easy they are to use. The dual length- and habitus-based systems are significantly more accurate than univariate age-based or length-based systems: despite being slightly less accurate in obese children than non-obese children, the Mercy method and the PAWPER XL tape remain the most accurate weight-estimation tools available. How these systems are used has been described elsewhere [22-25].�
The algorithm�
The rationale behind the proposed algorithm was straightforward � to provide a method to quickly and accurately obtain estimates of an obese child�s TBW and IBW within the first few moments of initiating resuscitative care.�
Key elements of the algorithm�
The identification of the obese child is at the crux of this algorithm, but it can be difficult even for experienced healthcare providers to identify obesity accurately [17]. Ideally, a validated system of assessing habitus should be employed such as reference images, or anthropometric measurements (e.g. mid-arm circumference or waist circumference) [26, 27]. This may add slightly to the time taken to follow the algorithm, but will increase the accuracy and appropriateness of management. The reliability of parental estimates has not been established in obese children and should be considered only if the parent can confidently recall a very recent measured weight. Parents cannot accurately assess the weight status of their children and may underestimate weight when asked to estimate. The user of this algorithm must weigh up the use of one method of weight estimation against the use of multiple methods. The Mercy method is slightly more accurate than the PAWPER XL tape in estimating TBW in severely obese children, but it cannot predict IBW. The clinical scenario may dictate which method or methods are most appropriate: the speed with which a weight-estimation is required (e.g. to calculate a defibrillation dose versus to calculate an induction dose for rapid sequence intubation) may also impact this decision. It would be beneficial if clinicians were proficient with more than one technique.�
Prerequisites for success: overcoming complexity�
Converting a quantification of body weight into the correct volume of diluted drug to administer is a complex, cognitively-intense process. It cannot succeed reliably without the use of comprehensive drug-dosing resuscitation aids, which provide information on drug dilution, preparation and required volume-to-administer. In obese children, this is far more complex, because of the need to use the correct weight descriptor for each drug (TBW or IBW). This would preferably be achieved using a computerised system or mobile phone application to limit the potential for error. Further research is still required in this field to determine the feasibility of such a system for use in both obese and non-obese children.�
Obstacles to emergency weight estimation�
There are two main obstacles to optimum drug therapy in emergencies, which are a reflection of a statement by the Institute of Medicine in the USA: �Meet the enemy: he is us� [28]. The first obstacle is scepticism, the second is a lack of professionalism.�
Scepticism�
There is an argument that the lack of high-grade evidence for many paediatric drug dose ranges means that it is pointless to attempt to estimate weight accurately. It is true that not enough is known about drug doses in children, but the clinician must nonetheless attempt to reduce errors as much as possible [7]. To use a system of weight estimation that is known to be inaccurate must be considered poor medical practice [29]. It is therefore essential that the most accurate and appropriate weight estimation systems be used.�
Professionalism�
A lowered standard of care should not be tolerated during emergencies. Even the most basic weight estimation techniques have been shown to be vulnerable to error without appropriate instruction and practice, so training in weight estimation should become routine [30]. Prompt defibrillation is emphasised, taught and trained for the treatment of arrythmogenic cardiac arrest, but the preceding, paralysing, fumbling delay in weight estimation to allow for energy dose calculation is frequently overlooked in the teaching. Weight estimation and drug dosing needs to be integral to the teaching and training for resuscitation. In this way weight estimation will not be an impediment to medical care, but will enhance it. This could happen in two ways. Weight estimation procedures should form part of simulation training drills so that healthcare providers become familiar with how to integrate them into acute medical care and how best to use resuscitation aids. Weight estimation procedures could also be performed on children with less acute presentations, together with feedback from actual measured weight, so that healthcare providers can become more experienced, and more accurate, with the use of their preferred systems.�
Limitations�
Given the lack of evidence on this topic, it was impossible to provide more than low-grade recommendations on how weight estimation could be used in a resuscitation setting.
A greater emphasis should be placed on the role of weight estimation in paediatric resuscitation: an integrated, comprehensive weight-estimation-resuscitation aid system can facilitate emergency medical care and reduce cognitive stress and medication errors. A poorly-planned weight estimation and drug dosing strategy can inject impediments into medical care with a high consequent risk of medical errors. Training in every element of resuscitative management, including weight estimation, is essential to deliver the level of professional care that our patients deserve. Differences in obese children�s body composition should be respected and dealt with according to pre-planned methodology, making use of appropriate methodologies to estimate or measure TBW and IBW when indicated. This algorithm is a preliminary proposition, designed to assist the training and preparation of teams whose task it is to resuscitate children. This will need to be critically examined, tested in simulation and improved upon. Most importantly, this proposal is intended to draw attention to the need for professionalism in emergency care: to advocate for the appropriate use of weight estimation and to promote training in weight estimation procedures to ultimately reduce medical errors in paediatric resuscitations.
What is known about this topic
- The three most accurate weight estimation systems at present are estimates by parents, the Mercy method and the PAWPER tape system;
- Weight estimation can be a barrier to the provision of successful emergency care;
- Training is essential to enable healthcare providers to use weight estimation systems effectively.
What this study adds
- This study provides a unique method of training in weight estimation for emergency care;
- This study also provides a first-of-its-kind algorithm to allow the user to select the most appropriate method of estimating weight in children of different habitus;
- This study also provides evidence-based guidelines on the use of total and ideal body weight for drug dose calculations.
The authors declare no competing interest.
MW and LNG both contributed equally to the design, data collection and writing of this paper. All authors have read and agreed to the final version of this manuscript.
We are grateful to Dr Alison Bentley who provided general and supervisory support; this project was part of doctoral research which she supervised.
Table
1: summary of the evidence evaluated: the direct and indirect evidence
for each topic is displayed; there is very little evidence on
any aspect of weight estimation other than accuracy, much of
which is of low grade
Table 2: notes on the weight estimation algorithm
Figure 1: a hierarchy of weight estimation systems ranked according to level of accuracy and ease-of-use
Figure 2: the full devised weight-estimation algorithm
Figure 3: a description of the weight estimation systems included in the algorithm
Figure 4: three clinical scenarios highlighting the time-sensitive need for both TBW and IBW in an obese child
- Porter E, Barcega B, Kim TY. Analysis of medication errors in simulated pediatric resuscitation by residents. West J Emerg Med. 2014 Jul;15(4):486-90. PubMed | Google Scholar
- Kaufmann J, Laschat M, Wappler F. Medication errors in pediatric emergencies: a systematic analysis. Dtsch Arztebl Int. 2012 Sep;109(38):609-16. PubMed | Google Scholar
- Srinivasan V, Nadkarni VM, Helfaer MA, Carey SM, Berg RA, American Heart Association National Registry of Cardiopulmonary Resuscitation I. Childhood obesity and survival after in-hospital pediatric cardiopulmonary resuscitation. Pediatrics. 2010 Mar;125(3):e481-8. PubMed | Google Scholar
- Luten R, Wears RL, Broselow J, Croskerry P, Joseph MM, Frush K. Managing the unique size-related issues of pediatric resuscitation: reducing cognitive load with resuscitation aids. Acad Emerg Med. 2002 Aug;9(8):840-7. PubMed | Google Scholar
- Rowe S, Siegel D, Benjamin DK Jr. Best Pharmaceuticals for Children Act - Pediatric Trials Network Administrative Core C Gaps in drug dosing for obese children: a systematic review of commonly prescribed emergency care medications. Clin Ther. 2015 Sep 1;37(9):1924-32.
- Wells M, Goldstein L, Botha M. Emergency drug dosing in children. Edinburgh: Churchill Livingstone Elsevier. 2012.
- Waters MR. Paediatric resuscitation Dosage inaccuracies may be dangerous. BMJ. 1993 Jun 12;306(6892):1612-3. PubMed | Google Scholar
- Ross EL, Heizer J, Mixon MA, Jorgensen J, Valdez CA, Czaja AS et al. Development of recommendations for dosing of commonly prescribed medications in critically ill obese children. Am J Health Syst Pharm. 2015 Apr 1;72(7):542-56. PubMed | Google Scholar
- Kendrick JG, Carr RR, Ensom MH. Pharmacokinetics and drug dosing in obese children. J Pediatr Pharmacol Ther. 2010 Apr;15(2):94-109. PubMed | Google Scholar
- Marlow R, Lo D, Walton L. Accurate paediatric weight estimation by age: mission impossible? Archives of Disease in Childhood. 2011;96(Suppl 1):A1-A2. Google Scholar
- Carasco CF, Fletcher P, Maconochie I. Review of commonly used age-based weight estimates for paediatric drug dosing in relation to the pharmacokinetic properties of resuscitation drugs. Br J Clin Pharmacol. 2016 May;81(5):849-56. PubMed | Google Scholar
- Traub SL, Kichen L. Estimating ideal body mass in children. Am J Hosp Pharm. 1983 Jan;40(1):107-10. PubMed | Google Scholar
- Young KD, Korotzer NC. Weight estimation methods in children: a systematic review. Ann Emerg Med. 2016 Oct;68(4):441-451.e10. PubMed | Google Scholar
- Nieman CT, Manacci CF, Super DM, Mancuso C, Fallon WF Jr. Use of the Broselow tape may result in the underresuscitation of children. Acad Emerg Med. 2006 Oct;13(10):1011-9. PubMed | Google Scholar
- Luten R, Zaritsky A. The sophistication of simplicity... optimizing emergency dosing. Acad Emerg Med. 2008 May;15(5):461-5. PubMed | Google Scholar
- Rosenberg M, Thundiyil J, Greenberger S, Rawal A, Latimer-Pierson J. Does physician estimates of pediatric patient weights lead to inaccurate medication dosages. Annals of Emergency Medicine. 2010;56(3 (Suppl September 2010)):S47. Google Scholar
- Cornelissen KK, Gledhill LJ, Cornelissen PL, Tovee MJ. Visual biases in judging body weight. Br J Health Psychol. 2016 Sep;21(3):555-69. PubMed
- Georgoulas V, Wells M. The PAWPER tape and the Mercy Method outperform other methods of weight estimation in children in South Africa. S Afr Med J. 2016 Aug 7;106(9):933-9. PubMed | Google Scholar
- Wells M, Goldstein L, Bentley A. High-tech adjuncts to emergency weight estimation: point-of-care ultrasound and point-of-care bioelectrical impedance measurements can increase the accuracy of length-based weight estimation in children. Trauma and Emergency Care. 2017;2(3):1-8. Google Scholar
- Rinke ML, Moon M, Clark JS, Mudd S, Miller MR. Prescribing errors in a pediatric emergency department. Pediatr Emerg Care. 2008 Jan;24(1):1-8. PubMed | Google Scholar
- Wells M, Kramer E. Optimizing emergency drug dosing in children. Acad Emerg Med. 2008 Dec;15(12):1325; author reply 1326. PubMed | Google Scholar
- Lubitz DS, Seidel JS, Chameides L, Luten RC, Zaritsky AL, Campbell FW. A rapid method for estimating weight and resuscitation drug dosages from length in the pediatric age group. Ann Emerg Med. 1988 Jun;17(6):576-81. PubMed | Google Scholar
- Traub SL, Johnson CE. Comparison of methods of estimating creatinine clearance in children. Am J Hosp Pharm. 1980 Feb;37(2):195-201. PubMed | Google Scholar
- Abdel-Rahman SM, Ridge AL. An improved pediatric weight estimation strategy. Open Medical Devices Journal. 2012;4:87-97. Google Scholar
- Wells M, Coovadia A, Kramer E, Goldstein L. The PAWPER tape: a new concept tape-based device that increases the accuracy of weight estimation in children through the inclusion of a modifier based on body habitus. Resuscitation. 2013 Feb;84(2):227-32. PubMed | Google Scholar
- Tanner D, Negaard A, Huang R, Evans N, Hennes H. A prospective evaluation of the accuracy of weight estimation using the Broselow Tape in overweight and obese pediatric patients in the Emergency Department. Pediatric Emergency Care. 2017 Oct;33(10):675-678. Google Scholar
- Britnell S, Taylor S, Koziol-McLain J. Emergency weight estimation lookup tables for New Zealand children aged 5-10 years. Emerg Med Australas. 2016 Oct;28(5):558-63. PubMed | Google Scholar
- Nash DB. Meet the enemy: he is us. Am J Med Qual. 2011 Jan-Feb;26(1 Suppl):4S. PubMed
- Luscombe M, Owens B. Weight estimation in resuscitation: is the current formula still valid? Arch Dis Child. 2007 May;92(5):412-5. Epub 2007 Jan 9. PubMed | Google Scholar
- Frush K, Hohenhaus S, Luo X, Gerardi M, Wiebe RA. Evaluation of a Web-based education program on reducing medication dosing error: a multicenter, randomized controlled trial. Pediatr Emerg Care. 2006 Jan;22(1):62-70. PubMed | Google Scholar