Application of the Canadian C-Spine rule and nexus low criteria and results of cervical spine radiography in emergency condition
William Ngatchou, Jeanne Beirnaert, Daniel Lemogoum, Cyril Bouland, Pierre Youatou, Ahmed Sabry Ramadan, Regis Sontou, Maimouna Bol Alima, Alain Plumaker, Virginie Guimfacq, Claude Bika, Pierre Mols
Corresponding author: William Ngatchou, Department of Cardiac Surgery and Emergency medicine St Pierre Hospital, Brussels, Belgium 
Received: 04 Jul 2017 - Accepted: 15 Jun 2018 - Published: 21 Jun 2018
Domain: Emergency medicine
Keywords: Cervical spine X-ray, emergency, quality
©William Ngatchou et al. Pan African Medical Journal (ISSN: 1937-8688). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: William Ngatchou et al. Application of the Canadian C-Spine rule and nexus low criteria and results of cervical spine radiography in emergency condition. Pan African Medical Journal. 2018;30:157. [doi: 10.11604/pamj.2018.30.157.13256]
Available online at: https://www.panafrican-med-journal.com//content/article/30/157/full
Original article 
Application of the Canadian C-Spine rule and nexus low criteria and results of cervical spine radiography in emergency condition
Application of the Canadian C-Spine rule and nexus low criteria and results of cervical spine radiography in emergency condition
William Ngatchou1,&, Jeanne Beirnaert2, Daniel Lemogoum3, Cyril Bouland2, Pierre Youatou2, Ahmed Sabry Ramadan2, Regis Sontou4, Maimouna Bol Alima5, Alain Plumaker2, Virginie Guimfacq6, Claude Bika7, Pierre Mols2
1Department of Emergency and Cardiac Surgery, St Pierre University Hospital, Universit� Libre de Bruxelles, Belgium, 2Department of Emergency St Pierre University Hospital, Universit� Libre de Bruxelles, Belgium, 3Department of Cardiology, Erasme University Hospital, Universit� Libre de Bruxelles, Belgium, 4Department of Radiology, St Pierre University Hospital, Universit� Libre de Bruxelles, Belgium, 5Department of Cardiac Surgery, St Luc University Hospital, Universit� Catholique de Louvain, Belgium, 6Department of Cardiology, Ixelles University Hospital, Universit� Libre de Bruxelles, Belgium, 7Universit� de Douala, Cameroun
&Corresponding author
William Ngatchou, Department of Cardiac Surgery and Emergency medicine St Pierre Hospital, Brussels, Belgium
Introduction: the Canadian C Spine Rule (CCR) and the National Emergency X-Radiography Utilization Study (Nexus) low criteria are well accepted as guide to help physician in case of cervical blunt trauma.
Methods: we aimed to evaluate retrospectively the application of these recommendations in our emergency department. Secondly we analyzed the quality of cervical spine radiography (CSR) in an emergency setting.
Results: 281 patients with cervical blunt trauma were analyzed retrospectively. The CCR and the NEXUS rules were respected in 91.2% and 96.8% of cases respectively. No lesions were found in 96.4% of patient. A lesion was present in 1.1% of patient and suspected in 2.5% of patient. The quality of CSR was adequate in only 37.7% of patient. The poor quality of CSR was due either to the lack of C7 vertebrae visualization in 64.6% or other lower vertebrae in 28%. Other causes included the absence of open mouth view (8%), the absence C1 vertebrae visualization (3.4%), artifact in 2.3% and the absence of lateral view in 0.6% of patient.
Conclusion: CCR and NEXUS are widely used in our emergency department. The high rate of inadequate CSR reinforces the debate about it�s utility in emergency condition.
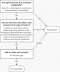
Cervical blunt trauma is major health problem in developed countries [1,2]. Missing a cervical-spine fracture is an obsession of many emergency departments� physicians, leading to unnecessary cervical-spine radiography (CSR). Two decision rules have been developed independently to permit more selective ordering of CSR, more rapid ruling out of injury to the cervical for patients, decrease patients� exposure to ionizing radiation and economic losses [3]. In 1992, The National Emergency X-Radiography Utilization Study (NEXUS) Low-Risk Criteria (NLC) developed one simple decision making instrument based on five clinical criteria (Table 1) that can help physicians to identify reliably the patients who need CSR after blunt trauma [4,5]. The second decision rule was the Canadian Cervical-Spine Rule (CCR) developed in 2001 in ten Canadian emergency departments [6]. This rule uses 3 high-risk criteria (age 65 year or older, dangerous mechanism, paresthesias in the extremities), 5 low criteria (simple rear-end motor vehicle crash, sitting position in emergency department, ambulatory at any time, delayed onset of neck pain, and absence of midline C �spine tenderness), and the ability of patients to actively rotate their necks, to determine the need for CSR (Figure 1). While these rules are widely accepted, their current application and results are poorly studied. The aim of this study was to evaluate retrospectively the compliance of our emergency physicians to these recommendations. The second objective was to assess the quality of CSR performed in emergency settings.
We retrospectively analyzed the file of all patients over 15 years old who underwent CSR following blunt trauma in our emergency department between January 2013 and December 2015. Patient with penetrating trauma and patient who underwent firstly Computer Tomography (CT) of the cervical spine were not included. For each eligible patient, data concerning mechanism of injury, the symptoms, and the respect of both NEXUS and CCR rules and the result of radiography were recorded. The quality of cervical CSR was defined by a senior radiologist as adequate (presence of anterior, lateral, and open mouth images, presence of all of seven cervical vertebrae, No artifact) or inadequate (absence of one or more than one vertebrae, absence of lateral or open mouth images, the presence of artifact). This protocol was approved by the local ethic committee (CHU St Pierre, Brussels, Belgium Agreement number: O.M. 007).
�
Statistical analysis�
Quantitative data were presented as mean � standard deviation (SD) and qualitative data were presented as counts and frequencies. Means were compared between good and poor quality of radiography using Student-t test while frequencies were compared using Chi squared test. All analyses were performed using SPSS 2.0 software.
Overall 281 patients were included. Demographics and clinical characteristics are summarized in Table 2. The mean age was 38.6 years. The mechanism of trauma was high in 70.8% of cases, 40.6% presented local pain. CCR and Nexus rules were respected in 91.8% and 96.8% of cases respectively. No lesion was found in 96.4% of patient. A lesion was present in 1.1% of patient and suspected in 2.5% of patient. The quality of X-ray was good in only 37.7% of patient. The poor quality of X-ray was due to the absence C7 vertebrae in 64.6%, the absence of more than C7 vertebrae in 28%, the absence of open mouth imaging in 8%, the absence of C1 in 3.4%, artifact in 2.3% and no profile in 0.6% of patient (Table 3).
The present study revealed that the Nexus and the CCR rules are well applied in our emergency department. In a survey send to 61 Massachusetts emergency physicians, Weiner S et al reported that only 56% and 10% of them recognized using the NEXUS and CCR rules respectively in their current practices [7]. The most common reason cited for not using the NEXUS rules in this study was patient insistence on obtaining a radiograph. The most common reason for not using the CCR was that it is too difficult to remember and use in daily practice. The Canadian team have published controversial studies showing the superiority of CCR [3,8]. This debate between the NEXUS and the Canadian group may have decreased the reliably of physician to these rules [7]. Furthermore, Zoe et al in a meta-analysis of 15 studies demonstrated that despite their high sensitivity, these rules have low specificity [9]. In our department, physicians are encouraged to use at least one rule before sending patients to perform CSR.
�
The second finding of this current study is the low rate of adequate CSR. An adequate CSR includes three views: a true lateral view, which must include all seven cervical vertebrae as well as C7-T1 junction, an anterior posterior view and an open mouth odontoid view [10]. In the context of trauma these images are all difficult to acquire because the patient may be in pain, confused, unconscious, or unable to cooperate due to the immobilization devices. In 92% of case, the absence of lower cervical vertebrae was the reason of inadequacy of radiograph. Traction on the arms may facilitate visualization of all seven cervical vertebrae on the lateral film. The fact that our technologist is alone could explain such findings. In a retrospective study of 640 consecutive CSR, Gale et al reported entire cervical spine visualization in only 27.8% of patients [11]. The author concluded provocatively that CSR are inadequate to fully evaluate the cervical spine after blunt trauma, and supplemental computer tomography (CT) is commonly required. Several others studies have also suggested the superiority of CT in moderate to high-risk adults [12-14] as well as in lower risk context [15]. The systematic use of CT for initial evaluation of blunt cervical spine injury points out the problem of radiation exposure [16] and the unjustifiable raise of health care cost [13,14]. On the other hand, repeated attempts to obtain adequate CSR could also be ineffective. Moreover, the arrival of fasted low-dose radiation exposure CT, the raise of malpractice lawsuit procedure against emergency physicians and radiologist will probably decrease the number of CSR in the future [17]. The development and the increasing availability of low dose multidetector CT will be the solution [18].
CCR and NEXUS are widely used in our emergency department. The high rate of inadequate CSR reinforces the debate about its utility in emergency condition.
What is known about this topic
- Cervical blunt trauma is major health problem in developed countries;
- The Canadian C Spine Rule (CCR) and the National Emergency X-Radiography Utilization Study (Nexus) low criteria are well accepted as guide to help physician in case of cervical blunt trauma;
- While these rules are widely accepted, their current application and results are poorly studied.
What this study adds
- The high rate of inadequate CSR reinforces the debate about its utility in emergency condition.
The authors declare no competing interests.
William Ngatchou (redaction), Jeanne Beirnaert (data collection), Daniel Lemogoum (translation), Cyril Bouland (data collection), Pierre Youatou (data collection), Ahmed Ramadan (data collection), Regis Sontou (X-ray analyze), Maimouna Bol Alima (translation), Alain Plumaker (review), Virginie Guimfacq (review), Claude Bika (statistical analysis) ,Pierre Mols (review). All authors have read and agreed to the final manuscript.
Table 1: the NEXUS low-risk criteria
Table 2: demographics and clinical characteristics
Table 3: reason inadequacy of cervical spine radiography
Figure 1: the Canadian C-Spine rule
- Chappuis G, Soltermann B. Numbur and cost of claims to minor cervical trauma in Europe: results from the comparative study by CEA, AREDOC and CEREDOC. Eur Spine J. 2008 Oct;17(10):1350-7. Epub 2008 Aug 15. PubMed | Google Scholar
- McCaig LF, Ly N. National Hospital Ambulatory Medical Care Survey: 2000 emergency department summary. Advance data from vital and health statistics. N� 326 hyattsville, Md: National center for Health statistics, 200 (DHHS publication (PHS) 2002-1250 02-02259). In Press.
- Stiell IG, Clement C, Mc Knight RD, Brison R, Schull MJ, Rowe BH et al. The Canadian C-Spine Rule versus the nexus Low-risk Criteria in patients with trauma. N Engl J Med. 2003 Dec 25;349(26):2510-8. PubMed | Google Scholar
- Hoffman JR, Schriger DL, Mower W, Luo JS, Zucker M. Low-risk criteria for cervical-spine eadiography in blunt trauma: a prospective study. Ann Emerg Med. 1992 Dec;21(12):1454-60. PubMed | Google Scholar
- Mahadevan S, Mower WR, Hoffman JR, Peeples N, Goldberg W, Sonner R. Interraterreliability of cervival spine injury criteria in patient with blunt trauma. Ann Emerg Med. 1998 Feb;31(2):197-201. Google Scholar
- Stiell IG, Wells GA, Vandemheen KL, Clement CM, Lesiuk H, De Maio VJ et al. The Canadian C-Spine rule for Radiography in alert and stable trauma patients. JAMA. 2001 Oct 17;286(15):1841-8. PubMed | Google Scholar
- Weiner S. The actual application of the NEXUS and Canadian C-Spine Rules by Emergency Physicians. Internat J Emerg Med. 2005;5:1-5. In Press.
- Dickinson G, Stiell IG, Schull M, Brison R, Clement CM, Vandemheen KL et al. Retrospective application of the NEXUS low �risk application criteria for cervical spine radiography in Cannadian emergency departments. Ann Emerg Med. 2004 Apr;43(4):507-14. PubMed | Google Scholar
- Michaleef ZA, Maher CG, Verhagen AP, Rebbeck T, Lin CW. Accuracy of the Canadian C-Spine rule and NEXUS to screen for clinical important cervical spine injury in patients following blunt trauma; asystematic review. CMAJ. 2012 Nov 6;184(16):E867-76. Epub 2012 Oct 9. PubMed | Google Scholar
- Tintinalli JE, Ruiz E, Krome RL. Emergency medicine: a comprehensive study guide. 4th ed. New York: Mc Graw-Hill; 1996. In Press.
- Gale SC, Gracias VH, Reilly PM, Schwab CW. The inefficiency of plain radiography to evaluate the cervical spine after blunt trauma. J Trauma. 2005 Nov;59(5):1121-5. PubMed | Google Scholar
- Homles JF, Akkinepalli R. Computer Tomography versus plain radiography to screen for cervical spine injury: a meta-analysis. J Trauma. 2005;58(5):902-905. Google Scholar
- Blackmore CC, Ramsey SD, Mann FA, Deyo RA. Cervical spine injury screening with CT in trauma patients: a cost-effectiveness analysis. Radiology. 1999 Jul;212(1):117-25. Google Scholar
- Hanson JA, Blackmore CC, Ramsey SD, Mann FA, Wilson AJ. Cervical spine injury: a decision rule to identify high-risk patients for helical CT screening. AJR Am J Roentgenol. 2000 Mar;174(3):713-7. PubMed | Google Scholar
- Bailitz J, Starr F, Beecroft M, Bankoff J, Roberts R, Bokhari F et al. CT should replace three-view radiographs as initial sreening test in patients at high, moderate, and low risk blunt cervical spine injury: a prospective comparison. J Trauma. 2009 Jun;66(6):1605-9. PubMed | Google Scholar
- Rybicki F, Nawfel RD, Judy PF, Ledbetter S, Dyson RL, Halt PS et al. Skin and thyroid dosimetry in cervical spine screening: two methods for evaluation and et comparison between a helical CT and radiographic trauma series. AJR. 2002;179(4):933-937. Google Scholar
- Quigley RS, Akpolat YT, Forrest BD, Wongworawat MD, Cheng WK. Reason for lawsuit in spinal cord injury affects final outcome. Spine (Phila Pa 1976). 2015 Jun 1;40(11):851-5. PubMed | Google Scholar
- Mulkens TH, Marchal P, Daineffe S, Salgado R, Rijdt BT, Kegelaers B, Ternote JL. Comparison of low-dose with multidetector CT in cervical spine trauma. AJNR Am J Neuroradiol. 2007 Sep;28(8):1444-50. PubMed | Google Scholar