Uptake of health insurance among Muslims in Nairobi county, Kenya
Mohammed Abdi Hassan, Wanja Mwaura-Tenambergen, Muthoni Mwangi Eunice
Corresponding author: Mohammed Abdi Hassan, Department of Health Systems Management, School of Medical Education, Kenya Methodist University, Nairobi, Kenya 
Received: 09 Mar 2017 - Accepted: 24 Aug 2017 - Published: 08 Sep 2017
Domain: Health system development
Keywords: Health insurance, insurance uptake, Muslims, Kenya
©Mohammed Abdi Hassan et al. Pan African Medical Journal (ISSN: 1937-8688). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Mohammed Abdi Hassan et al. Uptake of health insurance among Muslims in Nairobi county, Kenya. Pan African Medical Journal. 2017;28:12. [doi: 10.11604/pamj.2017.28.12.12214]
Available online at: https://www.panafrican-med-journal.com//content/article/28/12/full
Uptake of health insurance among Muslims in Nairobi county, Kenya
Mohammed Abdi Hassan1,&, Wanja Mwaura-Tenambergen1, Muthoni Mwangi Eunice1
1Department of Health Systems Management, School of Medical Education, Kenya Methodist University, Nairobi, Kenya
&Corresponding author
Mohammed Abdi Hassan, Department of Health Systems Management, School of Medical Education, Kenya Methodist University, Nairobi, Kenya
Introduction: in Kenya and the world across, health insurance has been reckoned as an important health policy that serves to protect households from the direct financial consequences of health care and meet the Sustainable Development Goal of Universal Health Coverage and Poverty Eradication. However, health insurance uptake has remained to be a major challenge for universal health care coverage especially among Kenyan Muslims who have conflicting religious faith towards conventional health insurance. This study had two main objectives: (1) to determine level of uptake of health insurance among Muslims and (2) to examine the role of religion in health insurance uptake among Muslims.
Methods: the study adopted a cross-sectional study design. Post-stratified sampling was used to select 389 respondents who participated in the survey questionnaires. Descriptive statistics, cross-tabulation and Test of independence (Chi-square) were used to analyze quantitative data using SPSS Version 20.
Results: findings revealed that only 86(22%) of Muslims were enrolled in a health insurance scheme. Among the 86 Muslims who had an insurance cover, Majority were enrolled in National Health Insurance Fund (65,70.6%) while 21(29.4%) were enrolled in private health insurance schemes. Among the 303 Muslims who had no insurance cover, 285 (94.1%)preferred being enrolled in Takaful Health insurance which is Shariah Compliant. Religion played a significant role on choice and enrollment of Muslims to health insurance schemes. Religious beliefs and Shariah teachings had a statistically significant relationship with uptake of health insurance (p < 0.05).
Conclusion: uptake of health insurance among Muslims is low despite the growing population of Muslims in Kenya partly due to Muslims strong religious belief and Shariah laws, which prohibits them from enrolling into conventional insurance hence limiting freedom of individual decisions on the insurance schemes to enroll in. Despite high demand for health insurance products among Muslims, there lacks health insurances products aligned to the religious beliefs and needs of Muslim hence exposing them to hefty medical bills which deepens poverty and inaccessibility to basic health care.
Financing healthcare delivery in the country is an insurmountable challenge to the economy and a hindrance to equitable access to high standard healthcare services [1]. Many countries including Kenya have been seeking for ways of how their health financing systems can provide sufficient financial risk protection to all of the population against the costs of healthcare irrespective of their diversity and religious affiliation. Proper health care financing ensures that the population not only has access to health care but also use the health services when they need them. Lack of health insurance has profound negative impact on health indicators when a large proportion is not covered. This is more critical in developing countries like Kenya where health sector is underfunded by approximately sixty to seventy percent [2]. As a result, in Kenya, many people incur significant out of pocket payment for health services whenever they need them due to lack of health insurance. This has led to catastrophic spending to a level of impoverishing the family unit through sale of assets and diversion of their meager income to cover medicare bills and expenditures [3]. The Kenyan households bear the greater burden of about 40% of the healthcare costs through out of pocket cash payment that on average drive at least one million economically marginal Kenyans below the poverty line annually, whenever sickness in the family occurs [1, 2]. Research indicates that the NHIF and other forms of health insurers have not been able to effectively reach out to majority of Kenyans, especially the poor, those in the informal sector and those with strong religious beliefs against conventional insurance like the Muslims [4].
For instance, National Health insurance Fund has achieved high levels of coverage of the formal sector up to almost 100%, but the coverage of the informal sector has proved more challenging; it accounts for 19% of the total membership of the Fund [5]. Empirical evidence finds health insurance to be associated with increased access and timely utilization of regular and appropriate health care services by individuals and families; it reduces the chances of out-of-pocket payments of healthcare bills at the point of delivery and ultimately reduces vulnerability and poverty [1, 3, 4]. In Kenya, 10% of total health care occurs in a pooled basis where 5.4% of total health expenditure is derived from public health insurance, which is collected through employers; National Health Insurance Fund contributes less than 4% of the total health expenditure, OOP funds 29% of Kenyan health care while 39% is funded by the government [6]. Although health insurance continues to grow widely across Africa's diverse socio-cultural landscape, coverage continues to be a fundamental challenge in achieving universal health coverage. Religion and ethnicity have been greatly associated with demand for health insurance [1]. This situation is more critical among Muslims who view conventional insurance schemes to be non-compliant with Shariah laws [7] which has resulted in few Muslims except those in mandatory health insurance having enrolled in conventional health insurance [8, 9]. Limited efforts have been taken to provide health insurance among Muslims. For example, Takaful insurance, which is Shariah compliant, has been formed to offer insurance products. However, preliminary reviews revealed that the insurance providers did not have health insurance products [7, 9]. This has left many Muslims with little financial protection for themselves and their dependents in case of health problems and illnesses [7, 8, 10] which deepens poverty and increases inaccessibility to health care.
Study population and location: this was a cross-sectional study design which was carried out in January, 2015 among Muslims in Nairobi County, Kenya. According to KNBS [11], approximately, about 4.3 million Muslims live in Kenya of whom, 60 percent live in urban areas. Nairobi county has the highest urban population in East Africa of about 3,138,369 million. About 10% of this population, 313,000, is made up of Muslim (Kenya National Bureau of Statistics, 2013). The study was carried out in Starehe and Kamukunji Sub-counties which had high number of muslims residents comprising middle and low income level earners [12].
�
Sampling technique and sample size: two-phase sampling, also called "post stratified sampling" was used in selecting study respondents from households [13]. A large sample of households was selected from the study sites and a short, screening interview of the household heads done to extract characteristics. This was followed by post-stratification of the identified households into two categories based upon the screening interview/inclusion criteria; those which met the inclusion criteria and those which did not meet the criteria. This was followed by simple random sampling of a sub-sample of households from the strata (identified households) which meets the inclusion was done to select 422 households who met the inclusion criteria. Two repeat visits were conducted to enroll those who were absent from the households during the initial data collection. A total of 389 household heads consented to the study and were successfully interviewed which translated to a response rate of 92.2%.�
Inclusion and exclusion criteria: the study included all muslims who gave informed consent to participate in the study and were residents of Nairobi county for at least 1 year and living in the selected study sites. However, the study excluded three respondents who were too sick to participate in the study at the time of data collection based on their self-report.�
Data collection process: written informed consent which was designed to explain the need, purpose, benefit and process of participation was used to obtain informed consent from participants. A predesigned structured and closed ended pretested questionnaire was used to collect data. The questionnaire was divided into three sections: section A contained questions regarding the background/individual characteristics of the respondents including age, sex, education, marital status, household size, employment status, income level, illness experiences and health status; section B included questions on the uptake of health insurance such as status of enrollment and type of health insurance scheme enrolled and section C detailed questions which explored the role of influence of Shariah law and teachings on enrollment and perceived necessity of health insurance. During data collection, three (3) experienced and trained research assistants who were proficient in English, Swahili and Somali language were used to administer the questionnaires and assist respondents with literacy difficulty in filling them. The principal investigator provided guidance and supervised the team during data collection. Ethical clearance approval was obtained from Ethical and Research Committee of Kenya Methodist University.�
Data management: data was coded entered, cleaned and analyzed using SPSS version 21 statistical package. Descriptive statistics including frequencies and percentages were used in describing study variables. Cross-tabulations were used to explore relationships between variables while Chi-squared tests were applied in assessing possible association between religion and health insurance uptake. Statistical significance was inferred at 5 percent i.e. 0.05.
Socio-demographic characteristics of respondents: a total of 389 household heads participated in this study. In terms of gender, 214 (55%) of the respondents were males. Respondents were aged between 18 and 45 years old. About 212 (54.5%) were married and 245 (63%) had university education as the highest level of educational attainment. A total of 164 (42.2%) respondents earned a monthly income of over KShs.50,000 while 308 (79.2%) had more than 3 household members (Table 1).
�
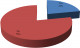
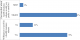
Uptake of health insurance among muslims: out of the 389 household heads interviewed, only 86 (22%) of them were enrolled in a health insurance scheme (Figure 1). Out of the 86 respondents who had a health insurance cover, 65 (70.6%) of them were enrolled in National Health Insurance Fund while only 21 (29.4%) were enrolled in private health insurance schemes. Out of the 303 respondents who were not enrolled in any health insurance scheme, 238 (78.4%) were willing to enroll in a health insurance; majority of them 285 (94.1%) preferred being enrolled in Takaful Health insurance while only 18 (5.9%) preferred conventional health especially such as NHIF (Figure 1).�
Role of religion on health insurance uptake: in regards to religion, 291 (74.8%) of the respondents said that religion influenced their decisions on uptake of health insurance. About three-quarter of the respondents (290, 74.6%) held the belief that health insurance was not necessary. There was a statistically significant relationship between religious beliefs (p = 0.009), Shariah laws (p = 0.015), perceived necessity of health insurance (p = 0.033) and uptake of health insurance (Table 2).
Despite the growing population of Muslims in Kenya, level of health insurance coverage among Muslims remains relatively low. This is to a large extent due to Muslims strong religious belief and Shariah laws which limit their individual ability and freedom to make decisions on the insurance schemes of choice to enroll [7]. Muslim teachings bar their faithful from enrolling into Shariah non-compliant insurance schemes constitute majority conventional insurances such as National Health Insurance Scheme which dominate the insurance market [8]. As a result, a substantial proportion of the Muslims are not covered by insurance except those in formal employment with mandatory social health insurance plans such as NHIF which makes them vulnerable to high health care expenditures in case of major illness. This situation is worsened by lack of Shariah compliant health insurances offering health insurance products aligned to the beliefs and needs of Muslim. This explains why uptake of health insurance among Muslims remains at low levels [7, 8]. Most of the existing Shariah compliant insurances companies cover mainly business related risks with little emphasis on health insurance, which leaves Muslims with no financial protection in case of illnesses. This causes many Muslims to incur significant OOP when utilizing health services due to lack of an insurance cover [14]. This has negative impact on health status of Muslims especially the poor. Majority of the Muslims who had an insurance cover were in formal employment. This was primarily due to their enrollment into mandatory health insurance as required by the Kenyan Government. This explains the high number of National Health Insurance Fund uptake among employed Muslims since their health insurance is administered by their employers [1, 14].
�
This means that majority of the common Muslims who have no employment and or are self- employed are not covered by health insurance hence exposing them to financial risks of ballooning medical expenses. This is consistent with study findings by Jacinta [2] who found that out of pocket payment funds about 29% of Kenyan health care expenditures. Many Muslims continues to experience catastrophic health care spending to a level of impoverishing a family unit through activities such as sale of assets and diversion of their meager income to cover the Medicare bills and expenditures [3, 4]. This has continued to increase financial and ill-health vulnerability among the many uninsured Muslims. On the other hand, demand and need for health insurance among the Muslims remains high and unmet; demand exists but the supply is very low [15]. Many uninsured Muslims were willing to enroll in a health insurance which is Shariah compliant. For instance, many Muslims were willing to enroll in Takaful health insurance scheme (a health insurance scheme which is designed and operated in line with Shariah laws and religious teaching) but there are no health insurance products, which are customized to the needs and requirements of Islamic teachings. Many Muslims are faithful to their religion and hence oppose anything that is perceived to contradict their religious teachings which are perceived as a cause of curse and therefore avoided as a sign of allegiance to their God, Allah for the purpose of receiving the blessings of obedience [7, 16]. Low uptake of health insurance due to religious beliefs is mainly based on the perception that Shariah compliance institutions are linked to high levels of trust and transparency which form key elements of health insurance uptake among Muslims [16].�
Shariah compliant products are perceived to value transparency, value for money and mutual benefit for all stakeholders which attracted Muslim faithful [17]. This is the guiding compass of a Muslim is the Islamic teachings and laws. Although Quran emphasizes the need for insurance against risks and losses, it is doesn't allow one to make profit or benefit against the other. It advocates for mutual benefit and improvement of welfare for all parties. Since most conventional insurance are perceived to be non-compliant to Shariah laws, Muslims are encouraged to avoid such products which are against their teachings [8, 18]. Conventional health insurances are perceived to result in some individual benefitting at the expense of others [19] i.e. they have elements of Maysir in which the profit of one party is dependent on the loss of the other which is forbidden in Shariah laws. These commercial insurance companies are perceived to exist to serve the interest of shareholders first, not policyholders. Such insurance schemes are deemed to contradict Islamic principles such as improvement of the welfare for all, which aims to establish a social order based on universal brotherhood [8]. Development of Shariah compliant health insurance products remains a promising strategy for increase demand and uptake of health insurance by Muslims hence improving universal health coverage. Although health insurance continues to grow widely across Africa's diverse socio-cultural landscape [1] Muslims still uphold conflicting faith and negative beliefs which negatively impact their ability and willingness to pay for a health insurance cover [8-10]. This has continued to expose many Muslims to financial and health vulnerabilities for themselves and their dependents in case of health problems and illnesses [20], which deepens poverty and increases inaccessibility to health care as emphasized by the following quote from one of the key informants interviewed.
Uptake of health insurance among Muslims is low despite the growing population of Muslims in Kenya mainly due to strong religious belief and Shariah laws which contradicts conventional insurances principles hence limiting their ability and willingness to enroll for social health insurance of choice to cushion them against medical expenses in case of illness. There exists a high demand for Shariah compliant health insurance products which are associated with high levels of trust and mutual benefit but the supply is non-existent hence creating a significant proportion of unmet need for health insurance among Muslims. Many Muslims remains exposed to financial risks associated with illness especially in the informal sector resulting into increasing out-of-pocket payment. To bridge the gap in health insurance coverage among Muslims, the government in partnership with all the key stakeholders should develop and implement Shariah compliant health insurance health insurance products to enhance acceptance and increase uptake among the Muslims. Existing insurance firms should explore opportunities for designing and expanding health insurance products aligned to Shariah teachings to target and respond to the demand, needs and expectations of the Muslims for health insurance. This can include review and alignment of available conventional health insurance products in the market including NHIF to conform to the needs and expectations of the Muslim community to reduce resistance for the uptake. The is also need for well developed and implemented health insurance product awareness campaigns targeting Muslims in the informal sector to increase awareness and encourage positive perceptions, attitudes and behaviour change towards enrolment into health insurance schemes of choice as a mechanism for reducing poverty and financial burdens associated with medical expenses.
What is known about this topic
- Muslim health insurance uptake is low;
- Due to lack of health insurance cover, many Muslims, especially the poor are financially vulnerable to escalating medical bills and hence exposed to impoverishment;
- Religion influences uptake of health insurance.
What this study adds
- Level of health insurance uptake among Muslims;
- Demand of health insurance among Muslims and type of health insurance; schemes preferred by Muslims;
- Religious factors/aspects associated with health insurance uptake.
The authors declare no competing interests.
Mohammed Abdi conceived and implemented the study. Both authors contributed to design of study, data analysis, interpretation and manuscript writing. Both authors have reviewed and approved the final version of the manuscript.
The investigators would like to express their gratitude to the participants, without whom, this study would be impossible.
Table 1: socio-demographic characteristics of the study respondents
Table 2: role of religion on health insurance uptake
Figure 1: level of health insurance uptake
Figure 2: insurance demand and preferences
- Isaac O and Clement A. Health Insurance and Vulnerability to Health Shocks in Ghana. Institute of Statistical. Social and Economic Research (ISSER), University of Ghana, 2011. Accessed on April 14th 2016.
- Munge K, Harvey A. The progressivity of health-care financing in Kenya. Health Policy Plan. 2014; 29(7): 912-920. PubMed | Google Scholar
- Brockmeyer B. Deliberations about an affordable national health insurance for the low income workforce in Namibia. 2012. The health system in Namibia. Accessed 25th May, 2016.
- Mathauer I, Schmidt JO, Wenyaa M. Extending social health insurance to the informal sector in Kenya: an assessment of factors affecting demand. International Journal of Health Planning and management. 2008; 23(1): 51-68. PubMed | Google Scholar
- Delloite. Review of the National Hospital Insurance Fund-Kenya. 2012. Accessed 22nd May, 2016.
- Jacinta A. Determinants of uptake of national hospital insurance fund scheme by the informal sector in Nairobi County, Kenya. 2012. School of Business; Kenyatta University. Accessed 25th May, 2016.
- Safder j, Farzana I, Jabran, N, Lindsay U. Takaful (Islamic Insurance): Concepts, Challenges and Opportunities. 2010. Milliman Research Report, Nairobi. Accessed 18th March 2016.
- Mohd M, Mohd F, Yeo C, Siti Y, Masnalliza M, Hardi M. A Study on Takaful and Conventional Insurance Preferences: the Case of Brunei. International Journal of Business and Social Science. 2012; 3(22): 34-43. Google Scholar
- Takaful News. Birth and Progress of Takaful in Africa; Issue 002. 2012. Accessed on 15th February 2016].
- Chua O. A Critical Evaluation of Insurance and Takaful. Proceedings from the International Conference on Takaful/Islamic Insurance Kuala Lumpur. 2000. Google Scholar
- KNBS. Kenya Population: Kenya Population Census. 2009. Accessed April 16th 2016.
- Kyobutungi, Ziraba A, "Ye" Y. The burden of disease profile of residents of Nairobi Slums: results from a demographic surveillance system. Health Metrics. 2006; 8: 6-1. Google Scholar
- UN. Studies in Methods: Designing Household Survey Samples; Practical Guidelines. 2005. Department of Economic and Social Affairs; Statistics Division: United Nations. Accessed 12th March 2016.
- Acharya A, Vellakkal S, Taylor F, Masset E, Satija A, Burke M. Impact of national health insurance for the poor and the informal sector in low-and middle-income countries. Soc Sci Med. 2012; 54(10): 1559-87. Google Scholar
- Donfouet P, Makaudze E, Mahieu P, Malin E. The determinants of the willingness-to-pay for community-based prepayment scheme in rural Cameroon. International journal of health care finance and economics. 2011; 11(3): 209-20. PubMed | Google Scholar
- Swartz, N, Coetzer P. (Takaful: an Islamic Insurance Instrument. Journal of Development and Agricultural Economics. 2010; 2(10): 333-339. Google Scholar
- Anwar, H. Islamic Finance: a Guide for International business and Investment. GMB Publishing Limited, United Kingdom. 2008. Google Scholar
- Ansari ZA. Analysis of the impact of reforms on insurance industry of Saudi Arabia. Interdisciplinary Journal of Research in Business. 2011; 1(8): 28-37. Google Scholar
- Ayub, M. Understanding Islamic Finance. John Willey & Sons. 2007. Google Scholar
- De Allegri M, Kouyat� B, Becher H, Gbangou A, Pokhrel S, Sanon M. Understanding enrolment in community health insurance in Sub-Saharan Africa: A population-based case-control study in rural Burkina Faso. Bull World Health Organ. 2006; 84(11): 852-8. PubMed | Google Scholar