The endoscopic endonasal approach to cranio-cervical junction: the complete panel
Nouman Aldahak, Bertram Richter, Joseph Synčse Bemora, Jeffery Thomas Keller, Sebastien Froelich, Khaled Mohamed Abdel Aziz
Corresponding author: Joseph Synčse Bemora, Department of Neurosurgery, Lariboisičre Hospital, Assistance Publique, Hôpitaux de Paris, University of Paris VII, Diderot 2, Rue Ambroise Paré 75475 Paris Cedex 10, Paris, France 
Received: 10 Mar 2017 - Accepted: 12 Jul 2017 - Published: 14 Aug 2017
Domain: Neurosurgery
Keywords: Craniocervical junction, endonasal, endoscopic, odontoidectomy, transnasal
©Nouman Aldahak et al. Pan African Medical Journal (ISSN: 1937-8688). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Nouman Aldahak et al. The endoscopic endonasal approach to cranio-cervical junction: the complete panel. Pan African Medical Journal. 2017;27:277. [doi: 10.11604/pamj.2017.27.277.12220]
Available online at: https://www.panafrican-med-journal.com//content/article/27/277/full
The endoscopic endonasal approach to cranio-cervical junction: the complete panel
Nouman Aldahak1,2, Bertram Richter1, Joseph Synčse Bemora2,&, Jeffery Thomas Keller3, Sebastien Froelich2, Khaled Mohamed Abdel Aziz1
1Department of Neurosurgery, Allegheny General Hospital, Drexel University College of Medicine, 420 East North Avenue, Suite 302, Pittsburgh, PA, 15212, USA, 2Department of Neurosurgery, Lariboisičre Hospital, Assistance Publique, Hôpitaux de Paris, University of Paris VII-Diderot 2, Rue Ambroise Paré 75475 Paris Cedex 10, Paris, France , 3Departments of Neurosurgery, University of Cincinnati College of Medicine, Cincinnati, Ohio, P.O Box 670515 Cincinnati, Ohio 45267-0515, USA
&Corresponding author
Joseph Synčse Bemora, Department of Neurosurgery, Lariboisičre Hospital, Assistance
Publique, Hôpitaux de Paris, University of Paris VII, Diderot 2, Rue Ambroise
Paré 75475 Paris Cedex 10, Paris, France
We aim to establish a complete summary on the Endoscopic Endonasal Approach (EEA) to Cranio Cervical Junction (CCJ): evolution since first description, criteria to predict the feasibility and limitations, anatomical landmarks, indications and biomechanical evaluation after performing the approach. A comprehensive literature search to identify all available literature published between March 2002 and June 2015, the articles were divided into four categories according to their main purpose: 1- surgical technique, 2- anatomical landmarks and limitations, 3- literature reviews to identify main indications, 4- biomechanical studies. Thereafter, we demonstrate the approach step-by-step, using 1 fresh and 3 silicon injected embalmed cadaveric specimen heads. 61 articles and one poster were identified. The approach was first described on cadaveric study in 2002, and firstly used to perform odontoidectomy in 2005. The main indication is odontoid rheumatoid pannus and basilar invagination. The nasopalatine line (NPL), the superior nostril-hard palate Line (SN-HP), the naso-axial line (NAxL), the rhinopalatine Line (RPL) and other methods were described to predict the anatomical feasibility of the approach. The craniocervical fusion is potentially unnecessary after removal of < 75% of one occipital condyle. A recent cadaveric study stated the possibility of C1-C2 fusion via EEA. This paper reviews all available clinical and anatomical studies on the EEA to CCJ. The approach marked a significant evolution since its first description in 2002. Because of its lesser complications compared to the transoral approach, the EEA became when feasible, the approach of choice to the ventral CCJ.
The transoral approach with its various variations has been the standard route of ventral access for the CCJ [1-5]. This procedure requires a long retraction of the tongue, dissection of the soft palate and incision in the oropharynx below the level of soft palate resulting in morbidity including tracheostomy from tongue swelling, enteral tube feeding or gastrostomy, wound healing complications and velopharyngeal incompetence (hypernasal speech and nasal reflux) due to the incision below the level of the soft palate [6, 7]. In 2002, Alfieri et al [8] published the first anatomical study demonstrated that the CCJ could be sufficiently exposed by the endonasal endoscopic route. This anatomical work gave the start signal to numerous anatomical and clinical studies to develop the Endoscopic Endonasal Approach (EEA). The aim of this study is to identify the evolution of the EEA to CCJ since its first description to achieve a complete summary of surgical technique, anatomical and radiological landmarks that predict the feasibility and limitations of the approach, various indications, biomechanical effect of the approach on stability of CCJ, and finally to demonstrate a step-by-step anatomical study.
Literature review: we performed a comprehensive literature review of all the English literature published from March 2002 up to June 2015. We utilized the MEDLINE/PubMed database. A bibliographic search was done for further additional articles. No exclusion criteria was considered, all available literature was included including anatomical studies, case reports and patients series. The articles were classified into 4 groups. Group 1- Articles describing surgical techniques; group 2- articles describing anatomical landmarks and limitations of EEA; group 3- clinical patients series and case reports; group 4- biomechanical studies. Each article in each category was reviewed; some articles were included in more than one group.
Approach demonstration: one fresh and three silicon injected embalmed cadaveric specimen heads were used to perform the approach for demonstration purpose; a computed tomography (CT) scan was done on the fresh head specimen in order to demonstrate all lines predicting the inferior limit of the approach.
Sixty-one articles and one poster were identified and reviewed.
Group 1: articles describing the surgical technique: Alfieri et al (2002) [8] first described the endoscopic endonasal approach to craniocervical junction in 2002 via an anatomical study utilizing 16 head specimens. Through the endoscopic endonasal route; they were able to expose the whole CCJ from the lower clivus up to the body of C2 without removing the nasal turbinates or the posterior part of nasal septum, this study gave the starting signal for numerous clinical and anatomical studies utilizing the EEA to CCJ. In 2005, Kassam et al [9] was the first to perform a fully endoscopic odontoidectomy in a 73-year-old woman with a history of rheumatoid arthritis and suffering from craniocervical junction ventral compression. Kassam identified his newly described approach among the expanded endoscopic approaches to the anterior skull base. One-side removal of the middle turbinate, a wide sphenoidectomy and removing 1cm of the posterior nasal septum allowed enhancing his surgical exposure. One year later, in 2006, Kassam [10] used his expanded EEA for clipping a large vertebral artery aneurysm.
In 2007 the department of neurosurgery in the University of Naples Federico II/Italy published two anatomical studies demonstrating the feasibility of the EEA to decompress the ventral CCJ and the upper cervical spinal cord [11, 12]. First one performed by Messina et al (2007) [12] who described the possibility of odontoidectomy by the EEA without any turbinectomy or even without the removal of the posterior third of the nasal septum. The second work was done by Cavallo et al (2007) [11] who exposed the entire clivus and CCJ using the expanded approach associated with opening the sphenoid sinus. The first retrospective patients' series was published in 2007 by Nayak et al [13]. Nine patients underwent endonasal endoscopic resection of the odontoid process. Since then, numerous studies have described the approach in adult and pediatric patients; they varied between patients' series, case reports and anatomical studies [14-45]. Technically, in order to access a midline lesion limited to CCJ region, many authors accept the use of two nostrils approach without turbinectomy or sphenoidectomy but with removing the posterior 1-2cm of the nasal septum to enlarge the choana and facilitate binostril application of instrumentations [16, 17, 24, 26, 29, 34]. The removal of anterior floor of the sphenoid sinus is another option to enlarge the working space [9, 10, 30, 36]. However, the use of one nostril or two nostrils technique and/or the expansion of the surgical corridor are strictly related to the lesion encroachment, surgeon's experience and/or preference.
Surgical steps: a 0° endoscope is introduced in the nostril. The free end of the middle turbinate leads to the superior lateral aspect of the choana [8]. (Figure 1 A); 1-2 cm of posterior nasal septum is removed in order to place the endoscope on midline. The line drawn between the upper edges of the Eustachian tubes Ostia crosses the ventral margin of foramina magnum "landmark" [8]. (Figure 1 B); tarious nasopharyngeal incisions could be used [25]. We demonstrate a mucosal-muscular flap, which will be pushed into mouth cavity (Figure 1 C). Bone exposure: the anterior atlanto-occipital membrane (AAOM) is removed (Figure 2 A); the anterior Arch of C1 is removed; therefore, the odontoid process and ligaments are visualized (Figure 2 B). The odontoid process is hollowed out then removed (Figure 2 C); the cruciate ligament is well exposed by removal the apical ligament and cutting out the alar ligaments (Figure 3 A); the extradural exposure could be done by removal of cruciate ligament if needed (Figure 3 B); the dura is opened for intra dural lesions (Figure 3 C).
Group 2: feasibility and anatomical limitations of the approach: the EEA to the CCJ is limited by anatomical structures, superiorly by the bony and soft tissues of the nose and inferiorly by the hard palate. Messina et al (2007) [12] stated that the possibility of performing an odontoidectomy via an endonasal route is strictly related to the level of the C1-C2 junction, which must be above the level of the horizontal hard palate, otherwise this procedure is virtually impossible. Since there, authors are trying to accurately predict the EEA limitations and thus, to choose the suitable approach for each patient without limiting the surgical exposure. The Palatine Line (PL) or the Hard-Palate Line (HPL) which drawn parallel to and along the floor of the hard palate was used as a reference in almost all studies [43, 46-52]. De Almedia et al (2009) [53] reviewed retrospectively the computed tomographic (CT) scans of 17 patients who underwent endonasal endoscopic surgery of the C1 or C2 vertebrae, they defined the nasopalatine line (NPL) connecting the most inferior point on the nasal bone (rhinion) to the most posterior point on the hard palate in the midsagittal plane, this line was called "Kassam Line" later on according to the senior author. De Almedia et al stated that the point of intersection of the NPL and the vertebral column accurately predicts the inferior limit of the surgical exposure.
Baird et al (2009) [54] based on a cadaver study on 9 specimens defined a line from the rhinion to within 3 to 5 mm from the base of the surgical resection. They stated that EEA is feasible as long as this line doesn't cross the posterior end of the hard palate. Aldana et al (2012) [55] presented a poster of 6 cadaver specimens study claiming that the previous described NPL or Kassam line overestimates the inferior limit of EEA to CCA, for that, they presented a new line, the superior nostril-hard palate line (SN-HP Line) that connects the superior aspect of the nostril to the anterior border of C1-C2 junction. Later on, the same author [46], stated that his (SN-HP Line) underestimated the inferior limit of the EEA. He described the naso-axial line (NAxL) where the starting point is the midpoint of the distance from rhinion to the anterior nasal spine of the maxillary bone and a second point is the tip of the posterior nasal spine of palatine bone. The line then extended to end at the spine column. Singh et al (2013) [51] analyzed the CT scan of 100 patients and found an inverse relationship between hard palate length and the lowest zone of the cervical spine potentially visualized by nasal endoscopy, this was the first study where the visualization by a 0, 30 and 45-degree endoscope was simulated. Same authors completed their clinical study by a second anatomical part [52] and concluded that the use of a 30-degree endoscope and neck extension increased the degree of exposure down the cervical spine.
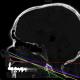
Lin et al (2014) [56] stated in their radiological study on 34 patients that there is no influence of the position of the cervical spine on the surgical convenience of the endoscopic transnasal approach. La Corte et al (2015) [50], found that the previous described NaxL overpredicted the approach limits, for that and depending on CT scan performed in patients who underwent an odontoidectomy, they described a new line, the Rhinopalatine Line (RPL) where the starting point corresponds to the two-thirds point of the distance from the rhinion to the anterior nasal spine of the maxillary bone and a second point at the posterior nasal spine of the palatine bone. The line is then extended to end at the cervical spine. Corte et al. stated that their new described line is the most accurate one that predicts the actual inferior limit of EEA to CCJ. The main lines described in literature to predict the inferior limitation of EEA to CCJ are summarized in Table 1 and Figure 4.
Group 3: indications: a variety of pathological lesions can affect the CCJ; ventral compression of this region can be produced by neoplasms, congenital disorders, infections, degenerative diseases and posttraumatic conditions [57]. The EEA to CCJ was first used by Kassam et al (2005) [9] to perform an odontoidectomy. Since then, the odontoidectomy is widely performed by the EEA as a treatment of congenital and acquired lesions causing compression of the ventral CCJ [13, 15, 18-21, 23, 24, 26, 35, 39, 44] including pediatric patients as well [14, 22, 30-32, 38, 40]. Most recent review of literature [58, 59] concluded that the rheumatoid pannus and basilar invagination were the most common indication of EEA to CCJ. Other case reports described the use of EEA approach for aneurysm clipping on the vertebral artery [10], for the excision of ventral posterior fossa meningioma [60] and for tuberculosis [61]. Recently, Mendez et al (2015) [62], by a cadaveric study, demonstrated the feasibility of C1-2 fusion via EEA, this novel technique could be the alternative of the second time C1-C2 posterior fixation.
Group 4: biomechanical stability following the approach: the CCJ moves in three directions, flexion-extension, axial rotation and lateral bending. Two cadaveric biomechanical studies [63, 64] from St. Joseph's Hospital, Phoenix, Arizona, USA concluded that the removal of the inferior-third of clivus associated with an intradural exposure to the ventral CCJ and foramen magnum led to hypermobility at Occiput-C1 junction. However, these studies stated that the craniocervical fusion is clinically indicated only after removal of 75% of anterior condyle. The EEA to CCJ provides the possibility to avoid the morbidity of the transoral approach by keeping the incision in the nasopharynx above the level of the soft palate; therefore, it affects early extubation and early feeding [60, 65]. The approach provides sufficient surgical field [54] and through it, selected cases of odontoidectomy can be performed with the preservation of C1 anterior arch, thus, it potentially reduces the instability of CCJ [18, 20, 66, 67]. Additional techniques to support the approach have been proposed. Some authors use the navigation [18, 24, 28, 29, 42, 68]; others offered a technique to preserve the mucosal integrity of the posterior nasal septum and pedicled nasoseptal flap [69]; the combination with the trans oral approach was also described [17, 70]. The main challenge of the EEA to CCJ is the presence of anatomical structures that can limit the surgical approach, including the bony and soft tissues of the nose superiorly and the hard palate inferiorly. Many studies aimed to determine the feasibility of the approach by using anatomical landmarks to determine the inferior limit and by studying the effect of head and neck position in widening the surgical field [12, 25, 46-56]
This is the first paper reviewing all available clinical, anatomical and biomechanical studies on the EEA to CCJ. This unique approach went through significant steps of evolution since its first description in 2002. The EEA became the approach of choice to the ventral CCJ. It is significantly less invasive compared to the trans oral approach and carries less potential side effects. The accurate prediction of the inferior limitation is now potentially feasible. However, we still need a standard method to evaluate the limitations. The approach still needs a work out to be applied for more indications especially the fusion.
What is known about this topic
- Two papers reviewed the available literature (clinical series) about the endoscopic endonasal approach to craniocervical junction.
What this study adds
- This is the first paper that covers all the available literature including the cadaveric studies and the case reports as well.
The authors declare no competing interest.
All the authors have read and agreed to the final manuscript.
The realization of this work was possible thanks to those who donated their bodies. The authors sincerely appreciate and gratefully acknowledge the donators and their families.
Table 1: lines predicting the inferior limit of the EEA to CCJ
Figure 1: (A) 0° endoscope
is introduced in left nostril of fresh head specimen the free end of the middle
turbinate leads to the superior lateral aspect of the choana: (Alfieri et al)
IT= inferior turbinate; MT= Middle turbinate; NF= Nasal floor; NS = Nasal septum;
Co= Choana; ET= Eustachian tube; (B) removal of 1-2 cm of posterior nasal septum,
the endoscope is placed on midline. RMF = Rosenmüller
fossa; SPT = Soft palate; NPX = Nasopharynx; the line drawn between the upper
edges of the eustachian tubes ostia (dashed line) crosses the ventral margin
of foramina
magnum "landmark" (Alfieri et al 2002); (C) mucosal-muscular flap was
done
and
pushed into mouth cavity VSJ= Spheno-vomer junction; AAOM= Anterior Atlanto-occipital
membrane (or ligament)
Figure 2: (A) bone exposure
after removal of AAOM: PhT = Pharyngeal tubercle of clivus; FM = Foramina magnum;
OdT= Odontoid tip; C1 = Anterior arch of C1; (B) embalmed specimen: removal of
anterior arch of C1 apL = Apical ligament; OD= Odontoid process; (C) the odontoid
process was hollowed out and removed; the clivus was partially drilled in order
to well demonstrate the apical ligament (ApL); the C1 superior articular process
was also partially drilled on each side to show the Alar ligaments (ALL) TL =
transverse portion of cruciate ligament
Figure 3: (A) the apical ligament was removed; the alar ligaments were cut out. The C2 body and was partially drilled CxL= Cruciate ligament; Occ = occipital condyle; (B) removal of cruciate ligament TcM= Tectorial membrane; (C) intradural view (sutures were applied on dura by transoral route for demonstration purpose C1Nv = C1 ventral nerve roots; DnL= dentate ligament; ASA = Anterior spinal artery; VA= vertebral artery; PICA= Posterior inferior cerebellar artery; AICA = Anterior inferior cerebellar artery; BA = Basilar artery
Figure 4: lines predicting
the inferior limits of EEA to CCJ, NPL (green), SN-HP Line (blue), NAxL (yellow),
RPL (Purple), the hard palate line (HPL) is also shown in dashed red
- Apuzzo ML, Weiss MH, Heiden JS. Transoral exposure of the atlantoaxial region. Neurosurgery. 1978; 3(2): 201-7. PubMed | Google Scholar
- Crockard HA, Calder I, Ransford AO. One-stage transoral decompression and posterior fixation in rheumatoid atlanto-axial subluxation. J Bone Joint Surg Br. 1990; 72(4): 682-5. PubMed | Google Scholar
- Dickman CA, Locantro J, Fessler RG. The influence of transoral odontoid resection on stability of the craniovertebral junction. J Neurosurg. 1992; 77(4): 525-30. PubMed | Google Scholar
- Frempong-Boadu AK, Faunce WA, Fessler RG. Endoscopically assisted transoral-transpharyngeal approach to the craniovertebral junction. Neurosurgery. 2002; 51(5): 60-6. PubMed | Google Scholar
- Menezes AH, VanGilder JC. Transoral-transpharyngeal approach to the anterior craniocervical junction: ten-year experience with 72 patients. J Neurosurg. 1988; 69(6): 895-903. PubMed | Google Scholar
- Crockard HA. Transoral surgery: some lessons learned. Br J Neurosurg. 1995; 9(3): 283-93. PubMed | Google Scholar
- Deopujari CE, Karmarkar VS, Shah NJ. Endoscopic approaches to the craniovertebral junction and odontoid process. World Neurosurg. 2014; 82(6): 49-53. PubMed | Google Scholar
- Alfieri A, Jho HD, Tschabitscher M. Endoscopic endonasal approach to the ventral cranio-cervical junction: anatomical study. Acta Neurochir (Wien). 2002; 144(3): 219-25. PubMed | Google Scholar
- Kassam AB, Snyderman C, Gardner P, Carrau R, Spiro R. The expanded endonasal approach: a fully endoscopic transnasal approach and resection of the odontoid process: technical case report. Neurosurgery. 2005; 57(1): 213. PubMed | Google Scholar
- Kassam AB, Mintz AH, Gardner PA, Horowitz MB, Carrau RL, Snyderman CH. The expanded endonasal approach for an endoscopic transnasal clipping and aneurysmorrhaphy of a large vertebral artery aneurysm: technical case report. Neurosurgery. 2006; 59(1): 162-5. PubMed | Google Scholar
- Cavallo LM, Cappabianca P, Messina A, Esposito F, Stella L, de Divitiis E, Tschabitscher M. The extended endoscopic endonasal approach to the clivus and cranio-vertebral junction: anatomical study. Childs Nerv Syst. 2007; 23(6): 665-71. PubMed | Google Scholar
- Messina A, Bruno MC, Decq P, Coste A, Cavallo LM, de Divittis E et al. Pure endoscopic endonasal odontoidectomy: anatomical study. Neurosurg Rev. 2007; 30(3): 189-94. PubMed | Google Scholar
- Nayak JV, Gardner PA, Vescan AD, Carrau RL, Kassam AB, Snyderman CH. Experience with the expanded endonasal approach for resection of the odontoid process in rheumatoid disease. Am J Rhinol. 2007; 21(5): 601-6. PubMed | Google Scholar
- Beech TJ, McDermott AL, Kay AD, Ahmed SK. Endoscopic endonasal resection of the odontoid peg-case report and literature review. Childs Nerv Syst. 2012; 28(10): 1795-9. PubMed | Google Scholar
- Cornelius JF, Kania R, Bostelmann R, Herman P, George B. Transnasal endoscopic odontoidectomy after occipito-cervical fusion during the same operative setting-technical note. Neurosurg Rev. 2011; 34(1): 115-21. PubMed | Google Scholar
- Menezes AH. Craniovertebral junction database analysis: incidence, classification, presentation and treatment algorithms. Childs Nerv Syst. 2008; 24(10): 1101-8. PubMed | Google Scholar
- Dlouhy BJ, Dahdaleh NS, Menezes AH. Evolution of transoral approaches, endoscopic endonasal approaches and reduction strategies for treatment of craniovertebral junction pathology: a treatment algorithm update. Neurosurg. 2015; 38(4): 8. PubMed | Google Scholar
- Duntze J, Eap C, Kleiber JC, Theret E, Dufour H, Fuentes S, Litre CF. Advantages and limitations of endoscopic endonasal odontoidectomy: a series of nine cases. Orthop Traumatol Surg Res. 2014; 100(7): 775-8. PubMed | Google Scholar
- Gempt J, Lehmberg J, Grams AE, Berends L, Meyer B, Stoffel M. Endoscopic transnasal resection of the odontoid: case series and clinical course. Eur Spine J. 2011; 20(4): 661-6. PubMed | Google Scholar
- Gladi M, Iacoangeli M, Specchia N, Re M, Dobran M, Alvaro L, Moriconi E, Scerrati M. Endoscopic transnasal odontoid resection to decompress the bulbo-medullary junction: a reliable anterior minimally invasive technique without posterior fusion. Eur Spine J. 2012; 21(1): 55-60. PubMed | Google Scholar
- Grammatica A, Bonali M, Ruscitti F, Marchioni D, Pinna G, Cunsolo EM, Presutti L. Transnasal endoscopic removal of malformation of the odontoid process in a patient with type I Arnold-Chiari malformation: a case report. Acta Otorhinolaryngol Ital. 2011; 31(4): 248-52. PubMed | Google Scholar
- Hankinson TC, Grunstein E, Gardner P, Spinks TJ, Anderson RC. Transnasal odontoid resection followed by posterior decompression and occipitocervical fusion in children with Chiari malformation Type I and ventral brainstem compression. J Neurosurg Pediatr. 2010; 5(6): 549-53. PubMed | Google Scholar
- Hansen MA, Da Cruz MJ, Owler BK. Endoscopic transnasal decompression for management of basilar invagination in osteogenesis imperfecta. J Neurosurg Spine. 2008; 9(4): 354-57. PubMed | Google Scholar
- Hickman ZL, McDowell MM, Barton SM, Sussman ES, Grunstein E, Anderson RC. Transnasal endoscopic approach to the pediatric craniovertebral junction and rostral cervical spine: case series and literature review. Neurosurg. 2013; 35(2): 14. PubMed | Google Scholar
- La Corte E, Aldana PR, Schiariti M, Maccari A, Ferroli P. Endoscopic approaches to the craniovertebral junction. Acta Neurochir. 2014; 156(2): 293-5. PubMed | Google Scholar
- Laufer I, Greenfield JP, Anand VK, Hartl R, Schwartz TH. Endonasal endoscopic resection of the odontoid process in a nonachondroplastic dwarf with juvenile rheumatoid arthritis: feasibility of the approach and utility of the intraoperative Iso-C three-dimensional navigation: case report. J Neurosurg Spine. 2008; 8(4): 376-80. PubMed | Google Scholar
- Lee A, Sommer D, Reddy K, Murty N, Gunnarsson T. Endoscopic transnasal approach to the craniocervical junction. Skull Base. 2010; 20(3): 199-205. PubMed | Google Scholar
- Leng LZ, Anand VK, Hartl R, Schwartz TH. Endonasal endoscopic resection of an os odontoideum to decompress the cervicomedullary junction: a minimal access surgical technique. Spine. 2009; 34(4): 139-43. PubMed | Google Scholar
- Liu JK, Patel J, Goldstein IM, Eloy JA. Endoscopic endonasal transclival transodontoid approach for ventral decompression of the craniovertebral junction: operative technique and nuances. Neurosurg. 2015; 38(4): 17. PubMed | Google Scholar
- Magrini S, Pasquini E, Mazzatenta D, Mascari C, Galassi E, Frank G. Endoscopic endonasal odontoidectomy in a patient affected by Down syndrome: technical case report. Neurosurgery. 2008; 63(2): 373-4. PubMed | Google Scholar
- Nagpal T. Transnasal endoscopic removal of malformation of the odontoid process in craniovertebral anomaly: a case report. Kulak Burun Bogaz Ihtis Derg. 2013; 23(2): 123-6. PubMed | Google Scholar
- Patel AJ, Boatey J, Muns J, Bollo RJ, Whitehead WE, Giannoni CM, Jea A. Endoscopic endonasal odontoidectomy in a child with chronic type 3 atlantoaxial rotatory fixation: case report and literature review. Childs Nerv Syst. 2012; 28(11): 1971-5. PubMed | Google Scholar
- Ponce-Gomez JA, Ortega-Porcayo LA, Soriano-Baron HE, Sotomayor-Gonzalez A, Arriada-Mendicoa N, Gomez-Amador JL et al. Evolution from microscopic transoral to endoscopic endonasal odontoidectomy. Neurosurg. 2014; 37(4): 15. PubMed | Google Scholar
- Rawal RB, Shah RN, Zanation AM. Endonasal odontoidectomy for basilar impression and brainstem compression due to radiation fibrosis. Laryngoscope. 2013; 123(3): 584-7. PubMed | Google Scholar
- Scholtes F, Signorelli F, McLaughlin N, Lavigne F, Bojanowski MW. Endoscopic endonasal resection of the odontoid process as a standalone decompressive procedure for basilar invagination in Chiari type I malformation. Minim Invasive Neurosurg . 2011; 54(4): 179-82. PubMed | Google Scholar
- Seker A, Inoue K, Osawa S, Akakin A, Kilic T, Rhoton AL Jr. Comparison of endoscopic transnasal and transoral approaches to the craniovertebral junction. World Neurosurg. 2010; 74(6): 583-602. PubMed | Google Scholar
- Singh H, Harrop J, Schiffmacher P, Rosen M, Evans J. Ventral surgical approaches to craniovertebral junction chordomas. Neurosurgery. 2010; 66(3): 96-103. PubMed | Google Scholar
- Sinha S, Mirza S, Bishop N, Zaki H, McMullan J. Endoscopic endonasal resection of the odontoid peg for paediatric basilar invagination. Br J Neurosurg. 2012; 26(4): 487-9. PubMed | Google Scholar
- Tanriverdi O, Tugcu B, Gunaldi O, Baydin SS, Demirgil BT, Sam B, et al. The selective odontoidectomy: endoscopic endonasal approach to the craniocervical junction. J Craniofac Surg. 2014; 25(4): 1482-7. PubMed | Google Scholar
- Tomazic PV, Stammberger H, Mokry M, Gerstenberger C, Habermann W. Endoscopic resection of odontoid process in Arnold Chiari malformation type II. B-ENT. 2011; 7(3): 209-13. PubMed | Google Scholar
- Visocchi M. Transnasal andtransoral approach to the clivus and the craniovertebral junction. J Neurosurg Sci. 2015. PubMed | Google Scholar
- Wu JC, Huang WC, Cheng H, Liang ML, Ho CY, Wong TT et al. Endoscopic transnasal transclival odontoidectomy: a new approach to decompression: technical case report. Neurosurgery. 2008; 63(1): 92-4. PubMed | Google Scholar
- Yen YS, Chang PY, Huang WC, Wu JC, Liang ML, Tu TH, Cheng H. Endoscopic transnasal odontoidectomy without resection of nasal turbinates: clinical outcomes of 13 patients. J Neurosurg Spine. 2014; 21(6): 929-37. PubMed | Google Scholar
- Yu Y, Wang X, Zhang X, Hu F, Gu Y, Xie T, Jiang X, Jiang C. Endoscopic transnasal odontoidectomy to treat basilar invagination with congenital osseous malformations. Eur Spine J. 2013; 22(5): 1127-36. PubMed | Google Scholar
- Zoli M, Mazzatenta D, Valluzzi A, Mascari C, Pasquini E, Frank G. Endoscopic Endonasal Odontoidectomy. Neurosurg Clin N Am. 2015; 26(3): 427-36. PubMed | Google Scholar
- Aldana PR, Naseri I, La Corte E. The naso-axial line: a new method of accurately predicting the inferior limit of the endoscopic endonasal approach to the craniovertebral junction. Neurosurgery. 2012; 71(2 Suppl Operative): 308-14. PubMed | Google Scholar
- Burke K, Benet A, Aghi MK, El-Sayed I. Impact of platybasia and anatomic variance on surgical approaches to the craniovertebral junction. Laryngoscope. 2014; 124(8): 1760-6. PubMed | Google Scholar
- El-Sayed IH, Wu JC, Ames CP, Balamurali G, Mummaneni PV. Combined transnasal and transoral endoscopic approaches to the craniovertebral junction. J Craniovertebr Junction Spine. 2010; 1(1): 44-8. PubMed | Google Scholar
- El-Sayed IH, Wu JC, Dhillon N, Ames CP, Mummaneni P. The importance of platybasia and the palatine line in patient selection for endonasal surgery of the craniocervical junction: a radiographic study of 12 patients. World Neurosurg. 2011; 76(1-2): 183-8. PubMed | Google Scholar
- La Corte E, Aldana PR, Ferroli P, Greenfield JP, Hartl R, Anand VK et al. The rhinopalatine line as a reliable predictor of the inferior extent of endonasal odontoidectomies. Neurosurg. 2015; 38(4): 16. PubMed | Google Scholar
- Singh H, Grobelny BT, Harrop J, Rosen M, Lober RM, Evans J. Endonasal access to the upper cervical spine, part one: radiographic morphometric analysis. J Neurol Surg B Skull Base. 2013; 74(3): 176-84. PubMed | Google Scholar
- Singh H, Lober RM, Virdi GS, Lopez H, Rosen M, Evans J. Endonasal Access to the Upper Cervical Spine: Part 2-Cadaveric Analysis. J Neurol Surg B Skull Base. 2015; 76(4): 262-5. PubMed | Google Scholar
- Almeida JR, Zanation AM, Snyderman CH, Carrau RL, Prevedello DM, Gardner PA, Kassam AB. Defining the nasopalatine line: the limit for endonasal surgery of the spine. Laryngoscope. 2009; 119(2): 239-44. PubMed | Google Scholar
- Baird CJ, Conway JE, Sciubba DM, Prevedello DM, Quinones-Hinojosa A, Kassam AB. Radiographic and anatomic basis of endoscopic anterior craniocervical decompression: a comparison of endonasal, transoral, and transcervical approaches. Neurosurgery. 2009; 65(6): 158-63. PubMed | Google Scholar
- Aldana P, Roy S. Preoperative prediction of the limits of endoscopic endonasal and transoral approaches to the craniovertebral junction: an image-guided cadaveric dissection. In: the Congress of Neurological Surgeons Annual Meeting. Washington, DC, 2011. Google Scholar
- Lin ZK, Chi YL, Wang XY, Yu Q, Fang BD, Wu LJ. The influence of cervical spine position on the three anterior endoscopic approaches to the craniovertebral junction: an imaging study. Spine J. 2014; 14(1): 80-6. PubMed | Google Scholar
- Menezes AH, VanGilder JC, Graf CJ, McDonnell DE. Craniocervical abnormalities: a comprehensive surgical approach. J Neurosurg. 1980; 53(4): 444-55. PubMed | Google Scholar
- Fang CH, Friedman R, Schild SD, Goldstein IM, Baredes S, Liu JK et al. Purely endoscopic endonasal surgery of the craniovertebral junction: A systematic review. Int Forum Allergy Rhinol. 2015; 5(8): 754-60. PubMed | Google Scholar
- Morales-Valero SF, Serchi E, Zoli M, Mazzatenta D, Van Gompel JJ. Endoscopic endonasal approach for craniovertebral junction pathology: a review of the literature. Neurosurg. 2015; 38(4): 15. PubMed | Google Scholar
- Beer-Furlan A, Vellutini EA, Balsalobre L, Stamm AC. Endoscopic Endonasal Approach to Ventral Posterior Fossa Meningiomas: From Case Selection to Surgical Management. Neurosurg Clin N Am. 2015; 26(3): 413-26. PubMed | Google Scholar
- Puraviappan P, Tang IP, Yong DJ, Prepageran N, Carrau RL, Kassam AB. Endoscopic, endonasal decompression of spinal stenosis with myelopathy secondary to cranio-vertebral tuberculosis: two cases. J Laryngol Otol. 2010; 124(7): 816-9. PubMed | Google Scholar
- Mendes GA, Dickman CA, Rodriguez-Martinez NG, Kalb S, Crawford NR, Sonntag VK, et al. Endoscopic endonasal atlantoaxial transarticular screw fixation technique: an anatomical feasibility and biomechanical study. J Neurosurg Spine. 2015; 22(5): 470-7. PubMed | Google Scholar
- Little AS, Perez-Orribo L, Rodriguez-Martinez NG, Reyes PM, Newcomb AG, Prevedello DM, et al. Biomechanical evaluation of the craniovertebral junction after inferior-third clivectomy and intradural exposure of the foramen magnum: implications for endoscopic endonasal approaches to the cranial base. J Neurosurg Spine. 2013; 18(4): 327-32. PubMed | Google Scholar
- Perez-Orribo L, Little AS, Lefevre RD, Reyes PR, Newcomb AG, Prevedello DMR et al. Biomechanical evaluation of the craniovertebral junction after anterior unilateral condylectomy: implications for endoscopic endonasal approaches to the cranial base. Neurosurgery. 2013; 72(6): 1029-30. PubMed | Google Scholar
- Goldschlager T, Hartl R, Greenfield JP, Anand VK, Schwartz TH. The endoscopic endonasal approach to the odontoid and its impact on early extubation and feeding. J Neurosurg. 2015; 122(3): 511-8. PubMed | Google Scholar
- Iacoangeli M, Gladi M, Alvaro L, Di Rienzo A, Specchia N, Scerrati M. Endoscopic endonasal odontoidectomy with anterior C1 arch preservation in elderly patients affected by rheumatoid arthritis. Spine J. 2013; 13(5): 542-8. PubMed | Google Scholar
- Mazzatenta D, Zoli M, Mascari C, Pasquini E, Frank G. Endoscopic endonasal odontoidectomy: clinical series. Spine. 2014; 39(10): 846-53. PubMed | Google Scholar
- Choudhri O, Mindea SA, Feroze A, Soudry E, Chang SD, Nayak JV. Experience with intraoperative navigation and imaging during endoscopic transnasal spinal approaches to the foramen magnum and odontoid. Neurosurg. 2014; 36(3): 4. PubMed | Google Scholar
- Eloy JA, Vazquez A, Mady LJ, Patel CR, Goldstein IM, Liu JK. Mucosal-sparing posterior septectomy for endoscopic endonasal approach to the craniocervical junction. Am J Otolaryngol. 2015; 36(3): 342-6. PubMed | Google Scholar
- Carrau RL, Prevedello DM, de Lara D, Durmus K, Ozer E. Combined transoral robotic surgery and endoscopic endonasal approach for the resection of extensive malignancies of the skull base. Head Neck. 2013; 35(11): 351-58. PubMed | Google Scholar
Search
This article authors
On Pubmed
On Google Scholar
Citation [Download]
Navigate this article
Similar articles in
Key words
Tables and figures
 Figure 1: (A) 0° endoscope is introduced in left nostril of fresh head specimen the free end of the middle turbinate leads to the superior lateral aspect of the choana: (Alfieri et al) IT= inferior turbinate; MT= Middle turbinate; NF= Nasal floor; NS = Nasal septum; Co= Choana; ET= Eustachian tube; (B) removal of 1-2 cm of posterior nasal septum, the endoscope is placed on midline. RMF = Rosenmüller fossa; SPT= Soft palate; NPX = Nasopharynx; the line drawn between the upper edges of the eustachian tubes ostia (dashed line) crosses the ventral margin of foramina magnum "landmark" (Alfieri et al 2002); (C) mucosal-muscular flap was done and pushed into mouth cavity VSJ = Spheno-vomer junction; AAOM = Anterior Atlanto-occipital membrane (or ligament)
Figure 1: (A) 0° endoscope is introduced in left nostril of fresh head specimen the free end of the middle turbinate leads to the superior lateral aspect of the choana: (Alfieri et al) IT= inferior turbinate; MT= Middle turbinate; NF= Nasal floor; NS = Nasal septum; Co= Choana; ET= Eustachian tube; (B) removal of 1-2 cm of posterior nasal septum, the endoscope is placed on midline. RMF = Rosenmüller fossa; SPT= Soft palate; NPX = Nasopharynx; the line drawn between the upper edges of the eustachian tubes ostia (dashed line) crosses the ventral margin of foramina magnum "landmark" (Alfieri et al 2002); (C) mucosal-muscular flap was done and pushed into mouth cavity VSJ = Spheno-vomer junction; AAOM = Anterior Atlanto-occipital membrane (or ligament)
 Figure 2: (A) bone exposure after removal of AAOM: PhT = Pharyngeal tubercle of clivus; FM = Foramina magnum; OdT= Odontoid tip; C1 = Anterior arch of C1; (B) embalmed specimen: removal of anterior arch of C1 apL = Apical ligament; OD= Odontoid process; (C) the odontoid process was hollowed out and removed; the clivus was partially drilled in order to well demonstrate the apical ligament (ApL); the C1 superior articular process was also partially drilled on each side to show the Alar ligaments (ALL) TL = transverse portion of cruciate ligament
Figure 2: (A) bone exposure after removal of AAOM: PhT = Pharyngeal tubercle of clivus; FM = Foramina magnum; OdT= Odontoid tip; C1 = Anterior arch of C1; (B) embalmed specimen: removal of anterior arch of C1 apL = Apical ligament; OD= Odontoid process; (C) the odontoid process was hollowed out and removed; the clivus was partially drilled in order to well demonstrate the apical ligament (ApL); the C1 superior articular process was also partially drilled on each side to show the Alar ligaments (ALL) TL = transverse portion of cruciate ligament
 Figure 3: (A) the apical ligament was removed; the alar ligaments were cut out. The C2 body and was partially drilled CxL= Cruciate ligament; Occ = occipital condyle; (B) removal of cruciate ligament TcM= Tectorial membrane; (C) intradural view (sutures were applied on dura by transoral route for demonstration purpose C1Nv = C1 ventral nerve roots; DnL= dentate ligament; ASA = Anterior spinal artery; VA= vertebral artery; PICA= Posterior inferior cerebellar artery; AICA = Anterior inferior cerebellar artery; BA = Basilar artery
Figure 3: (A) the apical ligament was removed; the alar ligaments were cut out. The C2 body and was partially drilled CxL= Cruciate ligament; Occ = occipital condyle; (B) removal of cruciate ligament TcM= Tectorial membrane; (C) intradural view (sutures were applied on dura by transoral route for demonstration purpose C1Nv = C1 ventral nerve roots; DnL= dentate ligament; ASA = Anterior spinal artery; VA= vertebral artery; PICA= Posterior inferior cerebellar artery; AICA = Anterior inferior cerebellar artery; BA = Basilar artery