Impact of training intervention on immunization providers’ knowledge and practice of routine immunization in Ibadan, south-western Nigeria: a primary health care experience
Victoria Bolanle Brown, Oyeninhun Abimbola Oluwatosin, Martins Olusola Ogundeji
Corresponding author: Victoria Bolanle Brown, School of Nursing, University College Hospital, Ibadan, Nigeria 
Received: 31 Dec 2016 - Accepted: 16 Apr 2017 - Published: 24 Apr 2017
Domain: Public Health
Keywords: Immunization, knowledge, practice, health-providers, training, intervention
©Victoria Bolanle Brown et al. Pan African Medical Journal (ISSN: 1937-8688). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Victoria Bolanle Brown et al. Impact of training intervention on immunization providers’ knowledge and practice of routine immunization in Ibadan, south-western Nigeria: a primary health care experience. Pan African Medical Journal. 2017;26:216. [doi: 10.11604/pamj.2017.26.216.11545]
Available online at: https://www.panafrican-med-journal.com//content/article/26/216/full
Original article 
Impact of training intervention on immunization providers’ knowledge and practice of routine immunization in Ibadan, south-western Nigeria: a primary health care experience
Impact of training intervention on immunization providers’ knowledge and practice of routine immunization in Ibadan, south-western Nigeria: a primary health care experience
Victoria Bolanle Brown1,&, Oyeninhun Abimbola Oluwatosin2, Martins Olusola Ogundeji3
1School of Nursing, University College Hospital, Ibadan, Nigeria, 2Department of Nursing, Faculty of Clinical Sciences, College of Medicine, University of Ibadan, Nigeria, 3Primary Health Care and Health Management Centre (PriHEMAC), Ibadan, Nigeria
&Corresponding author
Victoria Bolanle Brown, School of Nursing, University College Hospital, Ibadan, Nigeria
Introduction: immunization coverage rate in Nigeria is low for controlling vaccine-preventable-diseases. To improve immunization service delivery, regular training of health providers is essential. Few studies have evaluated the effect of immunization training on performance of providers in Primary Health Care (PHC) setting. We assessed the impact of immunization training intervention on knowledge and practice of immunization providers in Ibadan, Nigeria.
Methods: a pre-test, post-test experimental design was adopted; four randomly selected Local Government Areas (LGAs) were randomly assigned into two intervention and two control groups. One ward was randomly selected from each LGA. Participants were 70 immunization providers from PHC centers from the four wards. A two-day immunization training was organized for the participants in the intervention groups. Knowledge and practice data were collected from all participants with a questionnaire and an observation checklist pre-intervention, immediately, three months and six months post-intervention.
Results: repeated measures ANOVA revealed a statistically significant improvement in the scores of the participants in intervention groups in all the three parameters of questionnaire assessment between time points, general knowledge of immunization and self-reported practice (F= 8.235, P< 0.001), gathering immunization information from community (F= 2.919, P< 0.05) and communication with mothers about immunization (F=17.913, P< 0.001). However, the mean scores for observation of participants’ communication practice with mothers on immunization across four points of assessment in all the groups showed no significant improvement (P> 0.05).
Conclusion: there is a need for effective monitoring and supportive supervision system to ensure standard immunization practice in the context of task-shifting initiatives in PHC.
Increasing immunization levels for under-five children is one of the highest priorities for the Immunization Program [1]. The purpose of the immunization program is to achieve high vaccination rates to control vaccine- preventable-diseases (VPDs) among groups who are susceptible to the diseases and reduce morbidity and mortality among them. There is ample evidence that health service provider practices are a key determinant of vaccination coverage among children [2, 3]. Knowledge and attitudes of healthcare providers have significant impact on frequency with which vaccines are offered and accepted [4, 5]. Educational interventions on immunization providers have been found to improve immunization providers’ knowledge and practice and increase immunization uptake [6-9]. Although the different immunization strategies adopted in Nigeria has brought some improvement to immunization uptake among children, the coverage level is still below the recommended 90% level for the sustained control of VPDs [10]. Strengthening routine immunization is one of the child survival strategies in Nigeria. It is notable that a committed, confident and competent vaccination workforce is integral to ensuring high vaccine coverage [11]. In order to provide effective immunization services, Primary Health Care (PHC) providers who work at the grassroot should have up-to-date information about immunization on regular basis to keep them well versed with the basics of immunization and the prevailing practices pertaining to immunization program. Since health professionals’ attitudes and actions will reflect their training and development, continuing education can improve their knowledge base and skill level, it can change their behaviors and attitudes, and improve health outcomes [11, 12].
The federal system of government in Nigeria functions at three tiers: national, state and local governments. The Local Government Area (LGA) is primarily responsible for routine immunization delivery and other PHC services, though the state government provide some supervision and resources to enable service delivery. The federal government, through the National Primary Health Care Development (NPHCDA) sets the overall direction and mobilizes resources at the federal level [13]. In an attempt to improve access to health care, NPHCDA developed a ward health system through which a minimum health care package would be delivered. The Nigeria National Health Policy recognized the Local Government Area (LGA) as the operational level for PHC implementation. A ward is the smallest political structure, consisting of a geographical area with a population range of 10,000 to 30,000 people. There are on average, ten (10) wards per LGA, each represented by an elected councilor. The main rationale for selecting a ward as an operational area for delivering a minimum health care package was to mobilize political commitment to health service delivery as a requisite for social development. A ward has at least one PHC center [14]. Routine immunization services at PHC level are being delivered by nurses and midwives as well as some cadres of community health workers. The community health workers are substitute health personnel [15] trained to staff PHC centers through task shifting scheme. The community health workers are in three categories; the Community Health Officer (CHO), Community Health Extension Worker (CHEW), and Junior Community Health Extension Worker (JCHEW). Poor commitment to vaccination services, inadequate knowledge level regarding vaccinations, poor attitude, poor performance/competence of health workers and their inability to communicate effectively with mothers about immunization have been identified as some of the reasons children are not vaccinated in Nigeria [16]. In order to improve immunization providers’ knowledge and practice, the National Immunization Policy of 2009 in Nigeria [17] stated guidelines for mandatory continuous on-the-job training for health workers on immunization bi-annually. However, it is not certain that this aspect of the policy is effectively implemented at all levels of health care. Also, few studies have evaluated the effect of immunization training on performance of immunization providers in PHC in the study setting, the goal of this study therefore was to assess the impact of immunization training intervention on knowledge and self-reported practice of immunization providers in selected wards in Ibadan, south-western Nigeria.
Design: a pre-test, post-test experimental design was adopted. The study was conducted in Ibadan, south-western Nigeria. Four LGAs (two urban and two sub-urban) were randomly selected through a multi-stage sampling and randomly assigned to either training intervention group or control group and one ward was randomly selected from each LGA. Overall, a total of four wards widely spread apart were used for the recruitment of participants for the study, two wards for intervention groups (groups B and C) and two wards for the control groups (groups A and D).
Study population: participants were nurses, midwives, Community Health Officers (CHOs), Community Health Extension Workers (CHEWs), and Junior Community Health Extension Worker (JCHEW)s who were responsible for immunization service delivery at PHC level. Estimation [18,19] of the power of the study and solving for power (1- β) in the equation:
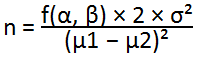
Where µ1 and µ2 are the mean outcome in the control and experimental group respectively, s is the standard deviation; f(α, β) = [Φ-1(α/2) + Φ-1(β)] 2
Assuming that each group starts with a mean knowledge score of 100 and standard deviation 16, this sample size has 89% power to detect a mean increase of 16 points (~ 1 SD unit) in knowledge scores in the intervention group versus the control group, assuming a significance level (β) of 0.05. The power to detect a mean increase of 12 points (~0.75 SD units) is 68%, under the same assumptions. The study inclusion criteria were being a PHC immunization provider (that is a nurse, a midwife, a Community Health Officer (CHO) or a Community Health Extension Workers (CHEWs.), having worked for at least three months in any PHC center in the selected wards and non-participation in any form of immunization training within six months prior to the commencement of the study.
Data collection: ethical approval was obtained for the study from the Oyo State Research Ethical Review Committee before the commencement of the data collection. Written informed consent was obtained from each participant. The questionnaire used for assessing immunization providers pre-and post-intervention had four sections: Section A assessed the socio-demographic and professional characteristics of the participants. Section B assessed the immunization providers’ knowledge and self-reported practice which included questions on participants’ knowledge of vaccine-preventable diseases, vaccines and vaccine administration, cold-chain, safe injection practices, conducting immunization sessions and their knowledge of the contraindications and side effects of each vaccine. Section C assessed their knowledge and self-reported practice on building community support for immunization and gathering immunization information from the community. Section D assessed the knowledge and self-reported practice of communication with mothers about immunization. The questions in the questionnaire were drawn from the immunization training question database developed by WHO. The reliability of the instruments was estimated through test- retest method and correlation coefficient was r = 0.90. A checklist was used for direct observation and assessment of participants’ communication practice with the mothers about immunization. This was done in the PHC centers where the participants work. The direct observations were conducted at every stage of the study (pre-intervention and post-intervention). The observation checklist contained 29 items. These items included all the variables that are considered to be essential for health educating mothers on immunization as well as documentation of all necessary immunization information. Pre- training intervention assessments were conducted at the beginning of each training workshop before the distribution of training materials and commencement of training. The questionnaires were self-administered while the direct observations were conducted by one of the researchers. Post-intervention assessments were conducted immediately after training, three months and six months after the training.
Training intervention package
This is the manual for training PHC immunization providers. The manual consisted of four culturally acceptable modules adapted by the researcher from two manuals on immunization training developed by WHO. The first WHO manual “Identifying and Overcoming Obstacles to Increase Immunization Coverage in Health Catchment Area was developed in 1997 and the second one “Immunization in Practice: a Resource Guide for Health Workers” was developed in 2004 [20,21]. The content of the four modules were as follows: (i) Module one: vaccine preventable diseases, vaccines, and cold chain (ii) Module two was on ensuring safe injections as well as planning and holding immunization sessions. (iii) Module three was on building community support for immunization and gathering immunization information from the community. (iv) Module four was on communication with mothers about immunization.
Intervention
The training involved a two- day immunization refresher training workshop following the pre-intervention assessment with questionnaire. A combination of different training methods utilized for the training include use of PowerPoint presentation, pictures, demonstrations, group discussions, and video show.
Data analysis
Data entry and analysis were performed with SPSS for windows version 21 (IBM SPS Statistics, IBM Corp, New York). Before analysis, the data were checked and cleaned. Participants socio-demographic characteristics like age, sex, professional background, educational background; years of experience of immunization practice and previous attendance of immunization training were described and summarized as means and standard deviations for continuous variables and as frequencies and percentages for categorical variables. Seventy-three questions were used to assess the participants’ knowledge and self-reported practice. Thirty-six questions were used to assess their knowledge, out of these, twenty-five items had options 1-5 in which only one option was correct, and 11 items had ‘True/False options. The remaining 37 items for assessing their knowledge and self-reported practice were on 7-points Likert scale. The first 7-points Likert scale assessed how important each statement about immunization is to a participant ranging from 6 (Very important) to 0 (Neutral/don’t know). The second 7-points Likert scale assessed how a participant agreed with each statement about immunization practice ranging from 6 (Strongly agree) to 0 (Neutral/don’t know). For the observation checklist, Scores were awarded to each item ranging from 0 (never) to 6 (very frequently) as immunization providers were observed communicating with mothers on immunization and documenting essential immunization information in the children’s cards and clinic records. Summation of scores for each session of observation were then made to add up for each point of assessment. The approximate scores of individuals before and after training were compared using paired t-test. Pre- test versus post-test differences among groups with training intervention and groups without training were tested using the paired t-test. Mean changes in post intervention scores immediately after intervention and at three months and six months post intervention were evaluated using repeated measures ANOVA. To test for the relationship between mean changes in knowledge and self-reported scores and participants’ professional backgrounds, educational levels, previous attendance of immunization training and years of experience at PHC level, one way ANOVA was used. Statistical significance level was set at p <0.05.
Composition of study participants
Overall, 70 willing and eligible immunization providers participated in the study. Thirty-nine participants (55.7%) in the intervention groups participated in a two-day refresher immunization training while the remaining 30 participants (44.3%) from control groups were not trained until after completion of the study One (1.4%) of the 70 participants retired from the service of one of the LGAs before the 6 months post -intervention assessment and was therefore loss to follow-up.
Socio-demographic and professional characteristics of participants in the study
The socio-demographic and professional profile of the training participants revealed that their age ranged from 26 to 57, mean age was 44.4 (SD 7.1) years. They were predominantly female (94.2%), only four (5.8%) were male. Nurses/midwives constituted only 17 (24.6%) of all the 69 participants, the remaining 52 (75.4%) were made up of CHOs and CHEWs. Other characteristics of the participants are presented in Table 1.
Immunization training experiences of PHC immunization providers in the study
Fifty-nine (85.5%) of the participants have had previous immunization training at one time or the other but not less than six months before the training in this study. Only 10 (14.5%) have never had any form of training on immunization. Among those who had been previously trained, the duration of the training ranged from one day to five days with the training organizers being mostly the local, state or federal government and international organizations like WHO and UNICEF.
Baseline mean scores of knowledge and self-reported practice of participants
Table 2 showed that at baseline, the participants group B (intervention) had the highest total mean scores while the participants group C (intervention) had the lowest total mean score.
Effect of the training intervention on the knowledge and self-reported practice of participants in the intervention groups
The group mean scores of the two groups who participated in the training intervention is presented in Figure 1. As displayed in the figure, there was a sharp increase in the mean scores of the participants’ knowledge and self-reported practice immediately after the training in the two groups. Thereafter, there was a drop in the mean scores of the two groups at the three months and six months post-intervention assessment. Table 3 showed the comparison of the mean scores of the participants in intervention groups in the different parameters assessed at baseline, immediate post-training and at 3 and 6 months post- training. The within subject effects in repeated measures ANOVA as presented in table revealed a statistically significant improvement in the participants scores in all the three parameters of questionnaire assessment between time points, general knowledge of immunization and self-reported practice (F= 8.235, P<0.001), gathering immunization information from the community (F=2.919, P< 0.05) and communication with mothers about immunization (F=17.913, P<0.001).
Comparison of knowledge and practice scores between training intervention groups and control groups at baseline, three months and six months post-intervention
Table 4 illustrates the Repeated Measures ANOVA comparison of group mean scores of participants for all the four groups at baseline, three months and six months post-intervention assessments. As revealed in the table, the three months post- intervention mean total knowledge scores of all the four groups (A,B,C and D) were higher than the baseline mean scores but the increase was more evident among groups B and C that had the training intervention.
Factors influencing PHC immunization providers’ knowledge and self-reported practice
Pre-and post- intervention assessments mean knowledge and self-reported practice scores of PHC immunization providers were compared utilizing a paired t-test with respect to their different study group, age, professional categories, years of experience of immunization practice at PHC level and previous attendance of immunization training. There was a significant association found between the participants’ study group and their pre-and post-intervention knowledge and self-reported practice scores. The mean scores of participants in in Group B (intervention) were significantly higher in communication with mothers about immunization immediate post-intervention (P< 0.05), three months post-intervention (P< 0.05) and six months post- intervention (P< 0.05) compared with participants from other three study groups (groups A-control, C-intervention and D-control). In all the study groups, participants’ age was not significantly associated with their mean scores pre-and post- intervention in all the three parameters assessed: general knowledge of immunization and self-reported practice, building community support for immunization and gathering immunization information from the community (P> 0.05). Comparing the participants’ scores with their professional category, the mean knowledge and self-reported practice scores of Nurse/Midwife/Public Health Nurse was significantly higher in three months post-intervention general knowledge of immunization and self-reported practice and gathering immunization information from the community (P< 0.05) compared with other professional categories like Community Health Officers (CHO), Nurse/Midwife, CHEW/CHO and CHEW (Community Health Extension Workers). The participants’ years of experience of immunization practice at PHC level and their mean scores for all the different types of assessment conducted showed no significant association (P>0.05). Also, no significant association was found between the participants’ previous attendance of immunization training (irrespective of the training interval) and their mean scores in the pre-intervention assessment. In general knowledge of immunization and self-reported practice (P>0.05), gathering immunization information from the community, (P>0.05) and communication with mothers about immunization (P>0.05).
Mean scores of observations of participants’ communication practice with mothers on immunization
The mean scores for observation of participants’ communication practice with mothers on immunization across four points of assessment is shown in Table 5. Between groups ANOVA showed no significant difference across the four points of assessment pre-intervention and post-intervention in the two groups with training intervention groups (Group B, P>0.05), (Group C, P> 0.05). Among the two groups without training intervention, group D showed a significant negative difference as there was a drop in the mean scores across the points of assessment (P<0.05).
Socio-demographic and professional characteristics of participants in the study
The findings in this study show that male gender constituted a very small proportion of the participants. Also, less than a quarter of the participants were nurse/midwife, this is an indication of shortage of professional nurses and midwives in the study setting, meanwhile, Nurses/midwives have been recognized as front-line service providers engaged in the efforts to renew Primary Health Care (PHC) and health system strengthening [22]. Recruitment and retention of qualified nurses/midwives is essential for sustainable and effective immunization services. Nurse have a unique role in advocating for immunization adherence, by listening to and addressing parents´ concerns about immunizations, nurses can dispel misconceptions and help change parents´ perceptions about the risks associated with immunizations [23].
Effect of the training intervention on the knowledge and self-reported practice of participants in the study
In this study, the immediate post-training intervention assessment showed an improvement in the knowledge and self-reported practice of the training participants in the two intervention groups. Surprisingly, the evidence of improvement was more with the participants in group C (intervention) who had the lowest mean score at baseline, but immediately after the training intervention there was a leap in their mean score in all the three sections of the assessment. This general improvement in the participants’ performance in the immediate post-intervention assessment can be attributed to the effectiveness of the training. Different teaching methods were utilized for the training, also, a bound copy of the training manual was given to each participant. It can be speculated that the various methods of teaching integrated in the training intervention helped in the initial increase in knowledge of the training participants. Evidence showed that an individual learns through five senses – hearing, sight, touch, smell, taste and combinations of these [24]. During the training intervention in this present study, hearing, such as in the lecture done with PowerPoint presentations accounts for only 13% of learning. However, 75% of learning is through the eyes; thus, the pictures, video clips, and group discussions contributed to the effectiveness of the program. Despite the improvement noticed in the performance of the participants in the two intervention groups in immediate post- training intervention assessment, there was a progressive moderate decline in their mean scores at three months and six months post-intervention. Though there was a decline in the knowledge of the participant, overall, the immunization training intervention significantly raised knowledge scores and self-reported practice scores in both groups and the scores at the end of the six-month period were still higher than pre-intervention scores. However, knowledge decay after training has been reported in previous studies [25,26]. Continuing education as a single intervention is likely to be effective in the short term and can improve the performance of health care providers; however, to sustain effectiveness, additional interventions addressing health systems or community issues are required [27]. The progressive decrease in the knowledge of the participants indicates that it can still further decrease in the succeeding months, this is an indication for frequent training and retraining of immunization providers by the government and immunization policy makers to maintain the standard practice on immunization.
Factors influencing PHC immunization providers’ knowledge and self-reported practice
In this study, immunization providers’ age, years of experience of immunization practice at PHC level and previous attendance of immunization training did not have any significant association with their performance in all the assessments conducted. Only professional category was found to have a significant association with their performance at three months post-intervention assessment. Nurse/Midwife/Public Health Nursing practitioners were better off in their performance than other category of health workers. The is probably because nurse/midwife/public health nursing qualification has a considerable public health academic dimension making nurses to be better equipped to work in the community. This also indicates that nurse/midwife/public health nurses probably understood how vital their position is to maintaining a high standard for immunization services which motivated them to be ready to gain and retain more information from the training intervention than the other healthcare workers. The results of this study have an implication for nurses/midwives who practice at PHC level to seek additional qualification in Public Health so that they can be better equipped for health promotion and disease prevention services at the grass root level where they work. Lack of significant improvement in the participants’ mode of communication with mothers about immunization in the study shows that training can improve knowledge without improvement in the attitude and behaviors of the trainees. Therefore, training intervention focusing on health providers to improve immunization coverage should target more on behavioral and attitudinal changes to achieve the desired effect.
Limitation: this study is not without limitation as immunization providers’ practice in this study (apart from communication practice) was measured based on self-report. Hence the degree of accuracy may not be fully guaranteed.
Recommendations for future research: for future research, it is important to evaluate the effect of immunization training intervention on actual practice of participants as well as routine immunization uptake.
Implications of the study for routine immunization services strengthening in Primary Health Care
Training of PHC services’ providers on immunization has the potential of building their capacity for efficient service delivery, mobilizing people to generate demand for immunization and monitoring program performance. However, for the impact of training to be sustained, government and immunization policy-makers should organize frequent training and retraining of immunization providers as stated in the national immunization policy to maintain the standard practice. Also, monitoring and supportive supervision system should be functional at the ward and health facility levels to enhance the quality of immunization services provided in the context of task-shifting initiatives in PHC.
This study showed that a training intervention on immunization for PHC providers improved their knowledge and self-reported practice but did not improve their actual practice of communication with mothers on immunization. There is a need for immunization policy makers to pay particular attention to monitoring, evaluating and supportive supervision of immunization practice of health providers in primary health care.
What is known about this topic
- Training is an important aspect of health providers’ knowledge and practice;
- Training interventions improve immunization provider’s performance.
What this study adds
- Training intervention can increase the knowledge and self-reported practice of immunization providers without improving their behavior, attitude and actual practice.
The authors declare no competing interest.
Brown VB, Oluwatosin OA and Ogundeji MO designed this study, all the authors participated in the data collection, Brown VB and Oluwatosin OA analyzed and interpreted the data. All authors have read and agreed to the final version of this manuscript.
The African Population and Health Research Centre (APHRC) in partnership with the International Development Research Centre (IDRC) are duly acknowledged for funding and technical support through the African Doctoral Dissertation Research Fellowship (ADDRF). Also Dr. Adebowale Adeyemo of the National Institutes of Health, Bestheda, MD, USA is duly acknowledged for technical assistance.
Table 1: socio-demographic and professional characteristics of participants across study groups
Table 2: baseline mean scores of knowledge and self-reported practice of participants by study group
Table 3: comparison of mean scores to detect intervention effect among participants in training intervention groups at baseline, immediate post-training intervention and at 3 and 6 months post- training intervention
Table 4: repeated Measures ANOVA of knowledge and practice scores between groups with training and groups without training intervention at baseline, three months and six months post-intervention
Table 5: mean scores for observation of participants’ communication with mothers on immunization across study groups
Figure 1: comparison of mean total knowledge and self-reported practice scores of training intervention group B and group C at baseline, 3 months and 6 months post-intervention assessment
- World Health Organization (WHO). State of the World's Vaccines and Immunization. 3rd ed. Geneva: WHO. 2009. Google Scholar
- Stockwell MS, Irigoyen M, Martinez RA, Findley S. How parents' negative experiences at immunization visits affect child immunization status in a community in New York City. Public Health Rep. 2011; 126 Suppl 2: 24-32. PubMed | Google Scholar
- Al-lela OQ, Bahari MB, Salih MR, Al-Abbassi MG, Elkalmi RM, Jamshed SQ. Factors underlying inadequate parents' awareness regarding pediatrics immunization: findings of cross-sectional study in Mosul- Iraq. BMC Pediatr. 2014; 14: 29. PubMed | Google Scholar
- Anastasi D, Di Giuseppe G, Marinelli P, Angelillo IF. Pediatricians knowledge, attitudes, and practices regarding immunizations for infants in Italy. BMC Public Health. 2009; 9: 463. PubMed | Google Scholar
- Pelly PL, Pierrynowski MacDougall DM, Halperin BA, Strang RA, Bowles SK, Baxendale DM, McNeil SA. An assessment of immunization education in Canadian health professional program. BMC Med Educ. 2010; 10: 86. PubMed | Google Scholar
- Uskun E, Uskun SB, Uysalgenc M, Yagiz M. Effectiveness of a training intervention on immunization to increase knowledge of primary healthcare workers and vaccination coverage rates. Public Health. 2008 Sep; 122(9): 949-58. PubMed | Google Scholar
- Moores P, Allan P. Affecting change through continuing education: improving vaccine administration technique. J Contin Educ Nurs. 2012; 43: 401-402. PubMed | Google Scholar
- Berenson AB, Rahman M, Hirth JM, Rupp RE, Sarpong KO. A brief educational intervention increases providers' human papillomavirus vaccine knowledge. Hum Vaccin Immunother. 2015; 11(6): 1331-6. PubMed | Google Scholar
- Perkins RB, Zisblatt L, Legler A, Trucks E, Hanchate A, Gorin SS. Effectiveness of a provider-focused intervention to improve HPV vaccination rates in boys and girls. Vaccine. 2015; 33: 1223-9. PubMed | Google Scholar
- National Population Commission (NPC) [Nigeria] and ICF International. Nigeria Demographic and Health Survey 2013. Abuja, Nigeria, and Rockville, Maryland, USA. 2014. PubMed | Google Scholar
- Leask J, Willaby HW, Kaufman J. The big picture in addressing vaccine hesitancy. Hum Vaccin Immunother. 2014; 10(9): 2600-2. PubMed | Google Scholar
- Desilets LD, Dickerson PS. Continuing nursing education: enhancing professional development. J Contin Educ Nurs. 2010 Mar; 41(3): 100-1. PubMed | Google Scholar
- Stokes-Prindle C, Wonodi C, Aina M et al. Landscape Analysis of Routine Immunization in Nigeria: identifying Barriers and Prioritizing Interventions. Baltimore, Maryland, United States: International Vaccine Access Center, Johns Hopkins Bloomberg School of Public Health. 2012. Google Scholar
- National Primary Health Care Development Agency (NPHCDA): Minimum Standards for Primary Health Care in Nigeria. Abuja; Nigeria. Abuja. NPHCDA; 2012. Google Scholar
- Dovlo D. Using mid-level cadres as substitutes for internationally mobile health professionals in Africa: a desk review. Hum Resour Health. 2004 Jun 18; 2(1): 7. PubMed | Google Scholar
- Centre for Disease Control and Prevention (CDC) and WHO. Literature Review: Reasons children are not vaccinated in low and middle income countries Country Facts Sheets & Global Matrix. Geneva: WHO. 2009; pp 55-57. Google Scholar
- Federal Ministry of Health. National Immunization Policy. National Primary Health Care Development Agency. NPHCDA. 2009; pp13. Google Scholar
- Pocock SJ. Clinical Trials: a Practical Approach. Chichester: John Wiley & Sons. 1983. Google Scholar
- Julious SA. Sample sizes for clinical trials with normal data. Stat Med. 2004 Jun 30; 23(12): 1921-86. PubMed | Google Scholar
- World Health Organization (WHO). Identifying and Overcoming Obstacles to Increased Immunization Coverage. Global Program for Vaccines and Immunization Expanded Program on Immunization. Geneva: WHO. 1997. Google Scholar
- World Health Organization (WHO). Immunization in Practice: A Practical Resource Guide for Health Workers. Geneva, WHO. 2004. Google Scholar
- World Health Organization (WHO) Resolution WHA 62.12. Primary Health Care, Including Health Systems and Strengthening. In: Sixty-Second World Health Assembly. Geneva: WHO. 2009. PubMed | Google Scholar
- Holland WG. Nurses as primary advocates for immunization adherence. MCN Am J Matern Child Nurs. 2014; 39(6): 351-6. PubMed | Google Scholar
- Mattiske C. Training for Result: Maximize the Impact of Training through Review. Sidney, Australia. The Performance Company Pty. 2009; pp54-57. Google Scholar
- Anderson GS, Gaetz M, Masse J. First aid skill retention of first responders within the workplace. Scand J Trauma Resusc Emerg Med. 2011; 19: 11. PubMed | Google Scholar
- Amaral F, Almeida Troncon LE. Retention of knowledge and clinical skills by medical students: a prospective, longitudinal, one-year study using basic pediatric cardiology as a model. The Open Medical Education Journal. 2013; 6: 48-54. PubMed | Google Scholar
- Dieleman M, Gerretsen B, van der Wilt GJ. Human resource management interventions to improve health workers' performance in low and middle income countries: a realist review. Health Res Policy Syst. 2009; 7: 7. PubMed | Google Scholar












