Primary multiple osseous leiomyosarcomas of the spine metastasizing to the skull
Oudrhiri Mohammed Yassaad, Raouzi Nabil, El KacemiInas, Allaoui Mohammed, Arkha Yasser, El Ouahabi Abdessamad
Corresponding author: Oudrhiri Mohammed Yassaad, Neurosurgery Department, H�pital des Sp�cialit�s, UHC Ibn Sina, Rabat, Morocco 
Received: 28 Oct 2015 - Accepted: 26 Jul 2016 - Published: 30 Aug 2016
Domain: Clinical medicine
Keywords: Leiomyosarcoma, spine, primary, spinal cord compression, immunohistochemistry
©Oudrhiri Mohammed Yassaad et al. Pan African Medical Journal (ISSN: 1937-8688). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Oudrhiri Mohammed Yassaad et al. Primary multiple osseous leiomyosarcomas of the spine metastasizing to the skull. Pan African Medical Journal. 2016;24:334. [doi: 10.11604/pamj.2016.24.334.8297]
Available online at: https://www.panafrican-med-journal.com//content/article/24/334/full
Primary multiple osseous leiomyosarcomas of the spine metastasizing to the skull
Oudrhiri Mohammed Yassaad1,&, Raouzi Nabil1, El KacemiInas1, Allaoui Mohammed2, Arkha Yasser1, El Ouahabi Abdessamad1
1Neurosurgery Department, H�pital des Sp�cialit�s, UHC Ibn Sina, Rabat, Morocco, 2Neuropathology Department, H�pital des Sp�cialit�s, UHC Ibn Sina, Rabat, Morocco
&Corresponding author
Oudrhiri Mohammed Yassaad, Neurosurgery Department, H�pital des Sp�cialit�s, UHC Ibn Sina, Rabat, Morocco
Primary osseous leiomyosarcoma of the spine is a very unusual condition, with only few cases being reported in the literature.In fact, this type of tumors arises from the smooth muscle cells and occurs usually in the uterus and the gastrointestinal tracts. If the spine should be involved, it occurs generally as a metastatic location. Location to the spine as a primary site is exceedingly rare. We present the case of a 37 years old female patient, with multiple spine levels involvement - to vertebral body and to posterior aspects of vertebral, causing spinal cord compression syndrome. A secondary location to the skull was diagnosed one month later. Through a literature review, we analyze various aspects in the diagnosis and management of this rare entity.
Primary osseous leiomyosarcoma of the spine is a very rare condition. This type of tumors arises from the smooth muscle cells and occurs usually in the uterus and the gastrointestinal tracts. The spine may then be involved as a metastatic location [1]. Primary location to bone is quite unusual, and has been mainly reported on long bones of the limbs [2]. Location to the spine as a primary site is exceedingly rare.
A 37 years old female was admitted to our department for a 2 months history of lombosacral radiculopathy - especially to the right leg - and low back pain, which was treated with NSAID (non steroid anti-inflammatory drug) with only partial remission. Two weeks before admission, the patient experienced rapidly progressive paraparesis with urinary dysfunction. Her past medical history was unremarkable. On admission, the patient was in moderate general condition (Karnovsky 50%) with a predominant right paraparesis (3/5), a sensory level below the umbilicus and genitor-urinary sphincter dysfunction. Reflexes were exaggerated on lower limbs. Local examination of the spine could find tenderness in the right paravertebral area on T12-L1 level, related to a subcutaneous fixed mass. Computed tomography and magnetic resonance imaging of the spine were performed. Findings were compatible with multiple metastases, and involved: (Figure 1). The posterior part of the vertebral body of T5, with posterior wall rupture (Figure 1 b); the posterior elements of T12 and L1 vertebras, with a tissular mass causing bone lysis, severe cord compression and extending to the paravertebral region; the vertebral body was intact (Figure 1 a, b, c, d, and e). Vertebral body of S1, withlysis, right spinal canal invasion and extension to the pre-vertebral area (Figure 1 f) These lesions were iso- to hypo-intense to bone on T1 weighted images (Figure 1 a, b), and heterogeneous on T2 weighted images with multiple hyperintense foci (Figure 1 c). Contrast enhancement was intense and also heterogeneous, and was extending vertically along the epidural space of the medial lesion (Figure 1 d). On CT scan, bone lysis was observed. Computed tomography of brain, cervical, thoracic, abdominal and pelvian regions, and also systemic investigations were all negative for a primary tumoral lesion. The patient was proposed for a posterior decompression on T12-L1 level with instrumented fixation -as symptoms were mainly related to it- and also a sacral decompression. In the dorsolumbar area, the tumor was immediately found under the subcutaneous tissue, invading the paravertebral muscles: A multi-lobulated firm mass, with a white-reddish appearance, mainly avascular. The tumor was not encapsulated but could easily be differentiated and separated from thesurrounding tissue. The bone lysis was evident, and the spinal cord compression severe. The dura matter was not infiltrated (Figure 2). Dural decompression was completed and T11-L2 screw fixation was performed - given the pedicle lysis on CT-scans - after gross total removal was achieved.
�
Taking advantage of the patient�s position, and given the history of lombosacral radiculopathy, an S1 right hemilaminectomy with curettage of the sacral body and radicular decompression were also performed.Operative findings were compatible with the upper level. Histology specimens were analyzed for both localizations, with an identical result: a malignant spindle cell proliferation with large necrotic areas. Tumor cells were arranged into short fascicles and interlacing bundles (Figure 3). The nuclei were hyperchromatic and occasionally highly pleiomorphic. Mitotic figures were recognized in about 15 per 10 high power fields. Large necrotic areas were observed (about 50% of the tumor surface). Immunohistochemical staining was positive for smooth muscle actin, desmin and H-caldesmon, and negative for S100 protein, and CD34 (Figure 4). Focal reactivity was observed with EMA. Thus, the diagnosis of a leiomyosarcoma grade 3 of the FNCLCC was established. In the postoperative period, the patient started improving her motor score, and gaining control on her urinary function. She was discharged on both rehabilitation unit and oncology unit for adjuvant therapy. One month after discharge, the patient presented for persistent headaches, with no focal signs. Locally, we could find tenderness on the right frontal area of the skull convexity. CT scan was performed, showing a small lytic frontal bone lesion extending to the subcutaneous tissue withoutdural extension (Figure 5). A small craniectomy around was performed, and the histopathology came back with no surprise. At one year follow up, the adjuvant therapy failed to obtain tumor control. The thoracic and abdominopelvian CT scan showed both local and systemic progression. Although her motor function improved continuosly to become self dependant, her general condition was worsening. She was then assessed for palliative treatment. The patient died two years after her initial management.
Leiomyosarcoma is a malignant neoplasm originating from the smooth muscle cells. It occurs predominantly in the retroperitoneum, the intrabdominal space and the subcutaneous tissue of the extremities [3]. Primary location to bone was mainly described for long bones such as femur and tibia [2], and account for 0.1% to 0.64% of all primary bone tumors [3]. The osseous leiomyosarcoma is thought to originate from the smooth cells in the vasculature. Other hypothesis includes a multipotential mesenchymal cell or an intermediate cell capable of smooth muscle cell differentiation [2]. This osseous origin can only be assessed after careful body screening to rule out a usual primary location, as osseous metastases may be the initial manifestation of primary uterine leiomyosarcoma [4].
�
Literature review�
We performed a careful analysis of the existing literature through a Pubmed research of Medline�s database (using the keywords: primary, leiomyosarcoma, spine, and skull). To date, 17 cases of primary spine locations have been reported (Table 1). These locations included both the vertebral body [1-3,5-12] and the posterior aspects of the vertebra [13-15]. Potsi, in his recent paper [1], took only into account the vertebral body involvement and found 14 reported observations (including his work). We think that the development into the posterior elements of the vertebra and the paravertebral area may be considered as well. In fact, our patient presented both aspects: a vertebral body lesion and a posterior vertebral/paravertebral lesion. The skull manifestation described here was considered as metastatic from the spine. No publication described primary multiple spine level involvement as was the case with our patient. Central nervous system involvement was described mainly as intracranial tumors [10,16]. This tumor affects adult patients, with ages ranging from 23 years to 75 years. No case has yet been described into the pediatric population. Unlike other bone locations where there is no sex preponderance[8], primary spinal locations occur more frequently in women (13 out of 18) as for leiomyosarcoma [11]. Most patients presented with pain and signs of spinal cord compression and progressive myelopathy. Leiomyosarcoma of the spine presents as an ill-defined lytic mass, affecting both the vertebral body and/or the posterior aspects, invading the spinal canal. A prevertebral or a paravertebral development is usually seen. A compression fracture may also be seen[11].The spine is uniformly affected. Although there is no specific radiologic criterion, this tumor appears frequently iso- to hyperintense to bone on T1 weighted images; a heterogeneous hyperintensity is seen on T2 weighted images with irregular enhancement [1]. Histopathology should differentiate leiomysarcoma from other spindle cell tumors. In this concern, immunohistochemical study is very useful: a positive reactivity with smooth muscle actin, vimentin and caldesmon, but negative reactivity for S100 protein and CD34 [3,11]. Reactivity for Desmin is irregular [1,9,12,15]. Some special histopathological aspects as anepithelioid differentiation were described [15].�
Although no consensus about treatment is available, management of these tumors, given their malignancy, should include total radical excision whenever possible [1]. Adjuvant therapy is mandatory and may include radiotherapy alone or an association to chemotherapy. In our case, we first considered the metastatic origin of the tumors given the multiple locations. When a primary lesion has been ruled out after careful repeated systemic screenings, the treatment modality consisted on a surgical treatment of the symptomatic level through a posterior approach, radical excision of the tumor and posterior fixation. Surgical excision of all lesions was not considered given the initial spreading of the tumor.
The diagnosis of a primary spine location of leiomyosarcoma is an unusual condition. It should only be made after careful screening for a primitive tumor, and on immunohistochemical basis. Surgical treatment, as for other spine malignancies, should be as radical as possible. We report herein another unusual aspect of this tumor.
The authors declare no competing interest.
The authors have read the final version of this manuscript.
Table 1: summary of published cases of primary spinal leiomyosarcomas
Figure 1: MRI images of the spine in sagittal T1 (a&b), sagital T2 (c) and post contrast sagital (d) and axial (e). The tumor is hypointense to bone on T1 weighted images (a&b), slightly hyperintense and heterogeneous on T2 weighted images (c), with intense, irregular contrast enhancement (d&e). Note the vertebral body involvement in T5 lesion (superior arrows in a, b & c). Note the severe spinal cord compression (middle arrows in a, b, c & e). Note the contrast enhancement along the dura that extends upward and downward (upper arrow in d). Image �f� is an axial CT scan slide showing the sacral lesion with the bone lysis (arrow).
Figure 2: operative findings. The tumor caused extended bone lysis (arrows in a); the dura was not invaded. The tumor was white-reddish and multilobulated (b)
Figure 3: photomicrograph of the biopsy specimen showing interlacing fascicles of spindle-shaped cells with elongated or blunt-ended nuclei and eosinophilic cytoplasm. Hyperchromatic or pleomorphic nuclei and mitoses are occasionally observed. (Haematoxylin and eosin; Original magnification, x100)
Figure 4: immunohistochemistry staining: the tumor cells are positive for H-Caldesmon (a), Alpha-Smooth Muscle Actin (b), Desmin (c), negative for S100 (d), (Original magnification, x100)
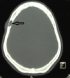
Figure 5: axial CT scan slide, showing the metastatic frontal bone lytic lesion (arrow)
- Potsi M, Stavrinou P, Patsinakidis N, Hatzibougias D, Foroglou N, Karayanopoulou G, et al. Primary osseous leiomyosarcoma of the spine: a rare entity--case report and review of the literature. J Neurol Surg Part A Cent Eur Neurosurg. 2012;73(4):238-242. PubMed | Google Scholar
- Antonescu CR, Erlandson RA, Huvos AG. Primary leiomyosarcoma of bone: a clinicopathologic, immunohistochemical, and ultrastructural study of 33 patients and a literature review. Am J Surg Pathol. 1997;21(11):1281-1294. PubMed | Google Scholar
- Nishida J, Kato S, Shiraishi H, Ehara S, Sato T, Okada KM, et al. Leiomyosarcoma of the Lumbar Spine: Case Report. Spine. 2002; 27: 42-46. PubMed | Google Scholar
- Fornasier VL, Paley D. Leiomyosarcoma in bone: primary or secondary? A case report and review of the literature. Skeletal Radiol. 1983;10(3):147-153. PubMed | Google Scholar
- Berlin �, Angervall L, Kindblom L-G, Berlin IC, Stener B. Primary leiomyosarcoma of bone. Skeletal Radiol. 1987;16(5):364-376. PubMed | Google Scholar
- Ganau S, Tom�s X, Mallofr� C, Macho JM, Pom�s J, Combalia A. Leiomyosarcoma of sacrum: imaging and histopathologic findings. Eur Radiol. 2002; 12 Suppl 3:35-39. PubMed | Google Scholar
- Krepler P, Windhager R, Bretschneider W, Toma CD, Kotz R. Total vertebrectomy for primary malignant tumours of the spine. J Bone Joint Surg Br. 2002;84-B(5):712-715. PubMed | Google Scholar
- Lo TH, Rooij WJJ van, Teepen JLJM, Verhagen ITHJ. Primary leiomyosarcoma of the spine. Neuroradiology. 1995;37(6):465-467. PubMed | Google Scholar
- Ochiai H, Yamakawa Y, Fukushima T, Yamada H, Hayashi T. Primary leiomyosarcoma of the cervical spine causing spontaneous compression fracture: Report of an autospy case. Neuropathology. 2000;20(1):60-4. PubMed | Google Scholar
- Ritter AM, Amaker BH, Graham RS, Broaddus WC, Ward JD. Central nervous system leiomyosarcoma in patients with acquired immunodeficiency syndrome: Report of two cases. J Neurosurg. 2000;92(4):688-692. PubMed | Google Scholar
- Sasaguri T, Tanimoto A, Kimura S, Kohno Y, Hirasawa M, Matsuki Y, et al. Primary leiomyosarcoma of the vertebra: Case report and review of the literature. Pathol Int. 2004;54(1):73-6. PubMed | Google Scholar
- Sucu HK, Bezircioglu H, Rezanko T. Partial Spondylectomy for Primary Leiomyosarcoma of C2 Vertebra.Spine. 2011; 36(21): E1422-E1426. PubMed | Google Scholar
- Aksoy DY, Altundag MK, Durusu M, Abali H, Onder S, Turker A, et al. Thoracic paravertebral leiomyosarcoma: rare but it does occur. Spine. 2002;27(12):E301-303. PubMed | Google Scholar
- Lehman NL, Jacobs CD, Holsten PA, Jaikumar S, Lehman TD, Gibbs IC, et al. Primary paraspinal leiomyosarcoma invading the cervical spinal canal successfully treated with surgery, radiotherapy, and chemotherapy: Case report. J Neurosurg Spine. 2007;6(5): 441-446. PubMed | Google Scholar
- Marshman LAG, Pollock JR, King A, Chawda SJ. Primary Extradural Epithelioid Leiomyosarcoma of the Cervical Spine: Case Report and Literature Review. Neurosurg. 2005;57: 372-375. PubMed | Google Scholar
- Zhang H, Dong L, Huang Y, Zhang B, Ma H, Zhou Y, et al. Primary intracranial leiomyosarcoma: review of the literature and presentation of a case. Onkologie. 2012;35(10):609-6. PubMed | Google Scholar
Search
This article authors
On Pubmed
On Google Scholar
Citation [Download]
Navigate this article
Similar articles in
Key words
Tables and figures
 Figure 1: MRI images of the spine in sagittal T1 (a&b), sagital T2 (c) and post contrast sagital (d) and axial (e). The tumor is hypointense to bone on T1 weighted images (a&b), slightly hyperintense and heterogeneous on T2 weighted images (c), with intense, irregular contrast enhancement (d&e). Note the vertebral body involvement in T5 lesion (superior arrows in a, b & c). Note the severe spinal cord compression (middle arrows in a, b, c & e). Note the contrast enhancement along the dura that extends upward and downward (upper arrow in d). Image �f� is an axial CT scan slide showing the sacral lesion with the bone lysis (arrow).
Figure 1: MRI images of the spine in sagittal T1 (a&b), sagital T2 (c) and post contrast sagital (d) and axial (e). The tumor is hypointense to bone on T1 weighted images (a&b), slightly hyperintense and heterogeneous on T2 weighted images (c), with intense, irregular contrast enhancement (d&e). Note the vertebral body involvement in T5 lesion (superior arrows in a, b & c). Note the severe spinal cord compression (middle arrows in a, b, c & e). Note the contrast enhancement along the dura that extends upward and downward (upper arrow in d). Image �f� is an axial CT scan slide showing the sacral lesion with the bone lysis (arrow).