Upper extremity deep vein thrombosis after elbow trauma: a case report of a rare occupational accident
Maher Maoua, Wided Boughattas, Aicha Brahem, Olfa El Maalel, Houda Kalboussi, Sana El Guedri, Wael Majdoub, Souhail Chatti, Faten Debbabi, Néjib Mrizak
Corresponding author: Maoua Maher, Department of Occupational Medicine, Faculty of Medicine of Sousse, Sousse, Tunisia 
Received: 13 Feb 2016 - Accepted: 04 Apr 2016 - Published: 28 Apr 2016
Domain: Clinical medicine
Keywords: Deep vein thrombosis, Upper extrimity, occupational accident
©Maher Maoua et al. Pan African Medical Journal (ISSN: 1937-8688). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Maher Maoua et al. Upper extremity deep vein thrombosis after elbow trauma: a case report of a rare occupational accident. Pan African Medical Journal. 2016;23:251. [doi: 10.11604/pamj.2016.23.251.9107]
Available online at: https://www.panafrican-med-journal.com//content/article/23/251/full
Original article 
Upper extremity deep vein thrombosis after elbow trauma: a case report of a rare occupational accident
Upper extremity deep vein thrombosis after elbow trauma: a case report of a rare occupational accident
Maher Maoua1,&, Wided Boughattas1, Aicha Brahem1, Olfa El Maalel1, Houda Kalboussi1, Sana El Guedri1, Wael Majdoub2, Souhail Chatti1, Faten Debbabi1, Néjib Mrizak1,2,3
1Department of Occupational Medicine, Faculty of Medicine of Sousse, Sousse, Tunisia, 2Department of Forensic Medicine, Faculty of Medicine of Sousse, Sousse, Tunisia, 3Department of Occupational Medicine, Teaching Hospital Farhat Hached, Sousse, Tunisia
&Corresponding author
Maoua Maher, Department of Occupational Medicine, Faculty of Medicine of Sousse, Sousse, Tunisia
Upper extremity deep vein thrombosis (UEDVT) is rare, especially after benign trauma. We report the case of a 31-year-old male nurse with UEDVT after elbow trauma with no fracture. This occupational accident caused thrombosis of basilica vein extended to humeral and axillary veins, collateral circulation in the arm and the right cervical and axillary regions. Thrombophilic tests and assessment of malignant tumor were negative. Treatment by low molecular weight heparin (LMWH) then by vitamin K antagonists was conducted and evaluation by Doppler ultrasonography realized 18 months after trauma showed recanalization of basilica and humeral veins and thrombosis of axillary and subclavian veins. Management of occupational activity was prescribed including eviction of heavy loads handling and repetitive gestures of upper limbs.
Upper deep vein thrombosis (UEDVT), which was considered as a rare benign phenomenon in the past, has become more frequent since the 1970s because of the use of central venous catheters (CVCs) transvenous pacers [1]. Approximately 4-10% of all cases of venous thrombosis involve the subclavian, axillary or brachial veins [2-4]. UEDVT is classified as primary or secondary on the basis of pathogenesis [5]. Trauma is a rare cause of secondary UEDVT. Few cases of traumatic UEDVT were reported but elbow trauma seems to be rarely involved in this reports.
A 31-year-old male nurse, with no medical history of any past illness, non-smoker, consulted our department of occupational medicine with symptoms of pain, elbow and shoulder discomfort and arm edema. Patient described the occurrence of moderate-intensity trauma of his right elbow during his night shift. The patient’s elbow was accidentally hurt by a door handle. Immediate pain and swelling of the right elbow motivated the patient to consult. Initial Doppler ultrasound showed a dilatation of the basilica vein with no signs of thrombosis. Analgesic treatment was prescribed but had no effect on symptoms.
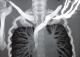
Fifteen days after the trauma, medical re-examination revealed mild cyanosis of the upper right extremity, arm and hand edema and supraclavicular fullness. CT angiography was immediately performed and showed thrombosis of basilica vein extended to humeral and axillary veins, collateral circulation in the arm and the right cervical and axillary regions (Figure 1). This exam revealed the absence of thrombosis of superior vena cava or intra-thoracic tumor (Figure 2). Antithrombin III, and protein C and S levels were normal. Factor V Leiden mutation was absent.
Treatment was based on anticoagulation initially by low molecular weight heparin (LMWH) then by vitamin K antagonists. Evaluation by Doppler ultrasonography realized 18 months after trauma showed recanalization of basilica and humeral veins and thrombosis of axillary and subclavian veins. Declaration of occupational accident was performed since the first reporting of the trauma. Management of occupational activity was prescribed including eviction of heavy loads handling and repetitive gestures of upper limbs.
Incidence of UEDVT is about 3 per 100.000 in the general population [6]. This incidence is much less than that of the lower extremity because of fewer and smaller valves in the veins of upper extremity, less hydrostatic pressure in the arms [6] and increased fibrinolytic activity in the endothelium of upper arm as compared to the lower arm [7-8].
Common risk factors for UEDVT are cancer, CVCs, and thrombophilia. Cancer is diagnosed in 63% of patients with UEDVT [9]. Coon and willis classified UEDVT into two divisions: traumatic (including internal and external trauma) and spontaneous [10]. Few reports of post-traumatic UEDVT included bone fractures. Concerned bones were mainly humerus [11] and clavicule [12]. Bibiche Y. and Kanjaa N. reported a case of traumatic subclavian vein thrombosis without clavicular fracture [13]. Swelling of the upper extremity is the most frequent sign of UEDVT [14]. However, most patients with UEDVT are asymptomatic and most of these cases are CVC-associated [15]. Other symptoms include pain, functional impairment and paresthesias, vague shoulder or neck discomfort with edema and collateral veins [16].
Physical examination may reveal cyanosis of the arm, supraclavicular fullness and visible subcutaneous veins over the evolved shoulder and chest wall, or elevated jugular venous distension [17].
Clinical evaluation remains poorly sensitive and specific and only 50% of objective investigations confirmed thrombosis in patients with symptoms of UEDVT [16]. Objective tests include venography, ultrasound, CT angiography, magnetic resonance angiography, radionuclide venography and D-dimer [14]. Ultrasound and CT angiography are frequently performed for their convenience and accessibility.
Possible complication are pulmonary embolus (PE) or recurrent PE, recurrent deep vein thrombosis (DVT) and SVC syndrome. Post thrombotic syndrome may be observed as sequel [14]. Mortality rates are variable and depend on underlying risk factors for thrombosis [14]. The 3-month mortality varies between 3.5% (non-malignancy-associated UEDVT) and 22% in case of associated malignancy.
Treatment options for UEDVT are conservative management (heat, rest and arm elevation), anticoagulation, thrombolysis, thrombectomy and surgical decompression [14].
Decrease of venous return causing stasis and thrombosis may be an explanation of our patient’s UEDVT after his elbow trauma. Traumatic vascular damage can’t be excluded and may participate in the genesis of the thrombus. Other etiologies were excluded by negative thrombophilic tests and normal radiological assessment. Patients with Paget-Shroetter Syndrome develop spontaneous UEDVT after strenuous activity which was not the case of our patient.
Post-traumatic UEDVT is a rare condition and may cause dramatic complications and sequelae even if trauma seems benign. Early management and close monitoring are required. Occupational impairment in our case was consequent and professional redeployment is envisaged.
The authors declare no competing interests.
Corresponding author Maoua Maher contributed in patient’s follow up and redaction of the scientific paper. All listed authors contributed in medico-legal management of the case and approved the final manuscript.
Figure 1: thrombosis of basilica vein extended to humeral and axillary veins, collateral circulation in the arm
Figure 2: thoracic CT angiography
- Mustafa S, Stein P, Patel K et al. Upper extremity deep venous thrombosis. Chest. 2003;123(6): 1953-6. PubMed | Google Scholar
- Joffe HV, Kucher N, Tapson VF, Goldhaber SZ. Upper-extremity deep vein thrombosis: a prospective registry of 592 patients. Circulation. 2004;110(12):1605-1611. PubMed | Google Scholar
- Bernardi E, Pesavento R, Prandoni P. Upper extremity deep venous thrombosis. Semin Thromb Hemost. 2006; 32(7):729-736. PubMed | Google Scholar
- Spencer FA, Emery C, Lessard D, Goldberg RJ, for the Worcester Venous Thromboembolism Study. Upper extremity deep vein thrombosis: a community-based perspective. Am J Med. 2007;120(8):678-684. PubMed | Google Scholar
- Joffe HV, Goldhaber SZ. Upper-Extremity Deep Vein Thrombosis. Circulation .2002;106(14):1874-80. PubMed | Google Scholar
- Saseedharan S, Bhargava S. Upper extremity deep vein thrombosis. Int J Crit Illn Inj Sci. 2012;2(1):21-6. PubMed | Google Scholar
- Pandolfi M, Robertson B, Isacson S, Nilsson IM. Fibrinolyticactivity of human veins in arms and legs. Thromb Diath Haemorrh. 1968;20(1):247-56. PubMed | Google Scholar
- Robertson BR, Pandolfi M, Nilsson IM. Response of local fibrinolytic activity to venous occlusion of arms and legs in healthy volunteers. Acta Chir Scand. 1972;138(5):437-40. PubMed | Google Scholar
- Lindblad B, Tengborn L, Bergqvist D. Deep vein thrombosis of the axillary-subclavian veins: epidemiologic data, effects of different types of treatment and late sequelae. Eur J VascSurg. 1988;2(3):161-5. PubMed | Google Scholar
- Coon WW, Willis PW 3rd. Thrombosis of axillary and subclavian veins. Arch Surg. 1967;94(5):657-63. PubMed | Google Scholar
- Chuter Graham SJ, Weir David J. Upper extrimity deep vein thrombosis following a humeral fracture: case report and literature review. Injury. 2005;36 (7):249-52. PubMed | Google Scholar
- Chuter Graham SJ, Weir David J. NandanAdla, Ali A, Shahane SA. Upper extremity deep vein thrombosis following a clavicular fracture. Euro J Orthop Surg. Traumatol. 2004;14(3):177-9. PubMed | Google Scholar
- Bibiche Y, Kanjaa N. Post traumatic thrombosis of the subclavian vein without right clavicle fracture: report of a case. Pan Afr Med J. 2015;20:256. PubMed | Google Scholar
- Marshall PS, Cain H. Upper Extremity Deep Vein Thrombosis. Clin Chest Med. 2010;31(4):783-97. PubMed | Google Scholar
- Chastre J, Cornud F, Bouchama A, Viau F, Benacerraf R, Gibert C. Thrombosis as a complication of pulmonary-artery catheterization via the internal jugular vein: prospective evaluation by phlebography. N Engl J Med. 1982;306(5):278-81. PubMed | Google Scholar
- Prandoni P, Polistena P, Bernardi E, Cogo A, Casara D, Verlato F et al. Upper-extremity deep vein thrombosis Risk factors, diagnosis, and complications. Arch Inter Med. 1997;157(1):57-62. PubMed | Google Scholar
- Spiezia L, Simioni P. Upper extremity deep vein thrombosis. Intern Emerg Med. 2010; 5(2):103-9. PubMed | Google Scholar