Management dilemma of hepatocellular carcinoma in pregnancy: a case report
Yaw Asante Awuku, Emmanuella Amoako, Dominic Oduro-Donkor, Joseph Adu
Corresponding author: Yaw Asante Awuku, Department of Medicine and Therapeutics, University of Cape Coast, Cape Coast, Ghana 
Received: 31 Jan 2016 - Accepted: 14 Mar 2016 - Published: 27 Apr 2016
Domain: Maternal and child health
Keywords: Pregnancy, hepatocellular carcinoma, chronic hepatitis B infection
©Yaw Asante Awuku et al. Pan African Medical Journal (ISSN: 1937-8688). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Yaw Asante Awuku et al. Management dilemma of hepatocellular carcinoma in pregnancy: a case report. Pan African Medical Journal. 2016;23:248. [doi: 10.11604/pamj.2016.23.248.8987]
Available online at: https://www.panafrican-med-journal.com//content/article/23/248/full
Management dilemma of hepatocellular carcinoma in pregnancy: a case report
Yaw Asante Awuku1,&, Emmanuella Amoako1, Dominic Oduro-Donkor1, Joseph Adu2
1Department of Medicine and Therapeutics, University of Cape Coast, Cape Coast, Ghana, 2Department of Obstetrics and Gynaecology, University of Cap Coast, Cape Coast, Ghana
&Corresponding author
Yaw Asante Awuku, Department of Medicine and Therapeutics, University of Cape Coast, Cape Coast, Ghana
Hepatocellular carcinoma is rarely associated with pregnancy and when it does there is poor prognosis for both the mother and the baby.There is paucity of evidence for best practice in hepatocellular carcinoma in pregnancy especially in the background of cirrhosis and decompensation. We present a 36 year old gravida 5 para 4 at 27 weeks gestation with hepatocellular carcinoma and main complaint of abdominal pain. She had chronic hepatitis B infection with hepatocellular carcinoma on a cirrhotic background. There were both clinical and laboratory features suggestive of liver decompensation. The pregnancy outcome was a fresh stillbirth with mother alive. This case report highlights the management dilemma of hepatocellular carcinoma in pregnancy on the background of decompensated liver cirrhosis and chronic hepatitis B infection.
Hepatocellular cancer(HCC) is the commonest cause of all primary liver cell cancers worldwide [1]. In Sub-Saharan Africa and eastern Asia chronic hepatitis B infection has been implicated as the major aetiologic factor. Other aetiologic factors include alcohol abuse, chronic hepatitis C and aflatoxin which have all been linked to Liver Cirrhosis [1,2]. Primary liver cancer in pregnancy is rare with very poor prognosis. Studies have reported the maternal and fetal losses as almost 100% in many case reports and series [3]. However, a distinct histological subtype referred to as fibrolamellar HCC (FLHCC) is associated with a better prognosis and usually in a non-cirrhotic liver [4]. There are no clear guidelines on the management of HCC in pregnancy especially on a cirrhotic background with decompensation and in the presence of e-Antigen positive chronic hepatitis B infection. The current WHO guidelines (March 2015) recommends Tenofovir an antiviral as safe and efficacious in pregnancy for chronic hepatitis B infection but did not discuss options for the triad of pregnancy, HCC and chronic hepatitis B infection [5]. We present a case of hepatocellular carcinoma (HCC) in the third trimester of pregnancy with underlying chronic hepatitis B infection and liver decompensation. The management dilemma and outcome of HCC in pregnancy in our client were highlighted.
A 36 year old female farmer gravida 5 para 4 at 27 weeks gestation presented to our facility. Her main complaint was a 3 month history of epigastric abdominal pain, which was gradual in onset, dull and persistent. Pain had gradually worsened over the months with no known relieving or aggravating factors but with intermittent radiation to the chest. There was a history of significant weight loss but no associated early satiety, jaundice, fever, itch or spontaneous bleeding. No history of blood transfusion and patient was on her routine hematinic from the antenatal clinic (ANC). She is not a known diabetic, Hypertensive and has no known chronic illness. Patient did not know her Hepatitis status. Denied to taking any alcohol or smoking. There were no cardiorespiratory nor urogenital symptoms. She did not store grains at home and had no known contact with chemicals or ionizing radiation. Clinical signs on examination included wasting, mild pallor, a tinge of jaundice but well hydrated, afebrile and no palpable lymphnodes. She had palmer erythema but no clubbing and parotid enlargement. Respiratory, cardiovascular and neurological examinations were unremarkable. Abdomen was grossly distended with distorted contour in the upper half and visibly distended anterior abdominal wall veins draining away from the umbilicus. Liver was enlarged 12cm below the costal margin with a span of 17cm. The liver was hard, nodular with irregular edge,mild tendernes and had a bruit on auscultation.The spleen was not palpable but with demonstrable mild ascites and bipedal eodema up to the mid shin. Symphysio fundal height was 26 cm, with longitudinal lie and breech presentation. Fetal heart rate was 134bpm and regular.Rectal and vaginal examination were unremarkable.Initial diagnosis of hepatocellular Carcinoma in pregnancy was made.
�
Laboratory assesment revealed HB-10.3g/dl, WBC 10200 cells/dl; Neutrophils 59.3%, lymphocytes 26.1%, Monocytes 10.1% and Eosinophils 2.7%. Platelets 350000/ul.Normal bilirubin but GGT and AST were raised (4times upper limit). Total protein and albumin were low, 44g/L and 29g/L respectively with INR-1.3.HBsAg was positive, HBeAg negative with HBV DNA level of 126869 IU/ml(Viral load). VDRL positive but TPHA not done. Alphafeto protein (AFP) >50000KU/L. She tested negative to HIV and HCV. Abdominal ultrasound showed a heterogeneous coarse liver with multiple hypoechoic lessions. The liver measured 17.2cm and there was mild ascites. Pelvic scan revealed a 27 week, 3 day old fetus, with active fetal movements. A revised diagnosis of hepatocellular carcinoma on a cirrhotic liver with decompensation in pregnancy was made. She was managed with analgesia,furosemide,spironolactone and lamivudine added for prevention of mother to child trasmission of the hepatitis B infection. The plan was to allow pregnancy to continue to at least 32 completed weeks to improve the chance of neonatal survival. However because of the progressive unbearable abdominal pain,pregnancy was terminated at 30 weeks 3days by successful induction of labour. The outcome was a fresh stillbirth weight 1.2kg. Pain was markedly reduced post delivery and was discharged home after 5days. She was booked for a follow up visit at the gastrointestinal clinic. She was seen at the clinic at 2 weeks and four weeks post discharge but was lost to follow up afterwards (Figure 1, Figure 2).
Hepatocellular carcinoma is rarely associated with pregnancy and its occurrence together has a poor prognosis for both the mother and the baby [6,7]. Our patient presented in the third trimester with features suggestive of hepatocellular carcinoma (large nodular liver with a bruit and significant weight loss). The diagnosis was confirmed with abdominal ultrasound and markely elevated alpha fetoprotein (AFP) ie > 50,000 KU/L bearing in mind that AFP is also raised in pregnancy and flare of chronic hepatitis B infection. The AFP value obtained for this patient is extremely high and usually seen in clients with HCC. The pregnancy and a possile flare of hepatitis B infection cannot explain the high AFP value in our client. She did not know her hepatitis B status but the results from our laboratory showed that she had e-antigen negative chronic hepatitis B with HBV DNA level of 126869 IU/ml. This clinical picture suggests a possible pre-core or core promoter mutation in our client as usually e-antigen negative patients are in the immune control phase with very low viral loads. Our client also had features of liver decompensation and the ultrasound rightly described HCC on a cirrhotic background. Oestrogen is known to stimulate hepatic growth, alter liver metabolism, and endogenous hormones may contribute to the rapid growth of liver cancer during pregnancy in the context of our client [8]. With the cirrhotic background in her case it may be that she had the HCC before the pregnancy but was small in size which the pregnancy factors catalysed its growth to a symptomatic phase. There is a remarkable increase in oestrogen levels during pregnancy. Our client engaged in active farming during pregnancy and with the evidence that aerobic exercise can affect the hypothalamic-pituitary-gonadal axis, this may lead to a reduction in oestrogen and progestogens from the ovaries [9]. This may explain why our client only reported in the last trimester since the early phase had less symptoms. We could not assay the hormone level to confirm this as she only reported to us in the last trimester for the first time.
�
There should be a careful evaluation of all pregnant women especially when abnormal masses are seen in the liver on abdominal sonography. Further investigations with magnetic resonance imaging (MRI), Triphasic Computerised tomography together with maternal serum AFP and amniotic fluid AFP if the facilities are available will help identify pregnant women with liver cancer for early optimal management of the mother and baby. In the case of HCC with pregnancy and chronic hepatitis B infection there are no clear guidelines. The current WHO guidelines indicates that treatment in adults with chronic hepatitis B also apply to pregnant women. Tenofovir and or lamivudine or emtricitabine is recommended as it has a better resistance profile and more extensive safety data in pregnant HBV positive mothers [5,10]. The guideline did not make a recommendation on the use of antivirals for preventing mother to child transmission as trials are on-going but recommends first dose vaccine within 24 hour of delivery [10]. The decision to terminate a pregnancy in this context at any point in time may be a call by the doctor but decision purely rest on the clients consent. Regular follow up during and after delivery is recommended in all cases.
Management of chronic hepatitis B infection complicated by hepatocellular carcinoma in pregnancyposes a treatment dilemma as the continuance of the pregnancy accelerates disease progression. Clinicians should add to the body of knowledge to help develop evidence based guidelines to improve maternal and fetal outcomes in clinical practice.
The authors declare no competing interest.
AYA conceptualized, clinical care and wrote this paper, AE clinical care an wrote the paper,ODD clinical care and reviewed the paper, AJ clinical care and reviewed the paper. All authors have read and agreed to the final version of this manuscript and have equally contributed to its content and to the management of the case.
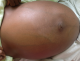
Figure 1: showing massive hepatomegaly with distended veins and the pregnancy
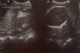
Figure 2: fetal head and the hepatomegaly with HCC in ultrasound view
- Trichopoulos D. Etiology of primary liver cancer and the role of steroidal hormones (editorial). Cancer Cases and Controls. 1992 Jan; 3(1):3-5. PubMed | Google Scholar
- Egwuatu VE. Primary hepatocellular carcinoma in pregnancy. Trans Royal Soc Trop Med Hyg. 1980;74(6):793-4. PubMed | Google Scholar
- Ndububa DA, Makinde ON, Ojo OS, Olasode BJ, Adetiloye VA, Famurewa OC et al. Case report: Hepatocellular carcinoma in pregnancy and postpartum period: a study of 6 cases in Nigerian women. Niger J ClinPract. 2004;7:46-9. PubMed | Google Scholar
- Kroll D, Mazor M, Zirkin H, Schulman H, Glezerman M. Fibrolamellar carcinoma of the liver in pregnancy: a case report. J Reprod Med. 1991; QT:823-7. PubMed | Google Scholar
- Petersen J, Heyne R, Mauss S, Schlaak J, Schiffelholz W, Eisenbach C. Effectiveness of tenofovir for chronic hepatitis B infield practice - 2-year interim results from the prospective German Multicenter Non-Interventional Study (GEMINIS). J Hepatol. 2013; 58:S313. Google Scholar
- Wang LR, Jeng CJ, Chu JS. Pregnancy associated hepatocellular carcinoma. Obstet Gynecol. 1993; 81:811-813. PubMed | Google Scholar
- Umeora OU, Egwuatu VE, Esike CO. Maternal mortality following primary liver cell cancer in pregnancy in a Nigerian. Ann Afr Med. 2006; 5:163. PubMed | Google Scholar
- Hsing AW, McLaughin JK, Hoover RN, Co Chien HT, Blot WJ, Fraumeni JF Jr. Parity and primary liver cancer among young women. J Natl Cancer Inst. 1992,July 15;84:1118-9. PubMed | Google Scholar
- Wolman RL. ABC of sports medicine: Osteoporosis and exercise. Br Med J. 1994August 6; 309:400. PubMed | Google Scholar
- Guidelines for the prevention, care and treatment of persons with chronic hepatitis b infection. March 2015, (2) Chapter 11.6. Google Scholar