Management of biomedical waste in two medical laboratories in Bangui, Central African Republic
Augustin Balekouzou, Christian Maucler Pamatika, Sylvain Wilfrid Nambei, Marceline Djeintote, Dahlia Mossoro, Kazambu Ditu, Bekolo Cavin, Etapelong Gerarld Sume, Marie Claire Okomo, Boniface Koffi, Yin Ping
Corresponding author: Ping Yin, Department of Epidemiology and Biostatistics, School of Public Health, Tongji Medical College, Huazhong University of Science and Technology; Hangkong Road 13, Wuhan City, Hubei Province, China 
Received: 04 Jan 2016 - Accepted: 10 Apr 2016 - Published: 26 Apr 2016
Domain: Epidemiology
Keywords: Management, biomedical waste, laboratory, Central African Republic
©Augustin Balekouzou et al. Pan African Medical Journal (ISSN: 1937-8688). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Augustin Balekouzou et al. Management of biomedical waste in two medical laboratories in Bangui, Central African Republic. Pan African Medical Journal. 2016;23:237. [doi: 10.11604/pamj.2016.23.237.8786]
Available online at: https://www.panafrican-med-journal.com//content/article/23/237/full
Original article 
Management of biomedical waste in two medical laboratories in Bangui, Central African Republic
Management of biomedical waste in two medical laboratories in Bangui, Central African Republic
Augustin Balekouzou1,2,3, Christian Maucler Pamatika4, Sylvain Wilfrid Nambei5, Marceline Djeintote6, Dahlia Mossoro7, Kazambu Ditu3, Bekolo Cavin2, Etapelong Gerarld Sume2,3, Marie Claire Okomo2, Boniface Koffi5,6, Yin Ping1,&
1Department of Epidemiology and Biostatistics, School of Public Health, Tongji Medical College of Huazhong University of Sciences and Technology, Wuhan, China, 2Faculty of Medicine and Biomedical Sciences, University of Yaound� 1, Cameroon, 3Central African Field Epidemiology and Laboratory Training Program, University of Yaound� 1, Cameroon, 4Hospital laboratory friendship Bangui, Central African Republic, 5Faculty of Health Sciences, University of Bangui, Central African Republic, 6National Laboratory of Clinical Biology and Public Health, Bangui, Central African Republic, 7Pediatric Complex, Bangui, Central African Republic
&Corresponding author
Ping Yin, Department of Epidemiology and Biostatistics, School of Public Health, Tongji Medical College, Huazhong University of Science and Technology; Hangkong Road 13, Wuhan City, Hubei Province, China
Introduction: this cross-sectional study was conducted among 73 healthcare workers in two laboratories in Bangui, using self administered questionnaire and scale grid to get information on knowledge and practice of management biomedical waste (BMW).
Methods: data were analyzed using SPSS software (version 20). Fisher chi-square test was used to investigate whether distributions of categorical variables differ from one another.
Results: findings from this study shows that; a gap in legal framework on BMW. Seventy percent of waste generated was infectious. Segregation and color coding was inappropriate. Only 29% of the services used safety boxes. Transport of BW is manual. About 64 % of respondents have not received training on BMW. 44 of 73 (60%) didn�t know certain diseases related to poor waste management and transmission routes. The surface technicians had significantly better knowledge about tetanus vaccine than the medical-technical staff (χ2 = 4.976, p=0.047). They had also a significantly higher risk of exposure to accidents due to waste handling than medical-technical (χ2=10.276, p=0.009). The 30-39 age group had a significantly higher risk of exposure to accidents related to the BMW compared to other ages groups (χ2=11.206, p=0.026).The National Laboratory personal has significantly higher knowledge about BCG and Meningitis vaccine than the Laboratory of Community Hospital personal (χ2=10.954, p=0.002 and χ2=4.304, p=0.05).
Conclusion: BMW was poor. Collaboration between the City Hall and sanitation services with the support of partners will greatly reduce the risk of exposure faced by laboratory personnel and the population.
Biomedical waste (BW) consist of liquid and/or solid waste, toxic and radioactive waste from diagnostic, treatment, prevention or health services [1]. Hospital waste management is a topical issue, given the various potential risks to human and environmental health [2]. The sound disposal waste produced in the laboratory is one of the key aspects of hygiene. This lack of hygiene affects not only within the hospital, but also the general environment. The risks associated with biomedical waste are infectious, toxic, psychosocial trauma, radioactive and environmental [3]. The BW management involves segregation, collection, transport, storage and disposal. This ensures hygiene in hospitals, security of staff and the community [4]. Adequate knowledge of these risks may be a vital factor in the proper disposal of waste [5]. The lack of awareness of proper waste management, the health hazards associated with BW, insufficient human and financial resources, and improper disposal are the major problems linked with healthcare waste management [6]. Few studies have shown that the current conditions of disposal of hospital waste are not always satisfactory in developing countries. In 2002, an investigation conducted by the World Health Organization (WHO) in 22 developing countries showed that the proportion of hospitals not implementing good waste disposal practices varied between 18-64% [7]. Faced with this alarming situation, WHO launched a global challenge for the safety of care treatments and proposed as a strategy BW management for prevention to the various risks incurred [8].
In Central African Republic (CAR), the management of BW remains developing. The law or regulation relating to BW management is not specific. However, to regulate waste management, health facilities often use the hygiene code of the CAR which includes provisions of articles relating to the management of BW. We can cite Articles 77 and 78 relating to cleaning systems of waste water; then articles 106 and 108 on air pollution and finally article 112 prohibiting the storage of waste all categories of non-prescribed manner. However, the framework project on the environment CAR had also planned regulatory provisions on sound management of hospital waste, but this document still pending approval. To predict collection requirements, packaging and waste treatment, it is obvious to know the amount of waste produced every day. Regarding CAR, estimating the amount of waste produced was conducted in 2007 by the Emergency Support Project has multisectoral fight against HIV / AIDS under average 1288 kg per day of waste from 746 hospitals in the country. In addition, a study of waste management in laboratories and hospitals has never been performed. We found necessary to perform this study on the knowledge and practices of healthcare workers in BW management within two diagnostic laboratories in Bangui with a view to improve the hygiene and safety of the environment and to reduce the risks related to them.
The cross-sectional and descriptive study conducted from 1st May to 31st July 2012, at two diagnostic structures in Bangui: the National Laboratory (NL) and Laboratory of Community Hospital (LCH), both are referral centers for patients, and coaching for health professionals. The NL includes 10 units against 4 for the LCH; in addition employ 59 and 17 personals respectively. The technical staff represents over 80% of the staff of both laboratories. The sample was obtained using randomized sampling to first identify the laboratories from a total of 6 references within the selection criteria. The second to choose anyone working in the identified laboratories and agree to participate in the study. These two laboratories have 73 healthcares workers (HCW), including doctors, laboratory technicians, surface technicians and administration staff. These HCW were interviewed and observed for BW practices. Three types of questionnaires were designed to collect the data. The first questionnaire was composed of 23 items for administrative staff to understand the policy of BW management in their institutions; the second had 41 items for medical and technical staff for the assessment of their knowledge for the BW management and risks; the third with 39 questions concerned the surface technician to measure their behavior during the handling of the waste. A weighing device was used to deduce the weight of solid waste generated daily in laboratory investigations. The camera was also used for the observations during the investigation.
Statistical analysis
Data was analyzed using the statistical package for the social sciences (SPSS) version 20 (SPSS inc., Chicago, Il, USA). Chi-square test/ Fishers� Exact test were used to compare categorical data, including age between the two groups. Two way tables were utilized to assess the relationship between dependent and independent variables. The symbols �1� for the correct answer, and �0� for the wrong answer to every question were to assess the knowledge and practice of survey respondents. A total score is calculated for each participant. Permission to carry out this study was obtained by the Central African Republic Ministry of Health and corresponding ethics committee (N�114/MSPP/DLNBCSP/SAP/12).
Socio demographic characteristics of participants
Ninety questionnaires were administered, 73 were returned giving a response rate of 81%. In total, 14 units or services concerned by this study were enrolled in two medical laboratories in Bangui, capital of Central African Republic. However, interviews and observation on waste management were done in all services. NL has more personnel than the LCH (76.8% vs 23.2%) with more men than women (57.2% vs 42.8% in NL and 70.5% vs 29.4% in LCH). The mean age was 44.40 � 9.2. Medical-technical group represented 78.1% of all staff, followed by the administrative staff (12.3%) and surface technician (9.5%). The 30-39 years age group more prevalent among the NL staff (35.7%), while it was the 40-49 age group that was the majority in the LCH personal (35.2%). The majority of respondents of both laboratories had more than one year work experience (82.2% in NL and 64.7% in LCH). More than half of personal (56.1%) were civil servants. However, there was no significantly different among two laboratories regarding socio demographic variables (Table 1).
Knowledge about biomedical waste management in two laboratories
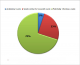
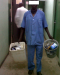
The Figure 1 shows that potentially infectious waste represent 70% of all waste generated by the both laboratories, followed by 25% for waste assimilated with garbage house ware and 5% body waste. However, the two laboratories produce monthly 78.13 and 102 kilogram of waste respectively for the community hospital laboratory and the national laboratory (Table 2). In addition, infectious wastes are found in three quarters of the services except for administrative services that produce only for household waste. Table 3 shows that the sorting of waste was systematic (64%) in all services of the two laboratories. While sorting inadequate (lack of waste separation) represented 42.8% in NL and 35.7% in LCH, totaling 79% of all surveyed services. However, the color coding system for different categories of waste was similar (1.5%) in both laboratories. Our study shows that the garbage bags were available in 100% of services. By cons, safety boxes for the collection of sharps were available in 29% of services. The proportions of the availability and use of safety boxes were similar (14.2%) in each laboratory. This study showed that the use of safety box was inappropriate because often exceeded filling � of its contents (Figure 2). Pathological wastes were packaged in plastic containers with lid and containing 10% formalin. In addition, recycled wastes (Petri dish, glass speculum, the hemolysis tube and slides objects) were directly deposited in a bleach solution at 10% and then autoclaved. Generally, waste collections are daily except on non-working days. There was no trolley in both laboratories and the transport was done by gloved hand (NL, Figure 3) or ungloved (LCH, Figure 4). Liquid wastes are directly dumped into pipes running waters without prior decontamination. All waste is stored in a secure central storage location for the NL and insecure for the LCH (Figure 5). Our study revealed that both laboratories do not have a service contract with a private company for waste disposal. Therefore, all combined solid waste with the exception of anatomical waste were disposed of by burning method to the incinerator Pyrolysis kind in the NL and Montfort for the LCH (Figure 6, Figure 7).
Knowledge and practice about biomedical waste management among medical-technical personal and surface technician of both laboratories
Knowledge of the risks relating to poor waste management is inadequate among staff of both laboratories. Over 64.1% of respondents have not received training or retraining on biomedical waste management. About 60% of participants did not know certain diseases related to poor waste management and transmission routes. While most participants judges knew the vaccines useful to their function and also the steps of good management (Table 4). Surface technicians have significantly more knowledge about the tetanus vaccine those medical-technical personnel (χ2=4.976, df=1, p-value=0.047). The practice of good management of biomedical waste is insufficient in both laboratories. Personal protective equipment is nonexistent, all surface technicians, responsible for the collection lacked boot, or protective eyewear. Only six percent of respondents received vaccines against hepatitis C and 14% against the flu. In addition, 57.1% of surface technicians have been victim of at least one accident was mishandling during their profession. The surface technician has a significantly higher risk of exposure to accidents due to waste handling those medical-technical (χ2=10.276, df=1, p-value=0.009). This study shows that the 30-39 age groups has a significantly higher risk of exposure to accidents due to the management of biomedical waste compared to other ages groups (χ2=11.206, df=4, p-value=0.026). On the other hand, there is statistically different among two laboratories regarding knowledge of vaccine useful for the management of biomedical waste. According to the Table 4, the NL personal has significantly higher knowledge about BCG and Meningitis vaccine than the LCH personal (χ2=10.954, df=1, p-value=0.002 and χ2=4.304, df=1, p-value=0.05).
In CAR, the national policy framework is characterized by a legal vacuum associated with BW management. The BW sector is characterized by a multitude of sources of production, difficult to identify, particularly illegal private practice and home care (self-medication). In almost all health facilities and laboratories, there are no plan or procedure managements of BW. Monitoring is usually done by sanitation. However, hygiene and safety officials assigned to these structures do not have sufficient material and financial resources to cope with this difficult task. In addition, the budget for waste management is often melted in the entire maintenance budget, making it difficult to cash outflow for the regularity of good waste management. Generally, waste management is not often ranked among the priorities of hospitals over drugs and reagents. As an example, our study showed that the exact amount allocated in the budget was not mastered by the leaders of the surveyed laboratories. This observation is consistent with the study by Al-Emad in 2011 in Yemen, but contradictory to those of Mahamat Nour in 2009, which showed that 1.67% of the waste budget in the overall operating budget [5, 9] .
It appears from this study that the monthly amount of solid waste generated in these laboratories was 78.73 kg for the LCH and 102 kg for NL. LCH production represents 22% difference to that of NL. The NL which is a national reference institution with more technical units producing more waste than the LCH. Our results are in disagreement with the studies by Amidou in 2009 at the B� Hospital in Lom� and Mahamat Nour in Ouagadougou who found respectively 4.8 tons and 2.90 tons of waste per month [9, 10]. This difference could be explained by the fact that their studies were performed in all of the hospital; which allowed them to have a great production compared to our study which concerned only the services of the laboratory. The laboratory activities are usually related to infectious products (body fluids..), that�s why our results showed that over 70% of wastes are potentially infectious, contrary to WHO guidelines which state that infectious BW account for only 10-25% of waste from hospital. Good management of hospital waste guarantees the safety of the survival of the person generating and the surrounding population. It includes the following steps: sorting, packaging, storage, treatment and disposal according Connor in 1990 and the WHO Bulletin 2005b [11, 12]. The results in Table 2 of this study allowed us to confirm that respondents laboratories do not have a particular system of coding the pre collection of materials (97%) in contrast to WHO recommendations on the use of bags different color for each category of waste including red for infectious, black or the other for waste assimilated with household refuse and rigid boxes for needles and sharp objects. In reality, the two laboratories use only one type of black garbage bag but varied capacity (25 L and 100 L) for any class of waste. The results of our study are also far from those of a study by Ndiaye et al. in Dakar which revealed that the use of color coding system was effective in 31.4% (27/86) services [2]. The lack of use of the coding system could be justified by inadequate explanations in the field of sorting the administrative authorities of the surveyed laboratories and financial difficulties faced by our health facilities. However, this encoding, allowing the identification and separation of BW, significantly reduced the amount of waste requiring special treatment, and the cost of this treatment [13].
In our study, the majority (64%) of respondents have achieved personal replied systematic sorting of waste in the units of analysis by separating the infectious waste and household waste. On the contrary, the results of our observation (not signify in the tables) showed that only 33% of services NL and 0% of services LCH actually applied on sorting waste at source while sorting was inadequate in 42.8% of the NL services and 35.7% in the LCH (Table 2). Our results are similar to the study by Ndiaye et al. in Dakar when 46.5% of the services claimed systematic sorting while inadequate in 53.5% of services [2]. In contrast to our results, routine screening is nonexistent in Mahamat Nour research in Ouagadougou [9]. This weakness is due to lack of training and staff awareness of the importance of sorting waste at source and the lack of adequate materials for pre waste collection. Normally the separation of waste by category had the advantage adaptation of treatment and disposals are applied to them. However, the results of our study show that very few of the services actually separate their waste into account their infectious nature. But Salamatou et al. have shown in their research the importance of this provision, which would be implemented by 85% of structures evaluated by the authors [13]. In the practice of protection of personnel and population against contamination from sharp or sharp objects, WHO recommended the use of rigid safety boxes. Our study showed that only two services each surveyed laboratories have at least a safety box, 29% (4/14) and use them. However our investigations have revealed that these boxes were provided by the Expanded Program on Immunization (EPI) in partnership with a legal source is unknown. Despite the availability of this security box in the above mentioned services, we see the disregard of instructions filling � and that they are often filled to the brim with overflow before transfer to storage. This practice is also found in the study of Ndiaye et al. that despite the availability of safety boxes in 82.5% of services, only 55.1% are employed [2]. Transporting BW within the services to the storage place is a step to risk of contamination. This transport must follow a remote circuitry areas frequented by patients and visitors and with maximum security using adjustable medical carts. However, our study showed no laboratory has any trolley for transportation, and transportation was done by hand by surface technicians every morning for work days. This practice could lead to serious problems in case of accidental fall. A study done at the regional hospital in Ziguinchor in Senegal also shows risky transport conditions with the use of trolleys and bins worn on the back or head [14].
The storage of risk waste requires special conditions, namely secure location, locked, easy to clean, well lit, ventilated and denied access to anyone outside the service. They also used for this type of waste material must be exclusively reserved for this purpose and secured to the stage of elimination [15]. In Table 2, 100% of respondents declare the availability of a central repository of waste. Rather, this storage location does not meet the conditions previously demonstrated (Figure 6, Figure 7) to the CHL. This situation is the same in the study by Daoudi at the Hassan II Hospital in Agadir, Morocco, where there is a complete lack of storage places [16]. By cons, studies by Mahamat Nour at CHUP-CDG in Ouagadougou and Ndiaye in Senegal show that storage is done in a specific room for the storage of waste [2, 9]. According to the international guidelines of the WHO, the real-time storage of waste outside the laboratory however, should not exceed 48 or 72 hours [17]. This principle was respected by the NL which eliminated its waste stored every 48 hours, for against the LCH; the frequency of disposal of waste daily given the amount of waste generated by the entire hospital but remains theoretical. Our study found that the time of disposal was not respected by the agents responsible for the community hospital (Figure 6). In addition, liquid waste collected for automaton should be disinfected with bleach (sodium hypochlorite) before being discharged while those dyes and other Gram are directly discharged without treatment prior. Our results agree with those of a study conducted by Zana Coulibaly et al. in Ivory Coast revealed that untreated effluent is discharged to the sewer system through the basins and sinks to 73, 3% of cases, or thrown away in 40% of cases [18]. This is a procedure which, according to Evans in 2004 in France, increases environmental pollution risk not only by potentially pathogenic microorganisms, but also heavy metals, detergents and organic halogen [19]. It appears from this study that the level of knowledge of laboratory staff on the management of BW is low with 64% unqualified personnel. These results are similar to the study by Ndiaye in Senegal in 2010 with a low level of knowledge estimated at 62.6% (47/86) of surveyed workers [2]. In addition, they are mostly informed about the risks associated with BW and the existence of management protocol in case of accidents due to handling waste. That is why only 38% of respondents knew about diseases related to poor waste handling and mode of contamination. In other hand, more than half of the participants were aware of the steps in the process of good management of BW.
However, the standards recommend that no staff member should handle risk waste without having been advised and trained in safety procedures [17, 20]. So that the non-respect of good waste handling practices expose collectors to infections with Mycobacterium tuberculosis with lung infections or pneumonia or skin-related fungal flora [21, 22]. For reducing the risk of infection from collecting, the law establishes an individual responsibility but also an institutional responsibility for training and support, and more generally, a national responsibility for the establishment of a regulatory framework [20]. For the management of health risks, our results have shown that the vaccines are considered important for personnel as part of his professional activity are summed to BCG, Typhoid fever, Hepatitis B and Meningitis, which represent more than 55%. However, surface technicians have significantly more knowledge of Tetanus vaccine as medical-technical staff (χ2 = 4.976, df = 1, p-value = 0.047). This knowledge would be linked to the risks incurred during their daily exercise function. In addition, the study showed that more than 82% of obligatory vaccinations are not administered to the staff of the surveyed laboratories. Therefore 15.6% of workers have been victims of at least one case of injury to the handling of waste in the last 12 months of the study. However, the risk of accidents is significantly higher for surface technicians than other laboratory personnel (χ2 = 10.276, df = 1, p-value = 0.009). It is also noted that only two (20%) of these accidents are reported to administrative authorities. Our results can approach the study of Blood Exposure Accidents (BEA) conducted by Kone in Mali shows that 64.1% of staff was involved in an accident during their work [23]. Our study also showed that the age group of 30-39 years had a significantly higher risk of exposure to accidents related to handling waste than other age groups (χ2 = 11.206, df = 4, p-value = 0026). Also note that the NL personal had significantly more knowledge on vaccines against tuberculosis and meningitis than those of LCH (χ2 = 10.954, df = 1, p-value= 0.002 and χ2 = 4.304, df = 1, p-value= 0.05). Habits of good practices observed in this study show that some personal confident of their seniority at work do not observe basic rules of wearing gowns and gloves during the short term manipulations [24, 25]. Despite this alarming situation, the medical staff, technical and sanitary personnel is aware of the risks associated with handling of BW, even if the majority is not formed on their management. However, in practice, there is some negligence in the sometimes deplorable behavior, particularly in terms of support staff such as laboratory assistants, whose level of knowledge and awareness on the management of BW is significantly lower than among doctors, biologists and technicians. There are over a decade, the basic training program of such staff (paramedical) do not include courses on biomedical risks. In addition, the concern of the laboratory personnel for emergency analyzes appear to be the major reason for the lack of interest in the management of BW. This observation raises the question of urgency and responsibility of personal hygiene in the management of BW, and must also ensure public safety in health facilities where they are assigned.
Analysis of the waste management in the two laboratories of the study is dominated by legislation deficiency. The coding system is nonexistent. The sorting is performed in a quarter of the two laboratories services. Transport of waste remains manual and the storage time is not observed in a laboratory on two. Waste disposal is made by incinerators. However, knowledge and protection of employees are insufficient. This requires capacity building of agents involved in the management of BW. For this, collaboration between the City Hall and sanitation services with the support of partners will greatly reduce the risk of exposure faced by laboratory personnel and the surrounding population of disposal of this waste site.
What is known about this topic
- In CAR, the management of BW remains embryonic. It is based on knowledge acquired during professional training for personnel managers or self-study for surface technicians. Habits of good practices recommended by WHO are not put into practice, exposing personnel who handle the waste and the population alongside waste production sites is a high risk of accidental contamination or infectious origin;
- The law or regulation relating to BW management is not specific. However, to regulate waste management, health facilities often use the hygiene code of the CAR which includes provisions of articles relating to the management of BW;
- Training and retraining were organized for the staff working in diagnostic structures in 2010 and 2011 but this does not include the cleaning staff, first at risk of waste handling.
What this study adds
- Our study had identified weaknesses in the waste management in the respondent�s diagnostic structures. Awareness for the staff of both laboratories about good practice in the laboratory was organized in October 2012 during the session of restitution results of this study;
- An editorial plan procedure manual of the BW management was developed and offered to health officials. Also the transport circuit definitions and timing waste disposal were introduced;
- It is also important to note that plugs and accident report register were introduced in laboratories surveyed. Several recommendations to improve healthcare waste management were made and given to political and health officials CAR.
The authors declare no competing interests.
BA conceived of the study, and designed the protocol, supervised the data collection and provided writing. PCM collected data. DM participated in the design of the study and performed the statistical analysis. NSW and All authors read and approved the final manuscript. DK, DD and KB have coordinated the work of the entire team.
Staff from: National laboratory and laboratory community hospital, University of Yaounde1,Tongji Medical College of Huazhong University of Sciences and Technology of China, AFENET, CAFELTP, CDC/Atlanta and Melinda Get Foundation for funding this study.
Table 1: socio-demographic characteristics of participants
Table 2: type and amount of solid waste generated in laboratories surveyed in the month of June 2012
Table 3: practical arrangements adopted in both laboratories
Table 4: correct knowledge of participants about health risks associated with biomedical waste
Figure 1: categorical proportion of solid waste generated in two laboratories investigations in june 2012
Figure 2: safety box exceeding the filling � of its content before proceeding to their elimination
Figure 3: transport waste to the central storage area of national laboratory
Figure 4: the surface technician has no glove, cart, or flap during transport of waste services to the central storage area of the laboratory community hospital in Bangui
Figure 5: the hospital hygiene service violates the waste disposal timing. Therefore, these wastes are spread around the storage center has the Bangui community hospital
Figure 6: pyrolysis type of incinerator at the national laboratory is semi-modern with little release smoke during waste disposal
Figure 7: montfort type of incinerator at the laboratory of community hospital is an old inefficient incinerator, with significant smoke during waste disposal
- Kishore J, Agarwal R, Kohli C, Sharma PK, Kamat N, Tyagi S. Status of biomedical waste management in nursing homes of delhi, India. J Clin Diagn Res. 2014; 8(3):56-58. PubMed | Google Scholar
- Ndiaye M, El Metghari L, Soumah MM, Sow ML. Biomedical waste management in five hospital in Dakar, Senegal. Bull Soc Pathol Exot. 2012; 105(4):296-304. PubMed | Google Scholar
- Lakbala P, Lakbala M. Knowledge, attitude and practice of hospital staff management. Waste Manag Res. 2013; 31(7):729-732. PubMed | Google Scholar
- Diaz LF, Fisher S, World Health Organization, Health Care Without Harm. Management of healthcare wastes. Waste Manag. 2005; 25(6):567-57. PubMed | Google Scholar
- Al-Emad AA. Assessment of medical waste management in the main hospitals in Yemen. East Mediterr Health J. 2011; 17(10):730-737. PubMed | Google Scholar
- Emmanuel J, Pieper U, Pr�ss A, Rushbrook P, Stringer R et al. World Health Organization (WHO): Safe management of wastes from health-care activities. In WHO Press. 2014; 380, 2nd Edition. PubMed | Google Scholar
- World Health Organization. Wastes from health care. Help Memory. 2000; N� 253. PubMed | Google Scholar
- World Health Organization. World undid Patient Safety, 2005-2006. World Health Organization, Gen�ve. 2004;36. PubMed | Google Scholar
- Mahamat N. Management of hospital solid waste and analysis of health risks CHUP-CDG Ouagadougou. Dissertation of training specialized Master in sanitary engineering and environment. 2009;73. PubMed | Google Scholar
- Amidou S. Contribution to the sustainable management of solid waste in the biomedical health district No. 3 of Lome: B� Hospital case ; diagnosis, analysis of health risks and improvement proposal. Dissertation, International Institute for Water and Environmental Engineering lome. 2009;72. PubMed | Google Scholar
- Connor D. Management Syndrome `not in my backyard 'in the 90: Principles and Cases for Waste Managers. 12e Conf�rence nationale sur la gestion des d�chets, St John�s (Terre-Neuve), Environnement Canada. 1990;1-8. PubMed | Google Scholar
- World Health Organization. Solid waste management activities of care in primary health centers. Help guide the decision Geneva, WHO. 2005;64. PubMed | Google Scholar
- Salamatou J, Ouzounian G, Levebre J. Hospital waste. Document, Observatoire r�gional des d�chets d�Ile de France. 1992;3. PubMed | Google Scholar
- Ndiaye P, Fall C, Diedhiou A, Tal-Dial A, Diedhiou O. Management of biomedical waste at the regional hospital in Ziguinchor. Cah �tud rech franco / Sant�. 2003; 13(3):171-176. PubMed | Google Scholar
- Faye P. Evaluation of the collection project, evacuation and treatment of household waste. Sanitary Engineering dissertation; These Public Health, Institute of Health and Development (ISED), UCAD S�n�gal. 1997;41. PubMed | Google Scholar
- Daoudi MA. Evaluation of the management of medical and pharmaceutical waste solids has the Hassan II Hospital in Agadir. Institut national d�administration sanitaire 9e cours de maitrise en administration sanitaire et sante publique, M�moire. 2008;28-29. PubMed | Google Scholar
- World Health Organization. Preparation of national health-care waste management plans for sub-Saharan Africa. Manual decision support Secretariat of the Basel Convention. 2005a;115. PubMed | Google Scholar
- Zana C et al. Liquid Waste Management in Microbiological Analysis Laboratories in Abidjan, Ivory Coast and Infectious Risk Partner. European Journal of Scientific Research. 2010; 40(2):247-255. PubMed | Google Scholar
- Evens E. Evaluation of the health and ecotoxicological risks of hospital waste: Doctoral thesis, Ecole doctorale de chimie de Lyon. Institut National des Sciences Appliqu�s de Lyon, France. 2004; 260. PubMed | Google Scholar
- D�cret no 94-352 du 4 mai 1994. Relatif � la protection des travailleurs contre les risques r�sultant de leur exposition � des agents biologiques et modifiant le code du travail (deuxi�me partie: D�crets en Conseil d'Etat). Minist�re du travail de l�Emploi et de la Formation professionnelle. Journal Officiel du 6 mai 1994; page 6620. PubMed | Google Scholar
- Johnson K, Braden RC, Caims KL et al. Transmission of Mycobacterium tuberculosis from medical waste. JAMA. 2000; 284(13):1683-1688. PubMed | Google Scholar
- Allmers H, Huber H, Baur X. Two years follow-up of a garbage collectors with allergic bronchopulmonary (ABPA). Am J Ind Med. 2000; 37(4):438-442. PubMed | Google Scholar
- Kon� MC, Mall� K. Blood exposure accidents: knowledge and practices of hospital health workers in Mali. Bull Soc Pathol Exot. 2015 Dec;108(5):369-72. PubMed | Google Scholar
- Cousin M, Gouget B. Hygiene and security in biological laboratories: Symposium immunology biomerieux. Paris-La Defense,France. 1994; 3(4):24-32. PubMed | Google Scholar
- Durand, F Roussill. Disposal of laboratory wastes; Regulatory aspects and recommendations. Spectra 2000 analyse. 1996; 24(182):23-26. PubMed | Google Scholar