Recurrent myocardial infarction in a young cocaine abuser
Rajae Stiha, Zainab Raissouni, Bouchra Ess-bai, Latifa Oukerraj, Jamila Zarzur, Mohamed Cherti
Corresponding author: Rajae Stiha, Cardiology B Department, CHU Ibn Sina, Faculty of Medicine and Pharmacy, University Mohammed V Souissi, Rabat, Morocco 
Received: 12 Jun 2015 - Accepted: 04 Jul 2015 - Published: 10 Jul 2015
Domain: Clinical medicine
Keywords: Cocaine, myocardial infarction, recurrences, prevention
©Rajae Stiha et al. Pan African Medical Journal (ISSN: 1937-8688). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Rajae Stiha et al. Recurrent myocardial infarction in a young cocaine abuser. Pan African Medical Journal. 2015;21:194. [doi: 10.11604/pamj.2015.21.194.7265]
Available online at: https://www.panafrican-med-journal.com//content/article/21/194/full
Recurrent myocardial infarction in a young cocaine abuser
Rajae Stiha1,&, Zainab Raissouni1, Bouchra Ess-bai1, Latifa Oukerraj1, Jamila Zarzur1, Mohamed Cherti1
1Cardiology B Department, CHU Ibn Sina, Faculty of Medicine and Pharmacy, University Mohammed V Souissi, Rabat, Morocco
&Corresponding author
Rajae Stiha, Cardiology B Department, CHU Ibn Sina, Faculty of Medicine and Pharmacy, University Mohammed V Souissi, Rabat, Morocco
Cocaine increases the risk of cardiovascular diseases, including myocardial infarction. We herein describe a case of a 22-year-old man with a long history of cocaine abuse. He presented at our institution because of acute coronary syndrome with ST segment elevation. Emergency coronary angiography revealed ostial occlusion of the left anterior descending artery, which required desobstruction and implantation of a bare metal stent. Angioplasty was complicated 4 months later by in-stent restenosis requiring reintervention. This case highlights myocardial infarction as a cocaine-induced effect. Appropriate treatment and cessation of cocaine abuse may prevent cardiovascular complications and recurrences.
Cocaine is an illicit drug used frequently worldwide. This drug is responsible for severe cardiovascular complications, including myocardial infarction (MI), aortic dissection, cardiomyopathy, arrhythmias, and sudden cardiac arrest. Especially in young adults without significant risk factors.
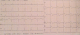
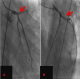
We report a case of a 22-year-old man with a long history of cocaine, cannabis, and tobacco abuse. He presented to our emergency department for onset severe chest pain. An initial physical examination demonstrated a blood pressure of 100/60 mmHg, heart rate of 112 beats/min, and respiratory rate of 18 breaths/min. Cardiovascular and lung examination were unremarkable. Eighteen-lead electrocardiogram on admission revealed a sinus rhythm and elevated ST segment in the anterior leads with biphasic T waves in V1-V5 (Figure 1). Echocardiography showed an ejection fraction of about 28% with anteroseptal, inferoseptal, lateral, and apical akinesis. Urgent coronary angiography revealed ostial occlusion of the left anterior descending artery (Figure 2, A) requiring desobstruction and implantation of a bare metal stent (BMS). The patient was discharged after 5 days (Figure 2, B). He presented 4 months later with typical chest pain at rest. Although he had not discontinued double antiplatelet therapy, he had resumed cocaine use. Catheterization revealed severe in-stent restenosis and the patient underwent a stenting with a drug-eluting stent (DES) (Figure 3). After one year follow-up, our patient remains asymptomatic, and ejection fraction rose to 38%, and he was scheduled for detoxification.
Cocaine is an alkaloid extracted from the leaf of the Erythroxylom coca plant in South America. It is available as a free base and hydrochloride salt and can be administered orally, intranasally, or intravenously, the serum half-life of cocaine is 45 to 90 min. Therefore, MI may occur several hours after ingesting cocaine [1]. Exposure to cocaine has harmful effects on several organs, particularly the heart and its vessels. Cocaine blocks presynaptic norepinephrine and dopamine reuptake in sympathetic nerve terminals, leading to an excess of these neurotransmitters at postsynaptic receptor sites. This adrenergic stimulation increases the heart rate, systemic arterial pressure, and myocardial contractility, all of which induce a significant imbalance in myocardial oxygen demand and supply [2]. Cocaine also acts like a class I antiarrhythmic agent, producing local anesthetic effects by blocking cardiac sodium and potassium channels. Therefore, cocaine exerts two main opposing actions; at low doses, the strengthening of sympathetic activity predominates, whereas the local anesthetic effect is most marked at higher doses [3]. Cocaine induces an endothelial dysfunction which result a coronary vasoconstriction, activation of platelets, increases adhesiveness and aggregability involved in coronary thrombi formation. These effects can be furthermore potentiated by smoke and alcohol [4]. Thus, MI can be related to increased myocardial demand, vasoconstriction and spasm, thrombosis, or accelerated atherosclerosis. In our case, all of these mechanisms seemed to be implicated as indicated by coronary angiography. The occurrence of acute coronary syndrome is unrelated to the amount of cocaine ingested, the route of administration, or the frequency of use [1].
�
Chest pain is a common symptom in cocaine-induced MI, as in our patient. This clinical presentation can be indicative of several etiologies, such as cocaine-induced aortic dissection [5]. An accurate diagnosis of MI may be difficult; the electrocardiographic abnormalities can be related to early repolarization syndrome or ventricular hypertrophy, particularly in young patients. In the present case, the electrocardiographic abnormalities were typical of MI. The serum troponin level should be checked whenever MI is suspected because creatinine kinase is nonspecific due to the occurrence of rhabdomyolysis in cocaine users [6]. Thrombolytic therapy should be considered only if primary percutaneous coronary intervention cannot be performed [7]. Coronary angiography is indicated in ST-segment elevation MI and is even more desirable in the setting of cocaine use [5]. Administration of beta-blockers after MI is controversial. The use of beta-blockers reduces the risk of coronary artery spasms and recurrence of MI [8]. Lange et al. [6] reported that beta-adrenergic blockade increases vasoconstriction when given after cocaine exposure; thus, use of beta-blockers should include a careful risk-benefit assessment. The recurrence of MI in our case can be explained by the resumption of cocaine use and by the BMS.Though cocaine use increases the risk of stent thrombosis within 1 to 247 days after stent implantation; this occurs regardless of appropriate antiplatelet therapy or the discontinuation of cocaine use [9].It is probably prudent to use bare metal stents [10].
MI is a serious complication of cocaine abuse. Early recognition is important for appropriate management. Stopping cocaine use is the primary goal of post-discharge therapy to ensure a better prognosis.
The authors declare no competing interest.
All the authors have contributed to this study in ways that comply to the ICMJE authorship criteria. All the authors have read and approved the final version of the manuscript.
Figure 1: electrocardiogram with ST segment elevation and biphasic T waves in anterior leads
Figure 2: A):
coronary angiography with ostial occlusion of the left anterior descending coronary
artery; B): successful desobstruction and stenting of the left anterior descending
coronary artery
Figure 3: successful angioplasty and implantation of a drug-eluting stent in the left anterior descending artery
- Kloner RA, Rezkalla S. Cocaine and the heart. N Engl J Med. 2003;348:487-8. PubMed | Google Scholar
- Amin M, Gabelman G, Karpel J et al. Acute myocardial infarction and chest pain syndromes after cocaine use. Am J Cardiol. 1990 Dec 15;66(20):1434-7. PubMed | Google Scholar
- Egashira K, Morgan KG, Morgan JP. Effects of cocaine on excitation contraction coupling of aortic smooth muscle from the ferret. J Clin Invest. 1991 Apr;87(4):1322-8. PubMed | Google Scholar
- Anil Om, Ellahham S, DiSciascio G. Management of cocaine-induced cardiovascular complications. Am Heart J. 1993 Feb;125(2 Pt 1):469-75. PubMed | Google Scholar
- James McCord, Hani Jneid, Judd Hollander E, De Lemos JA, Bojan Cercek. Management of cocaine-associated chest pain and myocardial infarction: a scientific statement from the American Heart Association Acute Cardiac Care Committee of the Council on Clinical Cardiolog. Circulation. 2008 Apr 8;117(14):1897-907. PubMed | Google Scholar
- Lange RA, Hillis LD. Cardiovascular complications of cocaine use. N Engl J Med. 2001 Aug 2;345(5):351-8. PubMed | Google Scholar
- Task Force on the management of ST-segment elevation acute myocardial infarction of the European Society of Cardiology (ESC) & al. ESC Guidelines for the management of acute myocardial infarction in patients presenting with ST-segment elevation. Eur Heart J. 2012 Oct;33(20):2569-619. PubMed | Google Scholar
- Philip Dattilo B, Susan Hailpern M. Beta Blockers are associated with reduced risk of myocardial infarction after cocaine use. Ann Emerg Med. 2008 Feb;51(2):117-25. PubMed | Google Scholar
- McKee SA, Applegate RJ, Hoyle JR, Sacrinty MT, Kutcher MA. Cocaine use is associated with an increased risk of stent thrombosis after percutaneous coronary intervention. Am Heart J. 2007 Jul;154(1):159-64. PubMed | Google Scholar
- Bryan Schwartz G, Shereif Rezkalla, Robert Kloner A. Cardiovascular Effects of Cocaine Circulation. Circulation. 2010 Dec 14;122(24):2558-69. PubMed | Google Scholar