A retrospective study on incidence of pulmonary tuberculosis and human immunodeficiency virus co-infection among patients attending National Tuberculosis and Leprosy Control Programme, Owo centre
Tony Ifeanyi Ojiezeh, Odunayo Omowumi Ogundipe, Victor Akinpelumin Adefosoye
Corresponding author: Tony Ifeanyi Ojiezeh, Department of Medical Laboratory Science, Afe Babalola University, Ado Ekiti, Ekiti State 
Received: 20 Oct 2014 - Accepted: 09 Apr 2015 - Published: 10 Apr 2015
Domain: Public Health
Keywords: Co-infection, HIV/AID, mortality, mycobacterium tuberculosis
©Tony Ifeanyi Ojiezeh et al. Pan African Medical Journal (ISSN: 1937-8688). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Tony Ifeanyi Ojiezeh et al. A retrospective study on incidence of pulmonary tuberculosis and human immunodeficiency virus co-infection among patients attending National Tuberculosis and Leprosy Control Programme, Owo centre. Pan African Medical Journal. 2015;20:345. [doi: 10.11604/pamj.2015.20.345.5643]
Available online at: https://www.panafrican-med-journal.com//content/article/20/345/full
Original article 
A retrospective study on incidence of pulmonary tuberculosis and human immunodeficiency virus co-infection among patients attending National Tuberculosis and Leprosy Control Programme, Owo centre
A retrospective study on incidence of pulmonary tuberculosis and human immunodeficiency virus co-infection among patients attending National Tuberculosis and Leprosy Control Programme, Owo centre
Tony Ifeanyi Ojiezeh1,&, Odunayo Omowumi Ogundipe2, Victor Akinpelumin Adefosoye3
1Department of Medical Laboratory Science, Afe Babalola University, Ado Ekiti, Ekiti State, 2Department of Medical Laboratory Science, Achievers University, Owo, Ondo State, 3National Tuberculosis and Leprosy Control Programm, Public Healthcare Centre, Owo, Ondo State
&Corresponding author
Tony Ifeanyi Ojiezeh, Department of Medical Laboratory Science, Afe Babalola University, Ado Ekiti, Ekiti State
Introduction: the incidence of co-infection of PTB and HIV/AIDS in sub-Sahara is alarming. The exotic nature of the duo infection may be responsible for high mortality among TB patients.
Methods: a five year retrospective study from January 2008 to December 2012 was carried out using profiles of new cases of PTB individuals that attended National Tuberculosis and Leprosy Control Programme (NTBLCP), Owo centre. A total of 342 new cases were retrieved using a pre-designed case record forms. Vital information on demographic data, social and medical history were retrieved including laboratory results, treatment access and mortality report.
Results: the prevalence of HIV sero - positive individual with PTB among the 342 new cases retrieved was 14.0%. In the studied population, incidence of infection was higher among 35 - 44 years age group, 53.8% are males and 46.2% are females. A total of 28.1% was classified as cured, 9.1% died, and 10.5 % defaulted or transferred out.
Conclusion: mortality due to co-infection is high; there is therefore the need to put-in more efforts to stem the trend of PTB and HIV/AIDs co-infection. The variation in the pattern of co-infection in different localities may be associated with the living condition, cultural and socio-economic factors. Other possible factors are enlightenment campaigns and easy access to treatments which should be step-up.
Tubercle bacillus (TB) is contagious and airborne. It is the second highest cause of death from an infectious disease worldwide, after the human immunodeficiency virus [1]. TB disease in children under 15 years of age (also called pediatric TB) is a public health problem of special significance because it is a marker for recent transmission of TB [2]. The impact of tuberculosis (TB) worldwide remains a serious concern with an estimated 8.7 million new cases (13% co-infected with HIV) and 1.4 million deaths due to TB (430,000 in HIV-infected individuals) in 2011 [3]. In sub-Saharan Africa, where there is an HIV pandemic, most countries have reported that above 30% of patients with active TB are co-infected with HIV. Nigeria has the highest TB burden in Africa and one of the highest in the world (311 per 100,000) [3]. As many as 210,000 new cases of all forms of TB occurred in the country in 2010, with Lagos, Kano, and Oyo having the highest TB prevalence rate. Similarly, Benue has a high TB burden which is attributable to a high HIV prevalence. More than 2 billion people (about one-third of the world's population) are estimated to be infected with Mycobacterium tuberculosis with new infections occurring in about 1% of the population each year [4]. Most infections however, do not progress to TB disease with as much as 90-95% of infections remain asymptomatic [5,6]. According to the World Health Organization (WHO), the global incidence of TB was 9 million in 2005, 13.7 million and 8.8 million in 2010. There were around 1.8 million TB-related deaths worldwide in 2003 and 1.45 million in 2010 of which the vast majority of deaths occurred in the developing countries in sub-Saharan Africa and Asia [4]. Among 1.45 million deaths, about 0.35 million occur in those co-infected with HIV [1]. A total of 10,528 TB cases (a rate of 3.4 cases per 100,000 persons) were reported in the United States in 2011. The primary site of infection in the lungs, known as the "Ghon focus", is generally located in either the upper part of the lower lobe, or the lower part of the upper lobe [7]. Once virulent tubercle bacilli gain access to the alveoli, they are subjected to phagocytosis by tissue macrophages. Effective TB treatment is difficult, due to the unusual structure and chemical composition of the mycobacterial cell wall, which hinders the entry of drugs and makes many antibiotics ineffective [8]. The modern approach to treatment of TB is based on several principles that have evolved over the last four decades. The spontaneous, random, chromosome mutations that confer resistance to each anti-tuberculosis drug prohibit the use of a single agent for treatment [9]. Drugs used to treat TB are classified as first-line and second-line agent. First-line agents are the most effective and a necessary component of any short course therapeutic regimen [10]. Second-line agents are employed when resistance or toxicity to first- line agents occurs. They are clinically less effective than first-line agents and much more frequently elicit severe reactions [10].
Study design
�
The retrospective study on prevalence and mortality rate of co-infection and treatment outcome of new cases of Mycobacterium tuberculosis (TB) was carried out in sub-urban area of Owo, Ondo State, and South west of Nigeria. The community is located at longitude 7� 11' 0" North, latitude 5� 35' 0" East of the equator with an estimated population of 218,886.�
Study population�
New cases of TB patients that attended National Tuberculosis and Leprosy Control Programme (NTBLCP), Owo centre for treatment of TB between 2008 to December 2012 constituted the sample population.�
Study instrument and variables�
New cases of pulmonary TB infection between January 2008 and December 2012 and variables such as bio-data, date of registration, medical history, laboratory result etc., and other information including treatment outcomes and retroviral status were retrieved using structured questionnaire with patients' attendant register.�
Sputum smear microscopy�
The diagnosis was carried out by Laboratory staff in the centre, using Ziehl Neelsen (ZN) technique on triplicate sputum samples of early morning spot collected under standard bio-safety procedures. Result interpretation was according to World Health Organization (WHO) standard.�
Data analysis�
The data obtained from the study were statistically analyzed using frequency and percentage count. Test of variance was used for statistical significant difference.
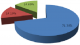
The age and gender distribution of new cases of PTB in NTBLCP, Owo centre from January 2008 to December 2012 is shown on Table 1. The infection rate was more among the males (53.8%) than the females (46.2%). The prevalence of PTB was higher among 35 - 44 years age group, about 70.8% of the set were males. The infection rate among children of less than 14 years age was 5% of the studied population. The incidence of PTB and HIV/AIDS sero-positive individual infected among the studied population within the five-year period was 14.0%. About 71.3% were sero-negative and 14.6% were undetermined. Figure 1 show HIV/AIDS co-infection with tuberculosis in NTBLCP Owo centre. Out of 342 new cases of PTB in the centre, 286 received treatment regimen I while the remaining 56 received treatment regimen II, out of which 28.1% were classified as cured, 9.1% as dead, and 10.5% defaulted. The remaining 52.3% were transferred cases to other health facility outside Owo centre. Figure 2 shows the outcome of treatment regimen of tuberculosis in NTBLCP Owo centre between January 2008 and December 2012.
The study was designed with an aim to recover information and data of incidence of new cases of PTB and HIV/AIDS co-infection in semi urban area Southwestern part of Nigeria. Early researchers have documented correlations between TB and HIV infection such that, mandatory screening of TB patients for HIV has been instituted. The link between HIV/AIDS and TB is a question of immunological competence, the reduction in cellular immunity due to HIV infection enhances the development of pathogen in a host. The lowering of host immunity of individual give way to the opportunistic infections. Exotic bacterium such as Mycobacterium will utilize the immunological incompetence of the host and cause havocs. A total of 14.10% co-infection with HIV sero-positive individual was observed in this study. This finding is judicious, when compared with the incidences reported in Tanzania and Guinea which showed higher values, but when compared with the report from Lagos and Plateau, Nigeria, there is an upsurge that requires urgent attention of government at all level to abate the spread. This result is in consonance with the reports of Tsaku et al. [11]. The analysis of the data of the five years on focus reveal that there is an increase of co-infections among sexually active, productive / childbearing persons aged 34 - 44 years. Individuals in this age group were more vulnerable to TB infection and comprised of young adults which forms the work force and bread winners of the families. A total of 70.8% of this subset are males, which means that males are highly exposed to the infection than the females, nonetheless the difference is statistically insignificant at P > 0.05. This finding is in tandem with the report of Iliyasu and Babashani [12] in Kano, and Maori [13] in Gombe but does not agree with the report of Nwobu et al. [14] in Edo and Onubogu et al [15] in Lagos. The variation in the pattern of co-infection at different zone may be associated with the living condition of the people, cultural and socio-economic factors. Other possible factors may include little or no enlightenment campaigns and difficulty in accessing treatments, and poor laboratory diagnosis.
�
The cure rate of TB infection is relatively low perhaps indicating the emergence of multi drug resistant strains of TB in the population studied. Even when WHO recommended regimen for TB treatment and control is free i.e. Directly Observed Treatment, Short-course (DOTS). The STOP TB partnership launched in 2006-2015, sets out the activities that will make impact on the global burden of TB which involves reducing the incidence of TB by 2015 [4]. Non-adherence to treatment regimen may not be unconnected to re-emergence of TB, because of the production of multi-drug resistant strains that are more virulent [16]. This may also explain why the cure rate is low [17,18]. Living condition and unhygienic practice of infected individual to handling of pulmonary exudates may be culpable as well. Overcrowding in most of the homes, living in poorly designed, unplanned housing and environment may precipitate the persistence of this age-long disease in our society. Hospitalization in special centre may be recommended, to reduce contact with the larger populace. This study observed 9.1% death rate among the population that attended the centre within the year on focus. This finding is analogous with the report of WHO [4], in which TB death rates declined from 11% in 2006 and then getting better as year goes by. The decline in death rate due to TB is clear evidence that WHO and donor agencies are making positive impacts in reducing global burden of TB and this is not unconnected with the commitment and effort of the contributing partners that have continued to support the programme.
Incidence of new cases of tuberculosis is high and the cure rate is still low. Everyone should be concerned with high mortality rate of co-infection of PTB and HIV/AIDs infection. If this trend is left unchecked, it will certainly increase the risk of getting others infecting to the fact that PTB is airborne.
The author's declare no competing interests.
Omowumi Odunayo Ogundipe participated in its coordination and acquisition of data. Tony Ifeanyi Ojiezeh substantially contributed to conception, design, and interpretation of data, drafting of manuscript and revising it critically for important intellectual content. Adefosoye Victor Akinpelumi contributed in data collection. All authors read and approved the final manuscript
The authors wish to acknowledge the Mrs. B. B. Imoukhuede of NTBLCP, Owo centre, for the assistance rendered during data compilation.
Table 1: age and gender distribution of new cases of PTB NTBLCP, Owo centre from January 2008 to December 2012
Figure 1: the occurrence of tuberculosis and HIV/AIDs co-infection in NTBLCP Owo Centre between January 2008 and December 2012
Figure 2: the outcome of treatment regimen of tuberculosis in NTBLCP Owo centre between January 2008 and December 2012
- World Health Organization. Tuberculosis IGRA TB Test, Policy Statement. The use of TB Interferon-Gamma Release Assays (IGRAs) in Low- and Middle-income Countries. 201. PubMed | Google Scholar
- Kabra, [edited by] Vimlesh Seth, SK. Essentials of tuberculosis in children. New Delhi: Jaypee Bros. 2006; (3rd ed): Medical Publishers. PubMed | Google Scholar
- World Health Organization. Group of risk. WHO global tuberculosis report. 2012. PubMed | Google Scholar
- World Health Organization. Epidemiology. Global tuberculosis control: epidemiology, strategy, financing mates of TB burden. 2009; 6-33. PubMed | Google Scholar
- Skolnik Richard. Global health 101. Jones & Bartlett Learning. 2011; (2nd ed): Burlington, MA. PubMed | Google Scholar
- Birn Anne-Emanuelle, Pillay Y, Holtz Timothy H. Textbook of International Health: Global Health in a Dynamic World. 2009; 3rd edition: Oxford University Press. Google Scholar
- Kumar V, Abbas AK, Fausto N, Mitchell RN. Robbins Basic Pathology. Saunders Elsevier. 2007; 8th ed. PubMed | Google Scholar
- Brennan Patrick J, Nikaido Hiroshi. The envelope of mycobacteria. Annu Rev Biochem. 1995; 64: 29-63. PubMed | Google Scholar
- Lawn Stephen D, Zumla AI. Tuberculosis. Lancet. 2011; 378 (9785): 57-72. PubMed | Google Scholar
- Menzies Dick, Al Jahdali H, Al Otaibi Badriah. Recent developments in treatment of latent tuberculosis infection. The Indian journal of medical research. 2011; 133 (3): 257-66. PubMed | Google Scholar
- Tsaku Isaac Mary, Akyala Ishaku, Amuta EU. A retrospective study on the mortality rate of Human Immunodeficiency Virus (Hiv) And pulmonary tuberculosis (PTB) co-infected individuals in Nasarawa State, Nigeria. Journal of Biology, Agriculture and Healthcare. 2011; 3(7): 218-224. PubMed | Google Scholar
- Iliyasu Zubairu, Babashani M. Prevalence and Predictors of TB coinfection Among HIV seropositive patients attending Aminu Kano Teaching Hospital, Northern Nigeria. J Epidemiol. 2009; 19(2):81-87. PubMed | Google Scholar
- Maori Lynn . Prevalence of Tuberculosis among HIV/AIDS Patients Attending Zambuk General Hospital. NY Sci J. 2012; 5(5):33-36. PubMed | Google Scholar
- Nwobu G Obiora, Okodua MA, Tatfeng Y Mirabeau. Comparative study of HIV Associated Pulmonary Tuberculosis in Chest Clinics from Two Regions of Edo State, Nigeria. Online J Hlth Allied Scs. 2004; 3: 4. PubMed | Google Scholar
- Onubogu CC, Kunle-Ope CN, Onyejepu N, Nwokoye NN, Raheem TY, Igbasi UT, Tochukwu NE, Omoleye RM, Ejezie CO, Musa AZ, Odunukwe NN, Onwujekwe DI and Idigbe EO. Prevalence of Tuberculosis and Human Immune deficiency Virus (TB/HIV) Co-infection amongst patients with broncho pulmonary disorders in Lagos. African Journal of Microbiology Research. 2010; 4(18): 1904-1908. PubMed | Google Scholar
- Pym S Alexander, Domenech P, Honore N, Song J, Deretic V, Cole T Stewart. Regulation of catalase- peroxidase (KatG) expression, isoniazid sensitivity and virulence by furA of Mycobacterium tuberculosis. Mol Microbiol. 2001; 40:879-889. PubMed | Google Scholar
- O'Brien Richard J. Drug- resistant tuberculosis: etiology, management and prevention. Semin Respir Infect. 1994; 9 (2): 104-112. PubMed | Google Scholar
- Volmink Jimmy, Garner P. Directly observed therapy for treating tuberculosis, In Volmink Jimmy. Cochrane Database Syst Rev. 2007; (4): CD003343. PubMed | Google Scholar