Multiple paraneoplastic syndromes revealing non-small cell lung carcinoma
Monia Youssef, Melek Kechida, Saoussen Cheikhmohamed, Adnene Moussa, Jameleddine Zili
Corresponding author: Youssef Monia, Dermatology Department Fattouma Bourguiba Hospital 5000 Monastir, Tunisia 
Received: 18 Apr 2014 - Accepted: 07 Oct 2014 - Published: 03 Nov 2014
Domain: Clinical medicine
Keywords: Carcinoma, paraneoplastic dermatoses, IgE
©Monia Youssef et al. Pan African Medical Journal (ISSN: 1937-8688). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Monia Youssef et al. Multiple paraneoplastic syndromes revealing non-small cell lung carcinoma. Pan African Medical Journal. 2014;19:237. [doi: 10.11604/pamj.2014.19.237.4409]
Available online at: https://www.panafrican-med-journal.com//content/article/19/237/full
Multiple paraneoplastic syndromes revealing non-small cell lung carcinoma
Monia Youssef1,&, Melek Kechida1, Saoussen Cheikhmohamed2, Adnene Moussa3, Jameleddine
1Dermatology Departement, Fattouma Bourguiba Hospital Monastir, Tunisia, 2Pneumology Departement, Fattouma Bourguiba Hospital Monastir, Tunisia, 3Anatomo-Pathology Departement, Fattouma Bourguiba Hospital Monastir, Tunisia
&Corresponding author
Youssef Monia, Dermatology Department Fattouma Bourguiba Hospital 5000 Monastir, Tunisia
A broad spectrum of paraneoplastic dermatoses is associated with lung cancer. We report herein a 56-year-old man who presented an association of erythroderma, acquired ichthyosis, palmo-plantar keratoderma, hypereosinophilia and hyper IgE. In light of these clinical and biological assessments an underlying malignancy had been suspected. A thoracic, abdominal and pelvic computed tomography showed a left hilar mass. The patient underwent a left pneumonectomy and the histological study had confirmed a non-small cell lung cancer. Recognition of cutaneous paraneoplastic syndromes is important since it leads to prompt diagnosis of an underlying malignancy and consequently a better management and prognosis of the disease.
Cutaneous paraneoplastic syndromes are a large group of dermatoses that may be associated with an internal malignancy. A broad spectrum of paraneoplastic dermatoses is associated with lung cancer. We report herein the case of patient who presented an association of erythroderma, acquired ichthyosis, palmo-plantar keratoderma, hypereosinophilia and hyper IgE that revealed a non-small-cell lung carcinoma (NSCLC).
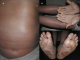
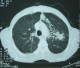
A 56-year-old man was admitted to our dermatology department on November 2011 for the onset of a three-month history of erythroderma associated with weight loss, asthenia and chronic diarrhea. He was a heavy smoker, with no past medical history. The physical examination on admission revealed generalized itchy, erythematous and scaling lesions on the face, trunk, and extremities predominantly on the extensor surfaces, associated with palmo-plantar keratoderma (Figure 1). The biological assessment revealed a biological inflammatory syndrome with an accelerated erythrocyte sedimentation rate at 85 mm, hypergammaglobulinemia at 16g/l, inflammatory anemia at 8.9 g/dl with hypereosinophilia ranging from 2500 to 3600 E/mm3 and hyper IgE serum level reaching 13932 U/ml . Cutaneous biopsies showed focal acanthosis and focal parakeratosis, hypogranulosis, with mild dermal perivascular infiltrate consisting mainly of lymphocytes and some eosinophils. Tumor markers showed only mildly elevated carcinoembryogenic antigen (CEA). A thoracic, abdominal and pelvic computed tomography showed a left hilar mass of 6 cm with micronodules of the left upper lobe without any other metastatic lesions (Figure 2). A stenotic infiltration of the culmen was found on the bronchial fibroscopy. The biopsy of this infiltration showed a bronchogenic epidermoid carcinoma. This diagnosis was confirmed by the histological analysis when the patient underwent a left pneumonectomy. The clinical course was characterized by a complete healing of the cutaneous lesions and a regression of the hyper eosinophilia and IgE. One year later the patient died due to the recurrence of his cancer.
Our case highlights the association of multiple paraneoplastic syndromes: transient erythroderma, acquired ichthyosis, palmo-plantar keratoderma, hyper eosinophilia and hyper IgE. The parallel course of the carcinoma, the cutaneous lesions and these hyper IgE and eosinophilia strongly supports paraneoplastic phenomenon. Erythroderma may be a cutaneous manifestation of malignancy. Its association with internal malignancy is approximately 1% [1]. Acquired ichthyosis (AI) is associated with malignancy in nearly half of the cases. One-third of the reported cancers were related to Hodgkin�s disease. Reported solid tumors associated with AI are breast, bronchial, laryngeal, esophageal, gastric bladder, transitional cell carcinoma of kidney, cervix and ovarian cancer [2].
�
Association of AI to other cutaneous paraneoplastic syndromes is rare. Some isolated cases of association have been reported in literature with erythroderma that evolved to erythema gyratum repens [3], bazex paraneoplastic acrokeratosis, addisonian pigmentation and dermatomyositis [4]. Association of lung carcinoma with paraneoplastic cutaneous manifestations has been widely reported in literature. A Pub Med literature search on cutaneous paraneoplastic manifestations associated with NSCLC from 1970 to February 2014 showed that there is no specific paraneoplastic dermatosis associated with this type of lung cancer. This latter is most commonly associated with neurologic, rheumatic and endocrine paraneoplastic syndromes. Clubbing and hypertrophic osteoarthropathy occurs in 1-5 % of all patients with NSCLC and is considered as the most reported paraneoplastic dermatosis [5, 6] but it is not specific to NSCLC.
We consider our case to be original because, to our knowledge, it is the first report in literature invoking the association of acquired ichthyosis with NSCLC, and also reporting a myriad of paraneoplastic cutaneous and hematologic syndromes revealing a NSCLC.
The authors declare no competing interest.
All authors contributed in this work. All authors have read and agreed to the final version of this manuscript and have equally contributed to its content and to the management of the case.
Figure 1: (A) erythematous and finely scaling lesions on the trunk; (B, C) palmo-plantar keratoderma
Figure 2: the scanographic aspect of the left hilar mass
- Chakraborty. Lymphoma as a cause of exfoliative dermatitis. Indian J Dermatol. 1983; 28(3):121-3. PubMed | Google Scholar
- Levy O, Tishler M. Acquired ichthyosis as the primary manifestation of renal cell carcinoma. Isr Med Assoc J. 2009; 11(2):121. PubMed | Google Scholar
- Penven K, Verneuil L, Dompmartin A, et al. An association of paraneoplastic syndromes in a patient. Ann Dermatol Venereol. 2002; 129(8-9): 1042-5. PubMed | Google Scholar
- Dar NR, Raza N, Khan A, Amin MU. Paraneoplastic Addisonian pigmentation and acquired ichthyosis as presenting features of multiple myeloma. J Coll Physicians Surg Pak. 2011; 21(1): 40-2. PubMed | Google Scholar
- Ito T, Goto K, Yoh K, et al. Hypertrophic pulmonary osteoarthropathy as a paraneoplastic manifestation of lung cancer. J Thorac Oncol. 2010; 5(7):976-80. PubMed | Google Scholar
- Lommatzsch M, Julius P, L�ck W, et al. Hypertrophic pulmonary osteoarthropathy as a cue for NSCLC: four cases in the light of the current literature. Pneumologie. 2012; 66(2):67-73. PubMed | Google Scholar