A rare third ventricle solitary tuberculoma
Hermann Adonis N’da, Adéréhime Haidara, Landry Drogba, Louis Kéhableon Derou, Konan Serges Yao, Vincent Ba Zézé
Corresponding author: N’da Hermann Adonis, Service de Neurochirurgie, Chu de Yopougon Abidjan, Côte D’Ivoire 
Received: 10 May 2013 - Accepted: 16 Jul 2013 - Published: 04 Sep 2013
Domain: Other
Keywords: Intraventricular Tuberculoma, third ventricle, tuberculoma
©Hermann Adonis N’da et al. Pan African Medical Journal (ISSN: 1937-8688). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Hermann Adonis N’da et al. A rare third ventricle solitary tuberculoma. Pan African Medical Journal. 2013;16:5. [doi: 10.11604/pamj.2013.16.5.2815]
Available online at: https://www.panafrican-med-journal.com//content/article/16/5/full
A Rare third ventricle solitary tuberculoma
Hermann Adonis N’da1,&, Adéréhime Haidara1, Landry Drogba1, Louis Kéhableon Derou1, Serges Konan Yao1, Vincent Ba Zézé1
1Service de Neurochirurgie, Chu de Yopougon Abidjan, Côte D’Ivoire
&Corresponding author
N’da Hermann Adonis, Service de Neurochirurgie, Chu de Yopougon Abidjan, Côte D’Ivoire
The localization of the tuberculoma at the third ventricle is rare. The authors report a case of third ventricle solitary Tuberculoma which has occurred in a 10 year old patient and revealed by a syndrome of intracranial hypertension without tuberculosis stigma. This lesion appears clinically and radiologically as a primary brain tumor. A total removal using a subchoroidal approach to the third ventricle has been performed. Histological examination showed a tuberculous like granuloma. An adjuvant antituberculous chemotherapy practiced for 6 months brought the complete cure. The authors insist on the diagnostic and therapeutic difficulties in front of a third ventricle solitary tuberculoma.
Tuberculosis continues to be a public health problem in under developed world. Tuberculoma's rate in all intracranial space occupying lesions is variable according to countries and series [1], 15.9% for Arsenjo et al in Chile, 7.3% for Arseni et al in Romania; 12.5% for Odeku et al in Nigeria. The absence of clinical sign specific to the third ventricle tuberculoma makes the diagnosis difficult to establish apart from any tuberculous mark [2,3]. Therapeutic management seems to be also difficult because of no veritable consensus on the treatment duration of this rare extra pulmonary form. This present report illustrates a rare case of tuberculoma which has mimed a primary intraventricular tumor and insist on diagnostic and therapeutic management difficulties.
A ten year old female has been allowed in hospitalization for intense frontal headaches. Theses headaches were associated to a progressive loss of the vision and to tonic seizure of the lowers members. These clinical signs had evolved for four (4) months. The neurological examination was normal. The examination of the other devices was also normal and there was no fever.
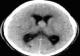
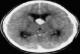
Computed tomography scan (CT Scan) revealed a nodular formation (19 mm high on 16.7 mm wide) in the anterior part of the third ventricle with an obstructive hydrocephalus (Figure 1). This lesion was enhanced by the contrast administration (Figure 2). The likely diagnosis of intraventricular tumor (colloid cyst) was evoked.
A total removal has been performed using a subchoroidal approach. The patient left the hospital 8 days after surgery.
Histological examination revealed the presence of central necrosis surrounded by a tuberculous like granuloma (Figure 3).
A new clinical status of the patient did not show tuberculosis infection stigma, HIV serology was negative. The Tuberculin skin test and the lung radiography were also normal. The confirmation of the tuberculous etiology was obtained by the Polymerase Chain Reaction (PCR). The CSF examination showed only 3 cells (3 lymphocytes) and the bacteriological examination using the ziehl-nielsen staining was negative. Protein level in CSF was normal (0.4g/l). She was treated with antituberculous chemotherapy including Isoniazid, Rifampicin, Pyrazinamid and Ethambutol for six months. The patient is living normally and is following her secondary studies, six (6) years afterwards.
The intraventricular localization of tuberculoma is rare. Primarily, tuberculoma seems to be child and young adults problem [4] because most of time, the patient do not exceed twenty years old.
The diagnostic strategy in front of a tuberculoma can be made of 2 manners. Firstly, the existence of a known or evolutionary bacillary context, having preceded or accompanying the neurological symptomatology, or the discovery of a tuberculous hearth, must firstly evoke the tuberculoma in front of an intracranial expansive process [5, 6].
This bacillary context did not exist in our case. The second case is the pure hypertensive form which appears clinically and radiologically as a brain primary tumor. The Diagnosis of this form is very difficult because of no bacillary context.
Even if neuroimaging can contribute to the diagnosis, it remains very difficult to differentiate the tuberculoma from a cerebral tumor. However, the peripheral catch of contrast, the central necrosis, a disproportionate oedema and the traction on the septum pellucidum are neuroimaging (CT Scan; MRI) features of intraventricular tuberculoma [1, 7].
The traction of the septum pellucidum is a very important radiological feature of tuberculoma because it signs the presence of intraventricular adhesive process [7, 8].
For many authors [4,9-10], an antituberculous chemotherapy has to be establish without necessary biopsy when the diagnosis of tuberculoma is reasonably likely and outside quite intracranial pressure increase.
We have no doubt on efficacy of the antituberculous chemotherapy but in spite of a strong suspicion of tuberculoma, it could be confused with brain primary tumors. Furthermore, exclusive chemotherapy could be long (12 to 18 months) with 3 years extreme for Rossi et al [11]. This kind of duration exposes the patient to the toxicity of antituberculous drugs. We recommend surgical resection or when possible an endoscopy biopsy in front of accessible lesion to firstly diagnosis confirmation.
Complete resection allows reducing in six months the antituberculous treatment duration. According to CT scan evolution of the lesion, this period could be prolonged in 9 months. This is what?s doing for extra pulmonary form (intracranial or vertebral location) of tuberculosis in our country, where, tuberculosis is an endemic disease.
The third ventricle location of tuberculoma is rare. The diagnosis of the pure hypertensive form is very difficult and very often presumptive.
Surgery is recommended to confirm the diagnosis and to reduce chemotherapy duration and toxicity. For these reasons complete resection via open surgery or endoscopic surgery of this lesion when it is possible is desirable.
Authors declared they have on conflict of interest.
All the authors contributed to the study. All the authors have read and approved the final version of the manuscript.
Figure 1: CT scan with an isodense nodular formation in the anterior part of third ventricle
Figure 2: CT scan with contrast administration
Figure 3: Haematoxylin Eosin (HE) × 100, Tuberculous granuloma with giants cells and caseous necrosis
- Singh JP, Chandy MJ. Third ventricular Tuberculoma: case report. Br J Neurosurg. 1988; 2(1): 93-96. PubMed | Google Scholar
- Choudoury AR. Non surgical treatment of Tuberculomas of the brain. Br J Neurosurg. 1989; 3(6): 643-53. PubMed | Google Scholar
- Delaporte P, Salama J, Amarenco P. Subthalamic tuberculoma disclosed by hemiballism: Efficacy of antituberculous treatement. Ann Med interne. 1983; 134(8):728-31. PubMed | Google Scholar
- Naim-ur-rahman. Intracranial Tuberculoma : diagnosis and management. Acta Neurochir. 1987; 88(3-4): 109-15. PubMed | Google Scholar
- Desgeorges M, Tranier J, Mercier PH et al. Tuberculome cérébral intraventriculaire ŕ propos d?un cas. Ann Med interne. 1977; 128:541-544. PubMed | Google Scholar
- Desai K, Nadkarni T, Bhatjiwale M, et al. Intraventricular tuberculomas. Neurol Med Chir. 2002; 42(11):501-503. PubMed | Google Scholar
- Berthier M, Sierra J, Leiguarda R. Intraventricular tuberculoma: Report of four cases in children. Neuroradiology. 1987; 29(2): 163-67. PubMed | Google Scholar
- Vajramani GV, Devi BI, Hedge T, et al. Intraventricular tuberculous abscess: A case report. Neurology India. 1999; 47(4): 327-29. PubMed | Google Scholar
- Hirsh LF, Lee SH, Silberstein ST. Intracranial tuberculoma and CT scan. Acta Neurochir. 1978; 45(1-2): 155-61. PubMed | Google Scholar
- Tandon PN, Bhargava S. Effect of medical treatement on intracranial tuberculoma: a CT study. Tubercle. 1985; 66(2): 85-87. PubMed | Google Scholar
- Rossi LN, Duzioni N, Terzi F. Intracranial tuberculoma in a child: Regression on CT scan under conservative therapy. Neuropediatrics. 1985; 16(4): 228-30. PubMed | Google Scholar