Ankyloblepharon filiforme adnatum: a case report
Bouchra Alami, Asmae Maadane, Rachid Sekhsoukh
Corresponding author: Bouchra Alami, Ophthalmology department, El Farabi Hospital, Medical School, University Mohammed First, Oujda, Morocco 
Received: 16 Nov 2012 - Accepted: 27 Jan 2013 - Published: 08 May 2013
Domain: Clinical medicine
Keywords: Ankyloblepharon filiforme adnatum, malformation, eyes
©Bouchra Alami et al. Pan African Medical Journal (ISSN: 1937-8688). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Bouchra Alami et al. Ankyloblepharon filiforme adnatum: a case report. Pan African Medical Journal. 2013;15:15. [doi: 10.11604/pamj.2013.15.15.2209]
Available online at: https://www.panafrican-med-journal.com//content/article/15/15/full
Ankyloblepharon filiforme adnatum: a case report
Bouchra Alami1,&, Asmae Maadane1, Rachid Sekhsoukh1
1Ophthalmology Department, El Farabi Hospital, Medical School, University Mohammed First, Oujda, Morocco
&Corresponding author
Bouchra Alami, Ophthalmology department, El Farabi Hospital, Medical School, University Mohammed First, Oujda, Morocco
Ankyloblepharon is defined by partial or complete adhesion of the ciliary edges of superior and inferior eyelids. It is usually a sporadic isolated malformation in which the upper and lower lids are joined by tags. Although it is an uncommon and benign condition, its presence should alert the clinician to the possibility of other important disorders. We report a case of a new born who had a sporadic ankyloblepharon, treated one day after birth.
Ankyloblepharon describes direct fusion of the lids. It is a rare congenital abnormality, in which single or multiple strands of fine connective tissue join the upper and lower lids anywhere along the lid but never at the lateral or medial canthus [1]. These strands are extensible, and by forcibly opening the lids their length can be almost doubled. The tissue invariably arises from the grey line, anterior to the meibomian gland orifices and posterior the cilia.
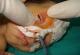
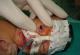
A female neonate was referred for assessment of his right eyelids. She was born at term, to a primigravid mother, weighing 3400 g. Pregnancy and delivery were unremarkable. There was no family history of congenital anomalies or consanguinity. The baby was noted to have fused right eyelids at birth; apart from this, she was perfectly healthy. A detailed pediatric assessment failed to reveal any other congenital abnormalities. Ocular examination showed partial fusion of his right upper and lower eyelids by a central narrow band of tissue, arising from the grey lines (Figure 1). Full eyelid opening was impaired and interpalpebral aperture was limited to 3.5 mm. Right eye examination was normal. The band of tissue was excised with Vannas scissors at the level of each eyelid margin (Figure 2). The procedure was performed under sedation. There was a limited bleeding. Subsequent right eye examination did not reveal any other pathology. At her follow up appointment 5 months later, no abnormality was noted.
Ankyloblepharon filiforme adnatum (AFA) is a rare benign congenital anomaly, first described by Von Hasner in 1881. Fusion of the eyelid margins is a normal stage in human development, but an abnormal occurrence at birth. The developing eyelid margins remain fused until the fifth gestational month, but may not be completely separated until the seventh month. Ankyloblepharon is characterized by full thickness fusion of the lid margins.
AFA describes single or multiple bands of tissue joining the upper and lower eyelids either unilaterally or bilaterally. The histology of these connecting strands has been shown to consist of vascularised central core surrounded by stratifed squamous epithelium [1]. It may present as an isolated congenital defect such as in our patient. However, it is always important to actively look for coexisting pathology.
The ophthalmic association of AFA is iridogoniodysgenesis with juvenile glaucoma [2]. It has been reported in the context of trisomy 18 (Edwards� syndrome) [3], Hay-Wells syndrome (a variant of the ectodactyly-ectodermal dysplasia-cleft lip palate syndrome) [4,5], the popliteal pterygium syndrome (characterized by intercrural webbing of the lower limbs), and CHANDS (curly hair-ankyloblepharon-nail dysplasia syndrome). Other associations may include hydrocephalus, meningocele, an imperforate anus, bilateral syndactyly, infantile glaucoma and cardiac problems such as patent ductus arteriosus and ventricular septal defects [6].
Detailed systemic assessment by an experienced pediatrician is therefore imperative in the management of AFA.
Rosenman et al [7,8] divide AFA into four subgroups (Table 1) and indicated that groups I and II were sporadic and groups III and IV were autosomal dominant with variable expressivity. Bacal et al [3] suggested a fifth group: AFA in association with chromosomal abnormalities.
The aetiology of this abnormality is unknown and a number of theories have been proposed. The currently accepted theory is that this condition is due to an interplay of temporary epithelial arrest and rapid mesenchymal proliferation, allowing union of lids at abnormal positions [5].
This case report demonstrates the simplicity in treating AFA. Surgical correction should be performed promptly to minimize any risk of amblyopia, and enable full examination of the eye. It also highlights that its presence should alert the clinician to the possibility of an underlying congenital disorder.
Ankyloblepharon filiforme adnatum is a rare but potentially amblyogenic congenital abnormality of the eyelids. Treatment should be performed to minimize the risk of amblyopia.
The authors declare that they have no competing interests.
All the authors contributed in the case management, BA made the case report. All authors read and approved the final manuscript.
Table 1: Classification of ankyloblepharon filiforme adnatum
Figure 1: Photograph of the neonate with ankyloblepharon filiforme adnatum showing partial fusion of the right upper and lower eyelids by a band of tissue
Figure 2: Right eye immediately after adhesion separation
- Judge H, Mott W, Gabriels J. Ankyloblepharon filiforme adnatum. Arch Ophthalmol. 1929; 2: 702-8. PubMed | Google Scholar
- Scott MH, Richard JM, Farris BK. Ankyloblepharon filiforme adnatum associated with infantile glaucoma and iridogoniodysgenesis. J Pediatr Ophthalmol Strabismus. 1994 Mar-Apr;31(2):93-5. PubMed | Google Scholar
- Bacal DA, Nelson LB, Zackai EH, Lavrich JB, Kousseff BG, McDonald-McGinn D. Ankyloblepharon filiforme adnatum in trisomy 18. J Pediatr Ophthalmol Strabismus. 1993 Sep-Oct;30(5):337-9. PubMed | Google Scholar
- Long JC, Blandford SE. Ankyloblepharon filiforme adnatum with cleft lip and palate. Am J Ophthalmol. 1962 Jan;53:126-9. PubMed | Google Scholar
- Vanderhooft SL, Stephan MJ, Sybert VP. Severe skin erosions and scalp infections in AEC syndrome. Pediatr Dermatol. 1993 Dec;10(4):334-40. PubMed | Google Scholar
- Anna Maria Gruener, Manjit S Mehat. A newborn with ankyloblepharon filiforme adnatum: a case report. Cases J. 2009 Aug 14;2:8146. PubMed | Google Scholar
- Amusini P, Bruel H, Chabrolle JP et al. Ankylobl�pharon filiforme adnatum. Arch P�diatr. 2000; 7: 1009-13. PubMed | Google Scholar
- Rosenman Y, Ronen S, Eidelman AI, Schimmel MS. Ankyloblepharon filiforme adnatum: congenital eyelid-band syndromes. Am J Dis Child. 1980 Aug;134(8):751-3. PubMed | Google Scholar