Prognosis of tetanus patients in the intensive care unit of Provincial Hospital Jason Sendwe, Lubumbashi, DR Congo
Michel Manika Muteya, Alain Kabey a Kabey, Théophile Muyumba Lubanga, Henri Mundongo Tshamba, Albert Mwembo Tambwe A Nkoy
Corresponding author: Michel Manika Muteya, Department of anesthesiology-intensive care, Cliniques Universitaires de Lubumbashi, University of Lubumbashi, B P 1825, R.D.Congo 
Received: 07 Nov 2012 - Accepted: 13 Feb 2013 - Published: 10 Mar 2013
Domain: Clinical medicine
Keywords: Tetanus, prognosis, mortality, Lubumbashi
©Michel Manika Muteya et al. Pan African Medical Journal (ISSN: 1937-8688). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Michel Manika Muteya et al. Prognosis of tetanus patients in the intensive care unit of Provincial Hospital Jason Sendwe, Lubumbashi, DR Congo. Pan African Medical Journal. 2013;14:93. [doi: 10.11604/pamj.2013.14.93.2180]
Available online at: https://www.panafrican-med-journal.com//content/article/14/93/full
Original article 
Prognosis of tetanus patients in the intensive care unit of Provincial Hospital Jason Sendwe, Lubumbashi, DR Congo
Prognosis of tetanus patients in the intensive care unit of Provincial Hospital Jason Sendwe, Lubumbashi, DR Congo
Michel Manika Muteya1,&, Alain Kabey a Kabey1, Théophile Muyumba Lubanga1, Henri Mundongo Tshamba2, Albert Mwembo Tambwe a Nkoy2
1Department of anesthesiology-intensive care, Cliniques Universitaires de Lubumbashi, University of Lubumbashi, B P 1825, R.D.Congo, 2School of Public Health, University of Lubumbashi, BP 1825, DR Congo.
&Corresponding author
Michel Manika Muteya, Department of anesthesiology-intensive care, Cliniques Universitaires de Lubumbashi, University of Lubumbashi, B P 1825, DR Congo
Tetanus is still a public health problem in developing countries including the Democratic Republic of Congo. The objective of this study was to determine the prognosis of patients with tetanus admitted in the Intensive Care Unit (ICU) of Provincial Hospital Jason Sendwe, Lubumbashi, DR Congo. This is a descriptive study which collected information from registers and medical records of patients admitted for tetanus in the ICU of Jason Sendwe Hospital, between January 2005 and December 2009. We calculated the parameters of position, dispersion as well as frequencies. We used the test of independent association of prognosis (death versus survival). Tetanus constituted 2.1% of admissions in the ICU during the 5-year period. The average age of patients was 39.38 ± 17; majority of patients were males (95.5%). The majority of patients lived the townships of Kampemba (27.3%), Kenya (22.7%), and Annexe (18.2%). All patients presented the generalized form of the infection. The door of entry was detectable in 71.5% of cases, localized mainly to the lower limbs (61.9%). The average length of stay was 11.29 ± 11.39 days. Mortality was observed in 52.4% of cases. This mortality was statistically significant in patients aged more than 40 years (p = 0.029) but not not related to the length of stay (p=0.080) nor the location of point of entry(p=0.28). In our environment the prognosis of tetanus remains severe. This disease is still frequent in the city of Lubumbashi; sensibilisation of population on preventive strategeis as well as setting up appropriate structures for better management of cases are required.
Tetanus is a toxic infection characterized by a spasm of skeletal muscles that often evolves progressively toward respiratory failure [1]. It is a devastating disease associated with autonomic instability and a high incidence of mortality [2]. Tetanus is caused by Clostridium tetani, a bacterium that infects open wounds such as lacerations and penetrating wounds. Older people, women and children are prone to injuries and therefore Clostridium tetani at high risk of the disease. The incubation period of the disease varies from 2 to 50 days [2-5]. As there is no specific laboratory test for tetanus, the diagnosis is based on history and clinical signs [6].
WHO and some authors estimate that between five hundred thousand to one million cases of tetanus occur every year worldwide, with 50% to 70% mortality in some regions [3,7]. The disease has become rare in developed countries mainly due to vaccination programs childhood to adulthood as well as measures of sterilization and aseptic technique [4,8,9]. Even in those countries when it is diagnosed, it remains a serious and deadly disease despite the progress of medicine and adequate resuscitation [10].
Although this disease is easily preventable with a highly effective vaccine, tetanus is still common and remains a public health problem; with high mortality in both adults and newborns in almost all developing countries, including the Democratic Republic of Congo [2,4,8,11], years after the introduction of vaccination through the Expanded Program on Immunization.
Lubumbashi is the second politico-administrative city and the more populated city of the Democratic Republic of Congo after Kinshasa. It is divided administratively into seven townships: Annexe, Kamalondo, Kampemba, Katuba, Kenya, Lubumbashi and Ruashi. It counts several health facilities including the Academic Clinics of Lubumbashi, the provincial hospital Janson Sendwe, hospitals of big companies and more referal health centers corresponding to the townships [12].
People affected by tetanus are most often referred to hospital Jason Sendwe because of the availability of anesthetist-resuscitator doctors. The objective of this study was to to determine the prognosis of tetanus in intensive care unit of the provincial hospital Jason Sendwe.
Type and period of study
This is a descriptive study with data coming from the analysis of medical records of patients admitted for tetanus in the intensive care unit of the Provincial Hospital of Jason Sendwe of Lubumbashi over a five years period from January 1st 2005 to December 31st 2009.
Sampling
It is a exhaustive sampling of all patients admitted for tetanus in ICU. The sample size consisted of 22 patients. The diagnosis of tetanus was based on the presence of at least two signs with or without visible entry door, with or without trismus, sardonic laughing, and rigidity of the abdominal wall and / or neck, in the end by reflex spasm spontaneous or induced by different stimuli. Socio-demographic and clinical parameters such as age, sex, place of residence, the presence of the door, the location of the entry door, the presence of a defect (diabetes, HIV), duration of hospitalization (from day of admission) and outcome (survival or death) were studied.
Data collection and analysis
Data were collected from registers and patients' records. Data were encoded using Epi Info ® Version 3.5.1 and Excel 2007 and analysed to derive means, standard deviations and frequencies. Fischer's chi-square was used to assess the association with other outcome variables (age, living, entry door) with a significance level of p <0.05
Incidence of tetanus
One thousand and twenty-nine (1029) patients were admitted to the ICU of the provincial hospital Jason Sendwe of Lubumbashi between January 2005 and December 2009. Of these, twenty-two (22) cases of tetanus were reported, representing a prevalence of 2.1%. All patients had the generalized form of infection on admission. Medical records could be retrieved for 21 of the 22. The vaccination status of patients was not known.
Age and sex
The average age of patients was 39, 38 ± 17.79 with a range from 5 to 77 years. 57.2% belong to the 30-50-year age-group; 52.1% of all patients were were younger than 40 years. There were 95.2% of male patients and only 4.7% female (Table 1).
Municipality of residence
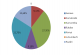
Figure 1 shows that 27.3% of the patients came from Kampemba town, 22.7% from the municipality of Kenya and 18.2% from Annexe. No patient did come from the center of the city of Lubumbashi.
Prognostic factors
The majority of patients had detectable point of entry (71.5%) while the point of entry was not detectable in 28.5% of cases. In 61.9% of cases the location of entry was the lower limbs against 4 8% for the upper limbs; in 4.8% of cases, the point of entry was a result of circumcision.
Only one patient was diabetic (4.5%). All patients were treated with diazepam, metronidazole or penicillin and intravenous antitoxin, all this combined with debridement of the wound and general measures of nursing. The average length of hospitalization was 11.29 ± 11.39 days with a range of 1 to 47 days. A mortality of 52.4% was recorded; 47.6% of the patients survived; one patient was discharged from the hospital against medical advice. Mortality was higher in patients aged more than 40 years (P = 0.029). The majority of patients who died (81.8%) have a average length of stay of 10 days. Mortality was not influenced by the duration of hospitalization (P = 0.80 or the location of the point of entry (Table 2).
Our study focused on tetanus cases admitted in the ICU of the provincial hospital Jason Sendwe, other cases of tetanus treated in other hospital departments including, medicine, surgery, pediatrics and neuropsychiatry were not included.
Tetanus accounted for 2.1% of all admissions to the ICU for a period of 5 years, from January 2005 to December 2009. This proportion is slightly higher than what has been found by Onwudukwa et al, in Nigeria in a university hospital where a prevalence of 1, 36% over a similar period was reported [13]. In reality, this prevalence would be greater if the study was extended throughout the hospital, this was the case in Senegal where, Soumaré et al, found a hospital prevalence of 5.3% [7]. Other cases of tetanus in the city will go unnoticed by because of limited access to health care due to ignorance and poverty of the population. According to WHO, the DRC has an average of 1023.265 tetanus cases reported per year including an average of 764.33 neonatal tetanus per year nationaly [14]. This is much higher than in Canada, where 4 cases of tetanus are reported per year, in the United States with 12-15 cases per year, in France with 18 cases per year and in the United Kingdom with 50-60 cases per year [8]. The high prevalence of tetanus in the DRC and in other developing countries can be explained by ignorance, lack of personal hygiene, lack of easy access to primary health care due to poverty and inefficiency of the vaccination program. The majority of patients in this study were male (90.5%) belonging to the age group of 30-50 years. A similar result was reported by Tendesse et al. in Ethiopia [9], Amisi et al. in Kinshasa [12] and Mabula et al. in Tanzania [5]. Simply because they are young adults who are part of the population economically active and and at higher risk of injury. Regarding sex again, the higher proportion of men can be explained by the fact that men are more active handicrafts and exposed to injury and are susceptible to infection, and women are immune due to routine vaccination during pregnancy [4,15]. Overcrowding, lack of hygiene, ignorance and poor living conditions can explain why the majority of patients are common residents of the largest and most populated and urbanized cities of Lubumbashi: Annexe, Kampemba and Kenya.
On the location of the point of entry, it was detectable in 71.5% of cases and more localized to the lower limbs (61.9%) as is the case in most of the literature on tetanus through the world [4,9,12]. This can be explained by the lack of adequate protection (shoes), personal hygiene of patients and once again, ignorance regarding the maintenance of personal health, and poverty.
In our series the mortality was observed in 52, 4% of cases, with a high prevalence in people over 40 years of age. A higher mortality rate was reported by Fawib in Nigeria (57.1%), Ndour et al. in Senegal (60.8%), Mabula et al. in Tanzania (72.7%) and Ilardo et al. in Argentina (75%) [16-19]. By cons, our mortality was relatively higher than what was found in Nigeria, Ethiopia, Senegal and Albania [7,9,13,20,21]. Decreased immunity from 40 years of age may explain why the disease is more prevalent and the mortality higher in this age group in our study; this finding was corroborated by other authors [12]. High mortality in our study as reported in other similar studies mentioned above, can be explained by the precarious living conditions of the population which does not allow easy access to primary health care, lack of adequate resuscitation equipment (laryngoscope, ventilator, monitor, etc). Beyond all these financial barriers people; the health seeking behavior of the population can contribute to the higher mortality; in most cases, patients will seek treatment from traditional healers before coming to hospital, often late; in hospitals, the limited experience of staff in managinng cases of tetanus can contribute to a higher mortality.
In our study, tetanus patients represent 2.1% of all admissions ICU patients, predominantly male (95.5%). The mortality rate was 52 4%. The prognosis is generally influenced by the patient's age and the time between injury and medical care. We recommend a vaccination policy from childhood to adulthood by regular booster vaccinations in young adults. Adequate structures, well equipped with resuscitation equipments are needed for better management of patients. Finally awareness capmpaigns should be conducted for appropriate and timely management of wounds at health facility level, health facility staff should also be capacitated for the appropriate diagnosis and management as well as early transfer to ICU.
The authors declare no competing interests.
All authors participated in the preparation of this manuscript and have read and approved the final version.
Table 1: Distribution of illnesses according to age and the sex.
Table 2 Distribution of the patients according to the factors prognoses
Figure 1: Distribution of the patients according to the township of residence
- Alagappan K, Alagappan K, McGowan J, DeClaro D, Ng D, Silverman R A. Tetanus antibody protection among HIV-infected Us-borne patient and immigrant. Int J Emerg Med. 2008; 1:123-6. PubMed | Google Scholar
- Sutiono AB, Qiantori A, Suwa H, Ohta T. Characteristic tetanus infection in disaster-affected areas: case study of the Yogyakarta earthquakes in Indonesia. BMC Research Notes. 2009; 2:34. PubMed | Google Scholar
- Bhatia. R, Prabhkar S, Grover V K. Tetanus: review. Neurology India. Dec. 2002; 50(4):398-407. PubMed | Google Scholar
- Ogunrin O A. tetanus ? a review of current concepts in management. Journal of Postgraduate Medicine. December 2009; 11(1): 46-60. PubMed | Google Scholar
- Vrushali Ponde. Tetanus: Anaesthetic Management. Indian Journal of Anaesthesia. 2009; 53(3):367-8. PubMed | Google Scholar
- Menelaos Karanikolas et al, Prolonged high-dose intravenous magnesium therapy for severe tetanus in the intensive care unit: a case series. Journal of Medical Case Reports 2010, 4:100. Google Scholar
- Soumaré M et al. Aspects épidémiologiques, cliniques et pronostiques du tétanos juvénile ŕ Dakar, Sénégal. Bull Soc Pathol Exot. 2005; 98 (5): 371-3. PubMed | Google Scholar
- Gibson K et al. Tetanus in developing countries: a case series and review. Can J Anesth/J Can Anesth. 2009; 56:307-15. PubMed | Google Scholar
- Tadesse A, Gebre-Seassie S. Five years review of cases of adult tetanus managed at Gondar University Hospital, North West Ethiopia (Gondar, Sep 2003-Aug 2008). Ethiop Med J . 2009 Oct; 47(4) 209-17. PubMed | Google Scholar
- Mangile L D, Sassi F C, Des Santes Sdes. Oral Sensorimotor function for feeding of patient with tetanus. Acta tropica, Sept 2009; 111(3):316-20. Google Scholar
- Amisi E et al. Prise en charge du tétanos en réanimation aux Cliniques Universitaires de Kinshasa : résultats des 10 ans. Congo Médical. Sept 2003; 11: 970-96. PubMed | Google Scholar
- N?sami Mabiala. Carte sur la croissance de la ville de Lubumbashi. Unilu, Observatoire du changement urbain. 2002. PubMed | Google Scholar
- Onwuchekwa Arthur Chukwubike, Asekomeh Eshiofe God?spower. A 10-year review of outcome of management of tetanus in adults at a Nigerian tertiary hospital. Annals of African Medicine. 2009; 8(3):168-72. PubMed | Google Scholar
- www.who.int/immunisation_monitoting/globalsummury/timeseries/TSincidencebycountry. accédé le 30 aout 2010. PubMed | Google Scholar
- Dao S et al. Tétanos en milieu hospitalier ŕ Bamako, Mali. Méd Trop. 2009 ; 69: 485-7. PubMed | Google Scholar
- Mabula D Mchembe and Victor Mwafongo. Tetanus and its treatment outcome in Dar es Salaam: need for male vaccination. East African Journal of Public Health. October 2005; 2(2): 22-3. PubMed | Google Scholar
- Fawibe AE. The pattern and outcome of adult tetanus at a sub-urban tertiary hospital in Nigeria. J Coll physician Surg Pak. Jan 2010; 1:68-70. PubMed | Google Scholar
- Ndour CT. Tetanus following intramuscular injection in Dakar: epidemiological, clinical and prognostic features. Dakar Med. 2005; 50(3):160-3. PubMed | Google Scholar
- Ilardo R, Frassone NE. Tetanus: Clinical and epidemiological characteristics. Review of 11 years. International Journal of Infectious Diseases. March 2010; 14 (suppl 1) 335-478. PubMed | Google Scholar
- Seydi M, Soumare M, Sow PS, Diop BM, Ndour CT et al. Tetanus: epidemiological aspects at the Infectious Disease Clinics at the Fann University Hospital Center in Dakar. Dakar Med. 2000; 45(1):5-7. PubMed | Google Scholar
- Pilaca A, Ndreu A, Byrazeri G, Shytaj K. Assessment of prognosis of tetanus and its related factors among Albanian adults. 20th European Congress of Clinical Microbiology and Infectious Diseases, Vienna, Austria. 10 - 13 April 2010. Google Scholar