Spontaneous transverse colon volvulus
Landolsi Sana, Gassara Ali, Helmi Kallel, Baklouti Amine, Saadaoui Ahmed, ElOuer Mohamed Ali, Chaeib Wajdi, Mannaď Saber
Corresponding author: Landolsi Sana, Department of general surgery, Jendouba’s Hospital, Tunisia 
Received: 22 Sep 2012 - Accepted: 20 Apr 2013 - Published: 25 Apr 2013
Domain: Clinical medicine
Keywords: Volvulus, Transverse colon, spontaneous
©Landolsi Sana et al. Pan African Medical Journal (ISSN: 1937-8688). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Landolsi Sana et al. Spontaneous transverse colon volvulus. Pan African Medical Journal. 2013;14:160. [doi: 10.11604/pamj.2013.14.160.2073]
Available online at: https://www.panafrican-med-journal.com//content/article/14/160/full
Spontaneous transverse colon volvulus
Landolsi Sana1,&, Gassara Ali1, Helmi Kallel1, Baklouti Amine1, Saadaoui Ahmed1, ElOuer Mohamed Ali1, Chaeib Wajdi1, Mannaď Saber1
1Department of general surgery, Jendouba’s Hospital, Tunisia
&Corresponding author
Landolsi Sana, Department of general surgery, Jendouba’s Hospital, Tunisia
We report a case of spontaneous transverse colon volvulus in a young healthy woman. It constitutes an unusual case since it occurred in a young healthy woman with a subacute onset and no aetiological factor has been found. Its diagnosis is still challenging. Prompt recognition with emergency intervention constitutes the key to successful outcome.
The transverse colon volvulus is an uncommon cause of bowel obstruction. It constitutes a surgical emergency since it can lead to bowel infarction, peritonitis, and death if not diagnosed at once. We report a case of a spontaneous transverse colon volvulus in a young healthy woman.
A 39-year old woman presented with a three-day history of constipation and progressive abdominal pain without nausea or vomiting. The last bowel movement had been three days ago. There was no significant past medical history especially of chronic constipation, psychiatric disease, neurologic disease, or abdominal surgery. Physical examination revealed a moderate distension of the abdomen without signs of peritonitis. The abdomen was tympanic to percussion. There were no umbilical or groin hernias. Digital rectal examination demonstrated an empty rectal vault without intraluminal masses.
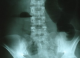
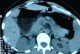
Blood investigations showed normal full blood count, urea, electrolytes, and clotting profile. The abdominal X-ray revealed a large bowel obstruction with a "U-shaped" loop in the left upper abdomen (Figure 1). The computed tomography demonstrated a dilatation of the right colon and the transverse colon with a cut-off near the splenic flexure (Figure 2). No signs of malignancy were found.
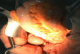
An emergency laparotomy was performed. Intra operative findings (Figure 3) were of a transverse colon volvulus rotated in a three hundred and sixty degrees clockwise direction on its mesentery. The point of twist was found in the left upper quadrant. The bowel was intact without signs of ischemia. A significant disparity in the size of the obstructed proximal and collapsed distal colon to the site of the volvulus was noticed. The transverse colon was mobile and increased in length. The volvulus was delivered into the incision and detorsed. An extended right hemicolectomy was carried on with end-to-side ileo-colic anastomosis.
The postoperative course was uneventful. Discharge from hospital was five days following admission. Histologically, the appearances were consistent with a sub acute progressive transverse colon volvulus. No acute inflammation, infarction, granulomas, dysplasia, malignancy, or vascular abnormality was noticed.
We reported a case of spontaneous transverse colon volvulus in a healthy young woman. She had no past medical history of chronic constipation, psychiatric disease, neurologic disease, or abdominal surgery. Intra operatively, the transverse colon was mobile with an increased length. There was no sign of malignancy.
Only 3 to 5% of all cases of intestinal obstruction are caused by colonic volvulus [1]. Among them, transverse colon is involved in 2 to 4% [2,3] versus 43 to 80% and 15 to 43% respectively for the sigmoid colon and the coecum [3]. A male predominance is noticed [3]. Its pathogenesis is not completely understood yet. Predisposing factors are congenital, physiological, and mechanical [1,4]. The two congenital properties thought to cause a volvulus are redundancy and non-fixation [5] as found in our case. Chagas disease can result in a megacolon increasing colonic length. Physiological causes include high-roughage diet and large bowel distension secondary to chronic constipation. This constipation is associated with psychiatric or neurologic diseases [3]. Mechanical causes include previous volvulus of the transverse or the sigmoid colon, distal colonic obstruction, adhesions, malposition of the colon following previous surgery, mobility of the right colon, inflammatory strictures, and carcinoma [1,4]. Other factors have been reported such as Chilaiditis syndrome [4], Clostridium difficile pseudomembranous colitis [6], and impaired intestinal motility associated with pregnancy.
Our patient presented with subacute transverse volvulus. This progressive onset of the symptoms can delay the diagnosis and the treatment thus resulting in progressing to the acute fulminating type with bowel infraction, peritonitis, and even death [4]. The subacute onset is characterized by massive abdominal distension in the setting of mild abdominal pain without rebound tenderness, nausea, or vomiting [1]. The leukocyte count is normal secondary to the lack of ischemia at early stages. Unlike our case, this type usually occurs in elderly patients affected by several comorbidities and bed-bound. Patients with the acute fulminating type of presentation have a sudden onset of severe abdominal pain, rebound tenderness, vomiting, little distension, and rapid clinical deterioration. Bowel sounds are initially hyperactive becoming absent later on [1, 7].
In our case, the distribution of the large bowel dilatation in abdominal X-ray could have raised the possibility of volvulus since it revealed a "U-shaped" loop with the apex pointing under the left hemidiaphragm. The diagnosis of transverse colon volvulus is difficult because it does not have the same classically recognizable radiographic features as sigmoid and coecal volvulus. It is usually made intra operatively. In the subacute type, the achievement of an early diagnosis through computed tomography is advised [7].
Whereas sigmoid volvulus can be decompressed by colonoscopy, transverse colon volvulus must be surgically detorsed in emergency [4]. Resection constitutes the treatment of choice to prevent recurrence [1,4]. In fact, detorsion alone or associated with colopexy has a higher rate of recurrence than resection [1,4]. The incidence of recurrent volvulus after previous resection and primary anastomosis varies between 22% and 36% [3]. Therefore, some authors recommend considering a subtotal colectomy in the presence of a megacolon, instead of partial resection of the involved bowel segment [3]. This resection is carried on with or without primary anastomosis dependent on the aspect of the colon, the existence or not of peritonitis, and the state of health of the patient. Our patient had an extended right hemicolectomy with a primary anastomosis. The post operative course was uneventful.
Transverse colon volvulus is rare. Its Diagnosis is challenging. Prompt recognition with emergency intervention constitutes the key to successful outcome.
The authors declare no competing interests.
All the authors have contributed to the management of the patient and the write up of the manuscript. All the authors have read and approve the final version of the manuscript.
Figure 1: Abdominal X-rays showing a dilated transverse colon with a “U-shaped” loop in the left upper abdomen.
Figure 2: Computed tomography revealing dilatation of the right colon and the transverse colon with a cut-off near the splenic flexure.
Figure 3: Intra operative view demonstrating transverse colon volvulus. The point of twist was located in the left upper quadrant of the abdomen.
- Sparks D, Dawood M, Chase D, Thomas D. Ischemic volvulus of the transverse colon: A case report and review of literature. Cases J. 2008 Sep 22;1(1):174. PubMed| Google Scholar
- Valsdottir E, Marks JH. Volvulus: Small Bowel and Colon. Clin Colon Rectal Surg. 2008 May;21(2):91-3. PubMed| Google Scholar
- Booij KAC, Tanis PJ, Van Gulik TM, Gouma DJ. Recurrent volvulus of the transverse colon after sigmoid resection. Int J Colorectal Dis. 2009 Apr;24(4):471-2. PubMed| Google Scholar
- Ciraldo A, Thomas D, Schmidt S: A Case Report: Transverse Colon Volvulus Associated With Chilaiditis Syndrome. The Internet Journal of Emergency and Intensive Care Medicine. 2000;4:2. Google Scholar
- Jornet J, Balaguer A, Escribano J, Pagone F, Domenech J, Castello D: Chilaiditi syndrome associated with transverse colon volvulus: First report in a paediatric patient and review of the literature. Eur J Pediatr Surg. 2003; 13:425-428.. Google Scholar
- Yaseen ZH, Watson RE, Dean HA, Wilson ME. Case report: transverse colon volvulus in a patient with Clostridium difficle pseudomembranous colitis. Am J Med Sci. 1994 Oct;308(4):247-50. PubMed| Google Scholar
- Liolios N, Mouravas V, Kepertis C, Patoulias J. Volvulus of the transverse colon in a child: A case report. Eur J Pediatr Surg. 2003 Apr;13(2):140-2. PubMed| Google Scholar