Recurrent desmoid tumor of the abdominal wall
Imane Toughrai, Aya Oufkir, Said Ait Laalim, Karim Ibn Majdoub, Khalid Mazaz
Corresponding author: Toughrai Imane, Department B of general surgery, Hassan II faculty hospital, Fes, Morocco 
Received: 17 Dec 2011 - Accepted: 07 Sep 2012 - Published: 20 Nov 2012
Domain: Surgery
Keywords: Desmoid tumor, recurrent tumor, abdominal wall, reconstruction
©Imane Toughrai et al. Pan African Medical Journal (ISSN: 1937-8688). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Imane Toughrai et al. Recurrent desmoid tumor of the abdominal wall. Pan African Medical Journal. 2012;13:60. [doi: 10.11604/pamj.2012.13.60.1431]
Available online at: https://www.panafrican-med-journal.com//content/article/13/60/full
Recurrent desmoid tumor of the abdominal wall
Imane Toughrai�,&, Aya Oufkir�, Said Ait Laalim�, Karim Ibn Majdoub�, Khalid Mazaz�
1Department B of general surgery, Hassan II faculty hospital, Fes, Morocco, 2Department of plastic and reconstructive surgery, Hassan II faculty hospital, Fes, Morroco
&Corresponding author
Toughrai Imane, Department B of general surgery, Hassan II faculty hospital, Fes, Morocco
Desmoid tumors constitute an aggressive form of fibromatosis, originating from muscle and aponeurosis. They account less than 3% of all soft tissue neoplasms [1,2]. Abdominal wall is one of the main location of desmoid tumors. They don't metastasize, but they have tendency to recur. Repetitive surgery makes abdominal wall reconstruction difficult.
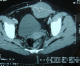
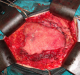
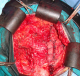
A 28- year-old female who had a history of tow caesareans. She was, also, operated 8 months before for a desmoid tumor of the abdominal wall. She was referred to our hospital for a growing mass of the lower abdominal wall. Clinical examination revealed a 10 cm mass of the left iliaca fossa, which was fixed to the pubic bone. Abdominal computed tomography scan (CT scan) demonstrated an heterogeneous para-ombilical tumor involving the left rectus abdominis muscle (Figure 1). We concluded to a recurrent desmoid tumor of the abdominal wall. The surgery was performed within the existent midline abdominal incision. The mass was originating from the left rectus abdominis muscle, arising from the ombilicus to the pubic bone in which it was strongly adhered. It extended to the limit with the inguinal ligament, to abdominal transversal and oblique muscles and to bladder on its anterior surface. The tumor was totally removed respecting at least 2 cm of margin with healthy tissue. The resection included left rectus muscle and both oblique muscles. The resulting defect in the abdominal wall measured 15/15 cm. it was repaired by a double layer mesh which was covered by a bepedicled flap using the anterior fascia of the controlateral rectus abdominis, combined with an advancement of the posterior fascia after a dissection between the residual external and internal oblique muscles (Figure 2, Figure 3). The patient recovery was uneventful and she was discharged at the 5th postoperative day. Histological examination of the specimen showed a desmoid tumor with free margins. The outcome 13 months later didn?t show any local recurrence or incisional hernia.
Abdominal desmoid tumor occur in the abdominal wall in 40 to 50% of cases [2,3]. Especially in young women, with a history of pregnancy or previous surgery [1]. It was the case in our patient. The tumor development appeared to be associated with her second caesarean which preceded symptoms four months ago. Recurrence diagnosis of desmoid tumor in our patient was facilitated by her surgical history, tumor location within the anterior abdominal wall and by the CT scan findings. In other circumstances, definitive diagnosis must be established with histo-pathologic analysis [3,4]. Desmoid tumor appearances in CT and MR imaging vary depending on their composition which changes over time [1,2,4].
�
Although they don?t metastasize, their infiltrative growth and tendency to recur even after macroscopic complete excision cause real management challenge in desmoid tumors.�
Surgery must be radical with the intent of achieving wide margins. This may leave extensive parietal loss of substance. However, it may not prevent recurrence which can occur in 20 to 30% of cases after complete resection. Recurrence rate can be more than 50% in resection R1 and R2 [5]. The median time to recurrence reported in literature is 14 to 17 months [5]. This situation leads to repeated operations. The quality of surgical excision is a major prognosis factor that influences tumor control and functional outcome, but not survival [5]. According to some authors, tumor stabilisation or regression after active phase of about 3 years is possible [1,5]. In this regard, the aggressiveness of treatment must be taken into account and compared to the benignity of the disease.�
Whether in, primary or recurrent desmoid tumor, the integrity of the abdominal wall must be restored after resection. Anatomical reconstruction by direct suture with release incision is possible [3]. Most often, prosthetic material is necessary to cover the defect. Newly developed material offers a tension free and secured repair. In our patient, we used a double layer mesh, a biomaterial with an anti-adhesive and inner surface acceptable for intra-peritoneal placement. We combined a Gibson and Micheau?s procedures which are respectively an advancement of the fascia of rectus abdominis and oblique muscles [6,7]. It?s a simple and easy technique of coverage using a well vascularized tissue that can be associated with prosthetic repair. In greater loss of substance, it?s recommended to use distant or free muscle flap.�
The effectiveness of radiation and non surgical methods such as chemotherapy, hormonotherapy and anti-inflammatory treatment is not proven yet. These therapies are recommended in patient in whom resection is technically impossible or when repetitive surgery is necessary [4,5].�
Considering the unpredictable behaviour of desmoid tumor and treatment complications, some authors advocate a wait-and-see policy as an available therapeutic option in this disease [5].
Surgery when it?s possible is still the treatment of choice, whether in primary or recurrent abdominal wall desmoid tumor. The quality of resection is a main prognosis factor. Radical surgery results in significant loss of substance in abdominal wall which can be managed using many reconstruction techniques. Repair by a double layer mesh covered by a pedicled fascial flap seems to be simple and efficient method.
The authors declare no competing interests.
All the authors have contributed to this manuscript in ways that comply to the ICMJE authorship criteria. All the authors have read and approved the final version of the manuscript.
Figure 1: abdominal CT scan shows an heterogeneous mass of the left iliaca fossa
Figure 2: operating view shows the abdominal wall defect reconstructed with a double layer mash
Figure 3: operating view shows the coverage by a bepedicled fascial flap after reconstruction
- Chia-Bang C, Yi-You C, Chih-Hsueh C, Yi-hong C et al. Sonographic computed tomography findings of intra-abdominal desmoid tumor. J Chin Med Assoc. 2010; 73: 393-395. This article on PubMed
- Kreuzberg B, Koudelova J, Ferda J et al. Diabnostic problems of abdominal desmoid tumors in various locations. Eur J Radiol. 2007 May;62(2):180-5. This article on PubMed
- Arshad AR, Normala B. Surgical management of large desmoid tumour of the anterior abdominal wall. Asian J Surg. 2008 Apr;31(2):90-5. This article on PubMed
- Teo HE, Peh WC, Shek TW. Case 84: desmoid tumor of the abdominal wall. Radiology. 2005 Jul;236(1):81-4. This article on PubMed
- Stoeckle E, Coindre J M, Longy M et al. A critical analysis of treatment strategies in desmoid tumors : a review of a series of 106 cases. EJSO. 2009; 35:129-134. This article on PubMed
- Gibson CL. Operation for cure of large ventral hernia. Ann Surg. 1920 Aug;72(2):214-7. This article on PubMed
- Micheau P, Grolleau JL, Rouge D. Large eventrations: deep extensive cleavage of the abdominal wall and prosthetic repair. Presse Med. 1995 Oct 21;24(31):1433-7. This article on PubMed