Giant viable hydatid cyst of the lung revealed by hiccups
Bouchentouf Rachid, Benjelloun Amine, Chafik Aziz, Aitbenasser Moulay Ali
Corresponding author: Bouchentouf Rachid, Department of Pulmonology, Avicenna Military Hospital, Marrakech, Morocco 
Received: 23 Apr 2012 - Accepted: 22 Sep 2012 - Published: 13 Nov 2012
Domain: Clinical medicine
Keywords: Hiccups, giant hydatid cyst, lung, surgery
©Bouchentouf Rachid et al. Pan African Medical Journal (ISSN: 1937-8688). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Bouchentouf Rachid et al. Giant viable hydatid cyst of the lung revealed by hiccups. Pan African Medical Journal. 2012;13:48. [doi: 10.11604/pamj.2012.13.48.1705]
Available online at: https://www.panafrican-med-journal.com//content/article/13/48/full
Giant viable hydatid cyst of the lung revealed by hiccups
Bouchentouf Rachid1,2,&, Benjelloun Amine1, Chafik Aziz3, Aitbenasser Moulay Ali1
1Department of pulmonology, Avicenna Military Hospital, Marrakech, Morocco, 2FMPM, Cadi Ayyad University, Marrakech, Morocco, 3Department of Thoracic Surgery, Avicenna Military Hospital, Marrakech, Morocco
&Corresponding author
Bouchentouf Rachid, Department of Pulmonology, Avicenna Military Hospital, Marrakech, Morocco
A hydatid cyst is a parasitic infection caused by Echinococcus Granulosus. The liver is the most commonly affected organ (> 65%) followed by the lung (>25%) [1], which is the predominant site of cyst formation in children. We report the case of pulmonary giant hydatid cyst revealed by hiccups and for which we have not found any similar case in the literature.
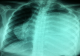
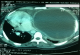
An 18-year-old woman presented with three month history of hiccups and progressive dyspnea. The patient was otherwise healthy, but there was a history of exposure to domestic dogs and sheep. Pulmonary examination revealed an abolition of breath sounds at auscultation of the left hemi thorax which was dull on percussion. Abdominal examination was normal. Chest radiograph postero-anterior view showed a very large dense homogenous opacity occupying nearly the entire left lung (Figure 1). Sonographic evaluation of the chest revealed a voluminous fluid collection occupying nearly the entire left hemithorax. The greatest collection contains daughter cysts. The computed tomography of thorax revealed a giant cystic lesion (29 cm x 17cm) occupying a large proportion of the left lung and pushing the heart to the right side (Figure 2). Biological investigations revealed the following: haemoglobin: 10 g/dl, white cells: 5700, C Reactive protein: 62 mg/l. Serum immunoglobulin titers were negative for Echinococcus granulosus. Abdominal ultrasonography did not revealed cysts. The diagnosis of giant hydatid cyst was made intraoperatively and cyst was removed conservatively. The postoperative was satisfactory and hiccups disappeared completely. Written informed consent was obtained for publication of this case report and accompanying images.
Hiccups are a sudden, irregular and spasmodic contraction of the diaphragm followed by an abrupt closure of the glotti. The cause of hiccups was due to compression of the phrenic nerve in the mediastinum. Echinococcosis is a parasitic disease frequently seen in sheep and cattle raising countries with poor sanitary conditions. Hydatid disease is endemic in Morocco; the annual incidence of chirurgical hydatid disease is 6.4/100000 in the Moroccan population [2]. Hepatic infestation is most commonly seen followed by lung involvement that has been seen in 25% of the cases, in some series [1]. Giant hydatid cysts of the lung are defined as cysts measuring 10 cm or more [3]. This entity is most frequently encountered in adolescents and in children older than ten year [3,4]. This predominance is explained by the fact the immune system and the relatively higher elasticity of the lung tissue in children and adolescents allows the rapid growth of cysts. The lung hydatid disease is frequently asymptomatic in children [3]. Nevertheless, giant lung hydatid cysts were constantly symptomatic [3-5]. Common presenting symptoms of giant pulmonary hydatid cyst are compression symptoms such as dry cough, while ruptured cyst can cause productive cough, chest pain, dyspnea, and very rarely anaphylactic shock. In our case, symptoms were chest pain and dyspnea, and hiccups. The diagnosis is easy in endemic areas. The patient is usually in good general health in cases of non-complicated cysts and chest X-ray will show a well-circumscribed dense homogenous opacity [6]. Giant pulmonary hydatid cysts can be located elsewhere in the lung but in literature they were located most commonly in the right lower lobe .In our case hydatid cyst was located in the left lower lobe. Computed tomography (CT) scan is not mandatory; however, it displays better information about the size of the hydatid cyst, and its relation to the lung parenchyma [7]. Serological tests have limited diagnostic value, and the inclusion of abdominal ultrasonography in the protocol of investigation is necessary because of the coexistence of hepatic cysts [8].
�
The chest X-ray and computerized thoracic tomography are generally sufficient for diagnosis. However a definite diagnosis was based on pathological confirmation. Surgery remains the treatment of choice for hydatid disease; the current treatment is complete excision of disease process with maximum preservation of the lung tissue. Medical treatment can be used during the postoperative period, in order to prevent the recurrence and occurrence of a secondary cyst.
Pulmonary giant hydatid cyst is a rare and a special clinical entity. The diagnosis must be evoked in front of opacity of the hemi thorax especially in a country of endemic disease.
The authors declare no competing interest.
All the authors have contributed to this case report and have read and approved the final version of the manuscript.
Figure 1: Posteroanterior radiograph of the giant pulmonary hydatid Cyst which pushed the heart to the right side
Figure 2: The computed tomography scan demonstrating the cyst completely involved the left Thorax
- Moro P, Scantz PM. Echinococcosis: a review. Int J Infect Dis. 2009; 13: 125-133. This article on PubMed
- Ould Ahmed Salem CB, Schneegans F, Chollet JY. Study of lesional aspects of hydatid echinococcosis in Man in Mauritania: fertility, histology of hydatid cysts and protoscolex viability. Bull Soc Pathol Exot. 2011; 104:1-5. This article on PubMed
- Karaoglanoglu N, Kurkcuoglu IC, Gorguner M, Eroglu A, Turkyilmaz A. Giant hydatid lung cysts. Eur J Cardiothorac Surg. 2001; 19: 914-7. This article on PubMed
- Arroud M, Afifi A, El Ghazi K, Nejjari CH, Bouabdallah Y. Lung hydatid cysts in children: comparison study between giant and non-giant cysts. Pediatr Surg Int. 2009; 25:37-40. This article on PubMed
- Ghallab NH, Alsabahi AA. Giant viable hydatid cysts of the lung: a case report. J Med Case Rep. 2008; 2:359. This article on PubMed
- Beggs I. The radiology of hydatid disease. AJR Am J Roentgenol. 1985; 145 (3):639-648. This article on PubMed
- Erdem CZ, Erdem LO. Radiological characteristics of pulmonary hydatid disease in children, less common radiological appearances. Eur J Radiol. 2003; 45:123-8. This article on PubMed
- Ulku R, Onen A, Onat S. Surgical treatment of pulmonary hydatid cysts in children: report of 66 cases. Eur J Pediatr Surg. 2004; 14: 255-9. This article on PubMed