Paraperesis: a rare complication after depressed skull fracture
Ali Asmat Syed, Anjum Arshad, Khatoon Abida, Sardha Minaksh
Corresponding author: Dr. Syed Asmat Ali, Assistant Professor, Department of Surgery, Jawaharlal Nehru Medical College, Aligarh Muslim University, Uttar Pradesh, India 
Received: 14 Oct 2011 - Accepted: 25 May 2012 - Published: 14 Aug 2012
Domain: Clinical medicine
Keywords: Fracture, paraperesis, edema, depressed fracture, skull
©Ali Asmat Syed et al. Pan African Medical Journal (ISSN: 1937-8688). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Ali Asmat Syed et al. Paraperesis: a rare complication after depressed skull fracture. Pan African Medical Journal. 2012;12:106. [doi: 10.11604/pamj.2012.12.106.1304]
Available online at: https://www.panafrican-med-journal.com//content/article/12/106/full
Paraperesis: a rare complication after depressed skull fracture
Ali Asmat Syed1,&, Anjum Arshad1, Khatoon Abida1, Sardha Minakshi1
1Jawaharlal Nehru Medical College, Aligarh Muslim University, Uttar Pradesh, India
&Corresponding author
Dr. Syed Asmat Ali, Assistant Professor, Department of Surgery, Jawaharlal Nehru Medical College, Aligarh Muslim University, Uttar Pradesh, India
Head injury is a leading cause of mortality and morbidity particularly in developing countries. It usually manifests as skull fracture, which is a break in the cranial bones. It is common after fall from height, road traffic accidents, physical assault and other injuries [1]. The incidence of skull fractures among head injured adults who present to emergency departments (ED) is unknown. The parietal bone is most frequently fractured, followed by the temporal, occipital, and frontal bones [2]. Skull fractures are grossly classified into linear, depressed and comminuted types. Linear fractures are the most common, followed by depressed skull fractures [3]. A skull fracture is considered depressed, when any portion of the outer table of the of fracture and depth of fracture line lies below the normal anatomical position of the inner table Depressed skull fractures typically occur when objects with a large amount of kinetic energy make contact with the skull over a fairly small area [4]. Most of the depressed fractures are over the front-parietal region (75%) as the bone is thin and the site is more prone to physical assault [5].
�
�
A 55-year old man, was hit on head by a wooden rod, he was brought within 1 hour of the alleged physical assault. He complained of pain, swelling and cut over scalp without any history of nausea, vomiting, loss of consciousness and other symptoms of head injury. On examination, his Glasgow Coma Scale (GCS) was 15/15, pupils were bilateral equal and reacting. He had no signs of neurological deficit. On local examination he had redness, swelling and laceration 1 x 1 cm over left high parietal region. Patient was managed conservatively and kept for 24 hours observation, in line with the protocol for head injury cases. Next day, patient complained of diffuse headache followed by difficulty in walking.
�
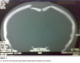
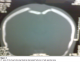
On examination he had weakness of both lower limbs, with right sided affected more than left. Motor power on right lower limb was 3/5 and on left lower limb it was 4/5. Deep tendon reflexes were exaggerated and plantar reflex was extensor, on both the limbs. Computerized Topography (CT) scan of head was done which showed small bilateral depressed fractures of the high parietal bones (Figure 1). Symmetrically depressed fragments of parietal bones associated with hypodensities in the adjacent brain parenchyma, suggestive of edema were seen. However there was no evidence of associated injury around superior sagittal sinus and hematoma or contusion in the brain parenchyma (Figure 2, Figure 3).�
The patient was managed conservatively for underlying associated brain edema, around high cortex region and he responded well. His weakness progressively improved and he was discharged after 2 weeks without any sequelae.
Depressed skull fractures can occur in a variety of settings, depending upon several variables like the age, thickness of the vault, make of object, the force of the impact etc. The size of impacting device and the force of impact are directly related to the magnitude of the dynamic load. In this case, a wooden rod with large amount of kinetic energy made contact with small area over the skull leading to depressed skull fracture. Further, as in our case, initially there were no associated neurological manifestations of injury, so depressed fractures may be missed if radiological investigations are not done. Even careful clinical examination sometime does not reveal anything although complications and sequelae of depressed skull fractures can be minimised by early diagnosis [6]. The scalp is relatively mobile and any area of depression may not lie directly beneath the laceration. Visual inspection of the skull through the scalp laceration may fail to reveal a fracture. Careful digital exploration of the scalp wound with a gloved finger would reveal a bone edge, a depression, or a mobile bone fragment but this could not be performed in our case, as wound was just 1 cm in size. The management of choice in preventing infection from open depressed skull fractures is operative debridement and thorough irrigation, though there is evidence that selected cases can be safely managed without operation especially if the site of fracture is in proximity of the venous sinuses [7-8]. Post trauma, brain edema after depressed fracture is usual phenomenon and patient can present as neurological deficit depending upon area of brain affected. However, local edema subsides usually after few days once active phase of injury is over [9].
We conclude that, at times mild head injury can manifest as depressed skull fracture. Further, paraperesis is also a rare complication of depressed skull fracture.
The authors declare no competing interests.
All the authors have contributed to the manuscript and have read and approved the final version.
Figure 1: CT scan of the head showing bilateral depressed parietal bone fracture
Figure 2: Bone window of coronal CT scan showing depressed fractures of bilateral parietal bones in high parietal region
Figure 3: CT scan of the head showing bilateral depressed factures in high parietal area
- Jennet B. Epidemiology of head injury. J Neurol Neurosurg Psychiatry. 1996; 60:362?9. This article on PubMed
- Golfinos, JG, Cooper, PR. Skull fracture and post-traumatic cerebrospinal fluid fistula. In: Head Injury - 4th edition. Cooper, PR, Golfinos, JG (Eds).
- Geisler FH. Skull fractures. In: Wilkins RH, Regachary SS, eds. Neurosurgery.
- Mehdi SA, Ahmed CB, Dogar IH, Shaukat A. Depressed skull fracture; Interrelationship between CT evaluation of & its clinical findings. Professional Med J. 2010 Dec; 17(4):616-622.
- Ishman SL, Friedland DR. Temporal bone fractures: traditional classification and clinical relevance. Laryngoscope. 2004 Oct;114(10):1734-41. This article on PubMed
- Marion DW. Complications of head injury and their therapy. Neurosurg Clin N Am. 1991 Apr;2(2):411-24. This article on PubMed
- Van der Heever CM, Van der Merwee DJ. Management of depressed skull fractures Selective conservative management of nonmissile injuries. J Neurosurg. 1989;71:186?90. This article on PubMed
- Bullock MR, Chesnut R, Ghajar J, Gordon D, Harti R,Newell DW, et al. Surgical management of depressed skull fractures. Neurosurgery. 2006; 58 (3 suppl): S56-60. This article on PubMed
- Fuentes S, Metellus P, Levrier O, Adetchessi T, Dufour H, Grisoli F. Depressed skull fracture overlying the superior sagittal sinus causing benign Intracranial hypertension Description of two cases and review of the literature.Br J Neurosurg. 2005 Oct;19(5):438-42. This article on PubMed