A case report of a huge congenital granular cell epulis operated under local anesthesia
Khalid Khattala, Mohamed Rami, Aziz Elmadi, Leila Chbani, Youssef Bouabdallah
Corresponding author: Khalid Khattala, Department of pediatric surgery, Hospital university Hassan II,Fez, Morroco 
Received: 11 Jun 2012 - Accepted: 09 Jul 2012 - Published: 14 Aug 2012
Domain: Clinical medicine
Keywords: Congenital granular cell tumor, gingival tumor, newborn, local anesthesia
©Khalid Khattala et al. Pan African Medical Journal (ISSN: 1937-8688). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Khalid Khattala et al. A case report of a huge congenital granular cell epulis operated under local anesthesia. Pan African Medical Journal. 2012;12:105. [doi: 10.11604/pamj.2012.12.105.1816]
Available online at: https://www.panafrican-med-journal.com//content/article/12/105/full
Original article 
A case report of a huge congenital granular cell epulis operated under local anesthesia
A case report of a huge congenital granular cell epulis operated under local anesthesia
Khalid Khattala1,&, Mohamed Rami1, Aziz Elmadi1, Leila Chbani2, Youssef Bouabdallah1
1Department of pediatric surgery, Hospital university Hassan II,Fez, Morroco, 2Department of histopatghology, Hospital university Hassan II,Fez, Morroco
&Corresponding author
Khalid Khattala, Department of pediatric surgery, Hospital university Hassan II,Fez, Morroco
Congenital granular cell tumour (CGCT) was first described by Neumann in 1871 [1]. One hundred and sixty seven cases have been reported, with a maxillary to mandible ratio of 3:1 and a female to male ratio 10:1[2]. The etiology of the condition is not clear. Surgical excision is advocated as the treatment of choice for this tumor. We report a new case who presented an intraoral tumor mass which was protruding from her mouth, compromising feeding. The lesion was removed under local anesthesia with good follow-up.
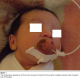
A 2 day old girl, born at 41 weeks gestation weighting 3,500kg, was referred with a growth in the anterior maxillary alveolus which was noticed at birth. Clinical examination revealed a full term female neonate with a huge, exophytic growth protruding from the oral cavity, measured approximately 4x2 cm in size. The tumor was attached by a large pedicleto the anterior maxillary ridge; the mass was firm in consistency and not tender to digital palpation. The initial management included intravenous fluids and gastric feeding as oral feeding was impossible for this child (Figure 1).
�
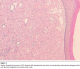
The tumor was excised under local anesthesia without a prior biopsy. No other lesions or systemic involvement was found. These were no complication after surgery. Histopathology confirmed the diagnosis of a completely excised congenital gingival granular cell tumour (Figure 2). Immunohistochemical investigation confirmed the diagnosis.
CGCT occurs in the mucosa of the maxillary alveolus as smooth surface pink mass, usually not associated with any other abnormality of the teeth or other congenital abnormalities [2]. It have usually been sporadically presented as isolated case reports in British literature, since the first case was described in Germany in 1871 as a congenital epulis by Neumann [1,3]. The tumor is postulated to originate from indifferentiatedmesenchymal cell, fibroblasts, myofibroblasts, histiocyts, Schwann cells or odontogenic epithelial cells; it is a benign mesenchymal tumor of unknown origin [4]. CGCT is a very rare lesion that appears as a sessile or pedunculated lesions protruding from the neonate�s mouth. The tumor occurs ten times more frequently in females than males and three times more frequently in the maxilla than mandible. It usually occurs as a single mass although 10% cases occur as multiple [5]. They are usually less than 1,5cm diameter [6]. Local excision is curative, with no reported recurrences in the literature, even when the excision has been incomplete [7], the CGCT removal under local anesthesia is an alternative if intubation is not possible us in our case or in case of small lesion [8]. Histopathology is the gold standard in the diagnostic process.
CGCT is a very rare mouth tumor, the lesion can be removed under local anesthesia if intubation is not possible, and the diagnosis can be confirmed after histopathology study, without possibility of recurrence.
The authors declared that they have no competing interest.
Khattala Khalid contributed to the writing the manuscript and the treatment of the patient, Rami Mohamed and Elmadi Aziz contributed to the writing the manuscript, Chbani Leila and andBouabdallah Youssef contributed to the treatment of the patient and the write-up of the manuscript. All the authors have read and approved the final version of the manuscript.
Figure 1: The preoperative appearance of the tumour showing It arising from the anterior maxillary alveolus (note the gastric tube for feeding)
Figure 2: Section through the tumour (x 250) stained with haematoxylin and eosin, demonstrating characteristic polygonal cells with granular cytoplasm and small round nuclei
- Eman A and Alls. Exploration of the Histogenesis of Congenital Granular Cell Epulis: An Immunohistochemical Study. Journal of the Egyptian Nat Cancer Inst. 2009; 21(2): 77-83. This article on PubMed
- Kannan S, Karthiga,Rajesh R. Congenital epulis - congenital granular cell lesion: A case report. Journal of Indian society of pedodontics and preventive dentistry. 2006; 24(2): 104-106. This article on PubMed
- Bukola F Adeyemi, Abideen O Oluwasola, Akinyele O Adisa. Congenital epulis. Indian journal of dental research. 2010; 21(2) : 292-294. This article on PubMed
- Godra A, D'Cruz CA, Labat MF. Pathologic quiz case: a newborn with a midline buccal mucosa mass - Congenital gingival granular cell tumor (congenital epulis). Arch Pathol Lab Med. 2004; 128:585-586. This article on PubMed
- Gokhale UA, Malhotra CJ. Congenital epulis of the newborn. Indian J Pathol Microbiol. 2009 Jul-Sep;52(3):436-7. This article on PubMed
- Mustafa Inan et Al. Congenital fibrous epulis in the infant. Yonsei medical journal. 2002; 43( 5): 675-677. This article on PubMed
- Anderson PJ, Kirkland P, Schafler K, Moss AL. Congenital gingival granular cell tumour. J R Soc Med. 1996 Jan;89(1):53P-4P. This article on PubMed
- Cheong SP, Fahy CJ, Craigie MJ. Anesthesia for excision of an intraoral mass in a neonate: use of a laryngeal mask during removal of congenital epulis. Anaesthesia and Intensive Care. 2008; 36(1): 116-118. This article on PubMed