Epidemiology of rotavirus diarrhea in children under 5 years in Northern Cameroon
Valentine Ngum Ndze, Achidi Eric Akum, Gonsu Hortense Kamga, Lyonga Emilia Enjema, Mathew Dioh Esona, Krisztian Banyai, Obama Abena Marie Therese
Corresponding author: Valentine Ngum Ndze, Faculty of Medicine and Biomedical Sciences, University of Yaound� I, Yaound�, Cameroon 
Received: 30 Jan 2012 - Accepted: 05 Mar 2012 - Published: 17 Apr 2012
Domain: Epidemiology
Keywords: Rotavirus, diarrhea, Cameroon, children, epidemiology, prevalence
©Valentine Ngum Ndze et al. Pan African Medical Journal (ISSN: 1937-8688). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Valentine Ngum Ndze et al. Epidemiology of rotavirus diarrhea in children under 5 years in Northern Cameroon. Pan African Medical Journal. 2012;11:73. [doi: 10.11604/pamj.2012.11.73.1548]
Available online at: https://www.panafrican-med-journal.com//content/article/11/73/full
Epidemiology of rotavirus diarrhea in children under 5 years in Northern Cameroon
Valentine Ngum Ndze1,&, Achidi Eric Akum2, Gonsu Hortense Kamga1, Lyonga Emilia Enjema1, Mathew Dioh Esona3, Krisztian Banyai4, Obama Abena Marie Therese1
1Faculty of Medicine and Biomedical Sciences, University of Yaound� I. Cameroon, 2Faculty of Health Sciences, University of Buea, Cameroon, 3Division of Viral Diseases, National Center for Immunization and Respiratory Diseases, Centers for Disease Control and Prevention, Atlanta, GA, USA, 4Veterinary Medical Research Institute, Hungarian Academy of Sciences, Hungariat krt. 21, Budapest 1143, Hungary
&Corresponding author
Valentine Ngum Ndze, Faculty of Medicine and Biomedical Sciences, University of Yaound� I, Yaound�, Cameroon
Diarrhea still remains one of the leading causes of childhood mortality worldwide particularly in developing countries, causing approximately 1.87 million deaths each year [1]. Group A rotavirus (RVA) infection is the most important cause of severe diarrhea in childhood causing 20% of fatal diarrhea in young children [2,3]. The annual estimates of rotavirus-related mortality in children <5 years, show that about 453000 children die worldwide due to rotavirus [4].
�
Since 2006, two rotavirus vaccines, RotaTeqTM (Merck and Co, PA, USA) and Rotarix� (GlaxoSmith Kline Biologicals, Rixensart, Belgium), have been licensed, and they are recommended for use in all countries by WHO, particularly in those countries with high diarrhea-related mortality in children younger than 5 years [5]. Limited data is available on rotavirus disease burden in Cameroon, particularly in the North West and Far North regions. The aim of this study was to determine the prevalence of group A rotavirus in children below 5 years with acute diarrhea in two regions of Northern Cameroon (North West and Far North Regions) so as to improve our knowledge on the burden of rotavirus disease in Cameroon for imminent introduction of a rotavirus vaccine.
Study site and study population
�
A descriptive cross-sectional study was conducted from October 2010 to July 2011 in Northern Cameroon (at the Regional Hospital Maroua and at the Domayo Djama integreted health center in the Far North region; and at the Regional hospital Bamenda and at the Esu integrated health centre in the North West region). The Far North region vegetation is mainly the Sahel type and is dry all year round with minor rains in the months of June, July and August. The North West region is mainly grassland characterized by equal dry chilly and rainy seasons. The population is urban (Maroua and Bamenda) and rural (Esu) and the major occupation in the study area is subsistence agriculture supplemented with fishing and dairy farming in the Far North region. Included in the study were all in- and out-patients less than 5 years who presented with acute diarrhea at the study sites and whose parents gave their informed consent to participate in the study.�
Sampling and Sample collection�
Participants were recruited in the order at which the cases presented. After informed consent was obtained, a pediatrician, medical doctor or consulting nurse assigned to the study examined each patient and filled out the demographic data and information on clinical symptoms and illness onset on a standardized questionnaire. A single fresh stool per participant per diarrhea episode was collected following microbiologically approved techniques. The samples were transported to the Hospital laboratory within 2 hours after collection and stored at -20°C and later transported on dry ice to the Veterinary Medical Research Institute, Hungarian Academy of Science, Budapest-Hungary where rotavirus detection was carried out.�
Laboratory detection of RVA�
Fecal suspensions (10%) were prepared in phosphate buffered saline and stored at -20°C. Rotavirus dsRNA was extracted from 100�l stool suspension using the Promega kit by the Cobett Nucleic acid automatic extractor following the manufacturer�s instructions [6]. Rotavirus A was detected by one-step RT-PCR (QIAGEN Kit) of gene 6 with VP6F and VP6R primers previously described [7]. In brief, denaturation of dsRNA was carried out at 97�C for 5 minutes, then reverse transcription carried out at 52�C for 30 minutes, activation of Taq polymerase at 95�C for 15 minutes followed by 40 cycles of PCR (denaturing at 95�C for 30sec, annealing at 52�C for 30sec, and extension at 72�C for 1 min) and a final extension cycle (72�C for 3 min). The cDNA was then ran on 1% Agarose gel (Seakem� LE agarose) electrophoresis in standard Tris-Borate-EDTA buffer to determine samples positive for group A rotavirus. Gels were stained with Gelred (Biotum).�
Data analysis�
Data was analyzed using Microsoft excel and Epi Info version 3.5.1. Prevalence was expressed as percentages. The Chi square test was used to analyze categorical variables and the Yates correction test where appropriate. A 95% confidence interval (CI) was calculated and values of P < 0.05 were considered significant.�
Ethical issues�
An ethical clearance was obtained from the Cameroon National Ethics Committee and administrative authorizations obtained from the different health care settings in our study.
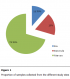
A total of 390 infants and young children with diarrhea were included in this study, 275 (70.5%) from Maroua, 70 (18%) from Bamenda and 45 (11.5%) from Esu (Figure 1) with a mean age of 14.8 months (median, 11 months; range 1-60 months). The sex distribution was 179 (45.9%) females to 211 (54.1%) males with mean ages of 15 months and 14.7 months (median, 11 months and 12 months, respectively). Of the 390 children with diarrhea, 252 (64.6%) were hospitalized and 138 (35.4%) were of the out-patient department.
�
This study reveals that 42.8% (167/390) of the children presenting with diarrhea were infected with group A rotavirus. The prevalence of RVA in children in the in-patient (49.2%) and the out-patient (31.2%) was significantly different, X2(Yates) =11.14, P=0.00085. The prevalence of group A rotavirus in the two sexes was similar 40.8% in males as to 45.3% in females as shown in Table 1. There was no significant difference observed when the prevalence of rotavirus in males was compared to that of females, X2 (Yates) =0.43, P=0.43. The highest number of cases with rotavirus infection was observed in the age group 0-12 months (47.9%) while the age group 49-60 months had the lowest prevalence (25%) (Table 1).�
It was observed that children positive for rotavirus who had diarrhea accompanied with fever and vomiting in the outpatient group and inpatient group were 13.0% and 28.6% respectively, P=0.03. (Table 2).
The aim of this study was to determine the prevalence of rotavirus in children ≤ 5 years presenting with acute gastroenteritis in two regions of Northern Cameroon (North West and Far North Regions). Our study showed a rotavirus prevalence of 42.8% (North West region 33.9% and Far North region 46.5%) and was significantly higher among hospitalized children.
�
Many studies have shown the important role of rotavirus as a cause of diarrhea in children in both developed and developing countries [8-13]. Most of the cases occurred in children less than 5 years of age. This detection rate is greater than what was obtained by Esona and co-workers (21.9%) during a 2003 study in Western Cameroon but similar to what was found in recent studies conducted in other parts of Africa [4,14,15]. It is noteworthy that detection of rotavirus in this study was done by RT-PCR while that of the 2003 study in Western Cameroon was done using an enzyme immunoassay (EIA) method. The Far North region is a flood prone region and has the highest occurrence of diarrhea disease in Cameroon. These factors combined might explain the difference in the prevalence estimates of rotavirus observed in Cameroon. The prevalence of rotavirus in the Far North region was 46.5% (128/275) indicating that rotavirus is an important contributor to the causes of diarrhea in this region of Cameroon and rotavirus may have aggravated the cholera situation since most of the rotavirus cases identified in this study site were recorded just after the cholera epidemic. There was a significant difference in the prevalence of rotavirus between the health care settings with higher incidence among hospitalized children. It should be noted that the sampling was biased and therefore not sufficiently comparable. The prevalence of rotavirus in the rural area (28.9%) was lower than that in the urban area (44.6%). The fact that patients from rural area had access primarily to outpatient clinic could have distorted this finding. Also the rural population may only report to the hospital when diarrhea had already subsided or toward the end of the episode. All this is due to transportation and availability of over the counter medication which may mask the disease. Cultural belief is also a factor that can keep mothers from reporting to the hospital at the onset of diarrhea disease. Most of the rotavirus cases were identified in the age group 0-24 months and it was observed that rotavirus detection rate decreases with age. This is in accordance with other studies [9,16] which also showed that rotavirus infection decreases with increasing age, due to acquired immunity that comes with age or asymptomatic infections [17,15]. Overall, a seasonal trend was observed in this study with most of the rotavirus cases occurring in the dry season with a detectable peak in the months of November and December (Figure 2). This finding is in contrast to what was observed by Esona and co-workers in 2003 in Western Cameroon where rotavirus infection was observed all year round. Caution should be taken in interpreting these results as data was not collected for a sufficiently longer period.�
Estimates on rotavirus mortality have been published previously. In 2003, Parashar and colleagues estimated ~18,500 diarrhea and 3696 RVA-associated child mortality occur in Cameroon annually [18], whereas the WHO�s 2004 report on child mortality due to diarrhea and rotavirus in Cameroon was ~14,500 and 4369 deaths (95% CI, 3612-5126), respectively [19,20]. These earlier estimates are based on lower detection rates (mean detection rate of 33%; 95% CI, 28-38) [4], for RVA utilized in calculations for Cameroon. Given the higher detection rate for RVA in this study, however, we anticipate that the number of rotavirus-associated deaths might be higher and stands at 6199 during 2010-2011 using the algorithm implemented by Parashar et al., (2003). This greater incidence of RVA infection is in agreement with estimates by the WHO for 2009-2010 [21].
This study showed that the prevalence of rotavirus was high (42.8%) especially among children admitted to hospital due to diarrhea in Northern Cameroon. Seeing the increase in RVA detection rates, continuation of enhanced surveillance is needed to better understand rotavirus disease burden in Cameroon. Further characterizations of the positive RVA cases have been initiated.
We acknowledge the support from the Ministry of Women Empowerment and the Family Cameroon for financial support during sample collection. We also thank the medical doctors, nurses and laboratory technicians who assisted in this work at the different study sites.
Authors declare that they have no conflict of interest
V.N.N, A.E.A, M.D.E, K.B and O.A.M.T designed the study. VNN, KB, MDE, GHK and LEE drafted the first version. All authors participated in the final version.
Table 1: Socio-demographic characteristics
Table 2: Clinical characteristics in relation to presence of RVA in hospitalized and out-patient cases
Figure 1: Proportion of samples collected from the different study sites
Figure 2: Monthly (seasonal) prevalence of group A rotavirus in Northern Cameroon
- Boschi-Pinto C, Velebit L and Shibuya K. Estimating child mortality due to diarrhoea in developing countries. Bull World Health Organ. 2008 Sep;86(9):710-7. This article on PubMed
- Parashar U D, Gibson C J, Bresee J S, and Glass R I. Rotavirus and severe childhood diarrhea. Emerging Infectious Diseases. 2006;12:304-306. This article on PubMed
- Estes M. and A. Kapikian. Rotaviruses. 2007. p. 1917-1974. In Fields Virology, D. M. Knipe, P. M. Howley, D. E. Griffin, R. A. Lamb, M. A. Martin, B. Roizman, and S. E. Straus. (ed.), 5th ed, vol. 2. Kluwer/Lippincott, Williams and Wilkins, Philadelphia, PA.
- Tate JE, Burton AH, Boschi-Pinto C, Steele AD, Duque J, Parashar UD. 2008 estimate of worldwide rotavirus-associated mortality in children younger than 5 years before the introduction of universal rotavirus vaccination programmes: a systematic review and meta-analysis. Lancet Infect Dis. 2012 Feb;12(2):136-41. This article on PubMed
- World Health Organization. Meeting of the Strategic Advisory Group of Experts on immunization, October 2009 - conclusions and recommendations.Wkly Epidemiol Rec. 2009 Dec 11;84(50):517-32. . This article on PubMed
- Gyuranecz M, Rigo K, Dan A, Foldvari G, Makrai L, Denes B, Fodor L, Majoros G, Tirjak L, Erdelyi K. Investigation of the Ecology of Francisella tularensis During an Inter-Epizootic Period. Vector Borne Zoonotic Dis. 2011 Aug;11(8):1031-5.. This article on PubMed
- Iturriza-Go`mara, M, Wong C, Blome S, Desselberger U, and Gray J. 2002 Molecular characterization of VP6 genes of human rotavirus isolates: correlation of genogroups with subgroups and evidence of independent segregation. J Virol. 2002 Jul;76(13):6596-601.. This article on PubMed
- Koulla-Shiro S, Loe C, Ekoe T. Prevalence of Campylobacter enteritis in children from Yaounde (Cameroon). Central African Journal of Medicine. 1995; 41:91-94. This article on PubMed
- Esona MD, Armah GE, Steele AD. Molecular epidemiology of rotavirus infection in Western Cameroon. Journal of Tropical Pediatrics. 2003;49:160-163. This article on PubMed
- Bok K, Castagnaro N, Borsa A, Nates S, Espul C, Fay O et al. Surveillance for rotavirus in Argentina. Journal of Medical Virology. 2001; 65:190-198. This article on PubMed
- Glass R I, Lew J F, Gangarosa R E, LeBaron C W, and Ho M S. Estimates of morbidity and mortality rates for diarrheal diseases in American children. Journal of Pediatrics. 1991; 118:S27-S33. This article on PubMed
- Khetawat D, Ghosh T, Bhattacharya M K, Bhattacharya S K, and Chakrabarti S. Molecular characterization of the VP7 gene of rotavirus isolated from a clinical sample of Calcutta, India. Virus Res. 2001; 74:53-58. This article on PubMed
- Staat M A, P H Azimi, T Berke, N Roberts, D I Bernstein, R L Ward, et al. Clinical presentations of rotavirus infection among hospitalized children. Pediatric Infectious Disease Journal. 2002; 21:221-227. This article on PubMed
- Nakawesi JS, Wobudeya E, Ndeezi G, Edison A Mworozi EA, Tumwine JK. Prevalence and factors associated with rotavirus infection among children admitted with acute diarrhea in Uganda. BMC Pediatrics. 2010; 10:69. This article on PubMed
- Odimayo MS, Olanrewaju WI, Omilabu SA, Adegboro B. Prevalence of rotavirus-induced diarrhea among children under 5 years in Ilorin, Nigeria. J Trop Pediatr. 2008;(54)5:343-346. This article on PubMed
- Bui Thi Thu Hien, Do Thuy Trang, Flemming Scheutz, Phung Dac Cam1, K�re Molbak and Anders Dalsgaard. Diarrhoeagenic Escherichia coli and other causes of childhood diarrhoea: a case-control study in children living in a wastewater-use area in Hanoi, Vietnam. J Med Microbiol. 2007 Aug;56(Pt 8):1086-96. This article on PubMed
- Jiang B, Gentsch J R, and Glass R I. The role of serum antibodies in the protection against rotavirus disease: an overview. Clin Infect Dis. 2002 May 15;34(10):1351-61.. This article on PubMed
- Parashar UD, Hummelman EG, Bresee JS, Miller MA, and Glass RI. Global Illness and Deaths Caused by Rotavirus Disease in Children. Emerging Infectious Diseases. 2003; 9; 5: 565-572. This article on PubMed
- Black RE, Cousens S, Johnson HL, Lawn JE, Rudan I, Bassani DG, et al. Global, regional, and national causes of child mortality in 2008: a systematic analysis. Lancet. 2010 Jun 5;375(9730):1969-87. This article on PubMed
- Neuzil KM, Armah GE, Parashar UD, and Steele AD. Rotavirus in Africa: Shifting the Focus to Disease Prevention. J Infect Dis. 2010 Sep 1;202 Suppl:S1-4. This article on PubMed
- World Health Organisation. Rotavirus surveillance worldwide - 2009. Wkly Epidemiol Rec. 2011 Apr 29;86(18):174-6. This article on PubMed