Giant right intrascrotal paratesticular lipoma: a case report
I Made Udiyana Indradiputra, Paksi Satyagraha
Corresponding author: Paksi Satyagraha, Department of Urology, Faculty of Medicine, Brawijaya University-Saiful Anwar Hospital Malang, East Java, Indonesia 
Received: 29 Mar 2018 - Accepted: 16 Jul 2018 - Published: 07 Nov 2018
Domain: Urology
Keywords: Lipoma, intrascrotal, paratesticular, rare disease
This article is published as part of the supplement Malang Continuing Urology Education: Reconstruction and Functional Urology, commissioned by Committee for the 1st InaGURS International Workshop & Symposium of Reconstruction &.
©I Made Udiyana Indradiputra et al. Pan African Medical Journal (ISSN: 1937-8688). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: I Made Udiyana Indradiputra et al. Giant right intrascrotal paratesticular lipoma: a case report. Pan African Medical Journal. 2018;31(1):8. [doi: 10.11604/pamj.supp.2018.31.1.15616]
Available online at: https://www.panafrican-med-journal.com//content/series/31/1/8/full
Giant right intrascrotal paratesticular lipoma: a case report
I Made Udiyana Indradiputra1, Paksi Satyagraha1,&
1Department of Urology, Faculty of Medicine, Brawijaya University-Saiful Anwar Hospital Malang, East Java, Indonesia
&Corresponding author
Paksi Satyagraha, Department of Urology, Faculty of Medicine, Brawijaya University-Saiful Anwar Hospital Malang, East Java, Indonesia
Benign paratesticular mesenchymal tumors of the scrotum, especially lipomas, are extremely rare. The regions of origin of intrascrotal lipomas are not fully detectable. Even though they mostly develop from the epididymis or spermatic cord, they may also rarely originate from the tunica vaginalis or subcutaneous fat of the scrotal wall. We reported one rare case of a painless giant right-sided scrotal mass suggestive of paratesticular lipoma.
Lipoma is the most common soft tissue tumor composed of adipose tissue to occur in the human body. Lipomas of the scrotum are rare and are diagnosed usually as an incidental finding in association with a hernia; in some cases, they are the only finding, without an associated hernia sac [1, 2]. These tumors are underdiagnosed because of their benign course. The term giant lipoma of the scrotum is used for tumors whose size exceeds 10 cm [3]. There are only a few reported cases of giant lipoma of the scrotum. We present here a case of giant intrascrotal paratesticular lipoma presented as a big scrotal mass, and its surgical management.
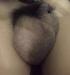
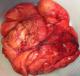
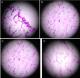
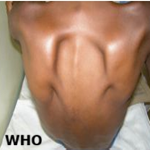
A 49-year-old male patient presented with a painless right-sided scrotal mass, that had slowly but continuously grown in the previous 18 months. It caused inconvenience only by its weight and bulk. On examination, the right scrotum was filled by an elastic, non-tender, and regularly shaped large mass (Figure 1). All laboratory panels were normal. Doppler scrotal ultrasound was conducted and revealed an echo-heterogenic structure with normal vascularization without bowel appearance which was apart from the testis. Both spermatic cords and testicles were normal. In addition, no testicular calcification was observed. Thus, intrascrotal lipoma with differential diagnosis of an omental hernia was suspected (Figure 2). Surgery was conducted (Inguinoscrotal incision); it found an intact right testis and epididymis. A huge tumor was found, slightly adhered to the tunica vaginalis. The tumor was completely dissected; a mass of densely packed fat was revealed, 19 * 15 * 6cm in size and 700g in weight. No postoperative complication was noted (Figure 3). Microscopic examination of the tumor revealed mature benign lipomatous tissue with vascularization and minimal fibrous collagen tissue, suggestive of lipoma. No anaplastic cells were detected. The final diagnosis was paratesticular lipoma. During the follow-up, no symptoms and no recurrent mass were observed early, 6 months and 1 year after the procedure (Figure 4).
Lipoma is the most common benign tumor of the spermatic cord. Giant lipoma remains a poorly defined entity. Most lipomas are found incidentally during hernia surgery [1, 2]. In our case, the tumor measured over 19 cm in its greatest dimension. In the present case, the patient presented with right painless inguinoscrotal swelling; laboratory findings were normal and Doppler ultrasound was suspicious of intrascrotal lipoma with differential diagnosis of an omental hernia. The confirmational diagnosis was made intraoperatively by an inguinoscrotal approach that revealed paratesticular lipoma. In our patient, there was no morbidity or long-term postsurgical sequelae. Excision of the tumor usually results in an uneventful recovery. The etiology of this condition is unknown, but a developmental origin has been proposed. All lipomas of the scrotum must be removed because of the possibility of their being converted into an aggressive neoplasm like liposarcoma [3, 4]. There have been very few reported cases of giant paratesticular lipoma. The entity of the giant lipoma is also a descriptive term, and further study on the behavior of this type of tumor is warranted.
No uniform classification exists; however, Leyson et al proposed classification of these tumors into two categories (paratesticular and extratesticular) according to their site of origin [5]. Paratesticular lipoma tumors include those that grow from the spermatic cord, epididymis, tunica vaginalis, and testicle. Extratesticular tumors are those that originate from preperitoneal or subperitoneal fat herniation, subserous fat around the inguinal ring, fasciae and transversalis muscles of the perineal area, perineum, and isolated fat lobules from subcutaneous tissues of the scrotal wall [5]. A lack of uniform classification makes it difficult to describe the number of cases in the literature; however, since only a few articles are reported, we consider paratesticular lipoma as a rare case. Diagnostic imaging has a role especially in differentiating between intratesticular and extratesticular lesions; however, pathological and microscopic examination of the lesion is still the gold standard for confirmational diagnosis. Inguinoscrotal exploration is recommended to evaluate the tumor. If the lesion is considered benign, simple enucleation will be proper. But if we consider malignant lesions, radical inguinal orchidectomy needs to be performed. Close follow-up needs to be performed to evaluate local relapse; none was seen in our case.
Intrascrotal paratesticular lipoma is sometimes difficult to diagnose because the clinical appearance of lipoma overlaps with that of other masses such as an omental hernia and hematoma. However, lipomas tend to be a well-defined echogenic mass, whereas a herniated omentum appears more elongated and should be traceable back to the inguinal area. Therefore, additional image evaluation plays an important role in the evaluation of these masses. In combination with clinical assessment, it can be indicated whether testis-sparing surgery is warranted.
The authors declare no competing interests.
All the authors contributed equally in the data collection and the drafting of the manuscript. All the authors read and agreed to the final manuscript.
All Author thank to 10th Malang Continuing Urology Education and Saiful Anwar Hospital for facilitating this article.
Figure 1: large right inguinoscrotal swelling
Figure 2: Doppler ultrasonography of right and left testes revealed an echo-heterogenic structure with normal vascularization without bowel appearance which was apart from the testis
Figure 3: macroscopic view of tumor
Figure 4: microscopic examination (mature benign lipomatous tissue with vascularization and minimal fibrous collagen tissue, suggestive of lipoma)
- Ahmed H, Rabindra KB, Niju P. Giant lipoma of the spermatic cord: a case report. Nat J Med Res. 2014; 4(2): 170-171. Google Scholar
- Veysel K, Hatice K, Izzet SP, Idil GT. Giant intrascrotal lipoma. BMJ case reports. 2013; (2013): bcr2013200500. PubMed | Google Scholar
- Konrad W. Surgical treatment giant spermatic cord lipoma. New Med. 2013; 17(2): 44-46. Google Scholar
- Ballas K, Rafailidis S, Symeonidis N, Triantaphyllou A et al. Retroperitoneal, mediastinal, and subcutaneous emphysema, complicating colonoscopy and rectal polypectomy. Journal of Laparoendoscopic & Advanced Surgical Techniques. 2007; 17(2): 1-3. PubMed | Google Scholar
- Florante J, Leyson J, Doroshow LW, Robbins MA. Extratesticular lipoma: report of 2 cases and a new classification. J Urol. 1976; 116(3): 324-32. PubMed | Google Scholar